by Jason Wasserman MD PhD FRCPC
July 13, 2022
What is a spermatocele?
A spermatocele is a non-cancerous fluid-filled space that develops in a part of the testicle called the epididymis. While most small spermatoceles will resolve on their own over time, large spermatoceles can cause pain and may need to be surgically removed.
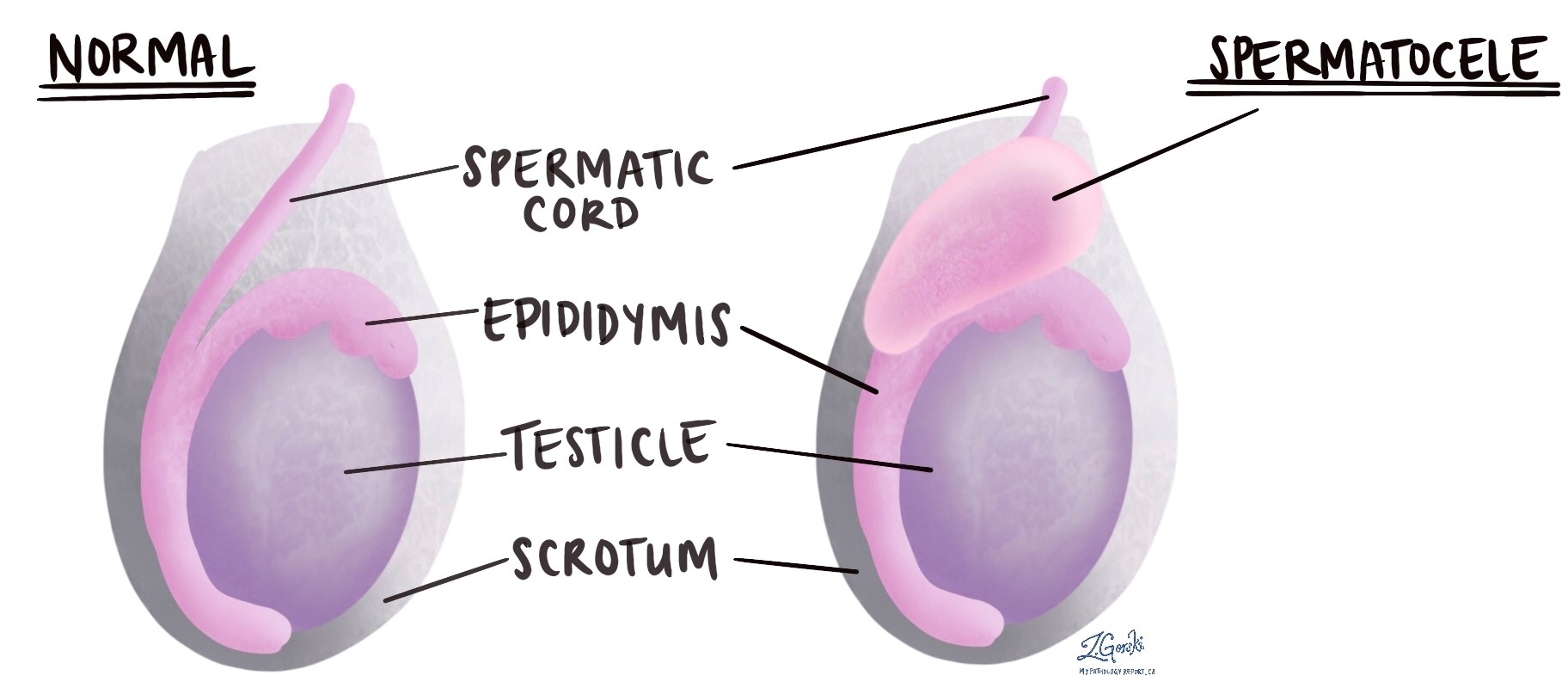
What causes a spermatocele?
For most patients, a cause is not identified. However, some spermatoceles may develop as a result of a blockage in one of the tubes that carry sperm out of the testis.
What are the symptoms of a spermatocele?
Most spermatoceles present as a painless lump in the scrotum adjacent to the testis.
Can a spermatocele turn into cancer over time?
No. A spermatocele cannot turn into cancer over time and it is not associated with an increased risk of developing testicular cancer.
How is the diagnosis of spermatocele made?
Your doctor may suspect that you have a spermatocele after performing a physical examination. During this examination, your doctor may shine a light on your scrotum. Because a spermatocele is filled with fluid, light can pass through it. Doctors describe this as ‘transillumination’. In contrast, a solid growth (such as a tumour) would not allow light through. Your doctor may also perform a test called an ultrasound. This test allows your doctor to see inside the scrotum. When examined by ultrasound, a spermatocele will appear as an open fluid-filled space called a cyst.
The diagnosis can also be made after the spermatocele is surgically removed and the tissue is sent to a pathologist for examination under the microscope.
What does a spermatocele look like when examined under the microscope?
When examined under the microscope, the spermatocele appears as an open space surrounded by a thin wall. The cells lining the wall are similar to those normally found in the epididymis. For example, cells with small finger-like projections called cilia are found in the normal epididymis and are commonly seen in a spermatocele. Sperm and fluid may be seen within the space in the center of the spermatocele.


