by Saleh Fadel MD and Bibianna Purgina MD FRCPC
November 19, 2023
Osteochondroma is the most common non-cancerous type of bone tumour. The name is made up of three parts that come from Greek words – “osteo-“meaning bone, “chondro-” meaning cartilage, and “-oma” which describes an abnormal growth. As the name suggests, the tumour is made up of both bone and cartilage.
Most osteochondromas develop in a part of the bone called the growth plate. Growth plates, also known as the “physis”, are present at the ends of bones, especially the long bones in our arms and legs. During childhood and puberty, these growth plates are responsible for our growth in height. When we are finished growing our growth plates close and eventually disappear. Osteochondromas are thought to grow from a piece of the growth plate that gets shifted due to trauma and continues to grow, along with the normal growth plate, and form an outgrowth of bone. The tumour also tends to stop growing when the person stops growing.
Osteochondromas can range in size from 1 cm to more than 20 cm, with the average size being 3 to 6 cm. The most common location is the edge of a long bone such as those found in the legs and arms and around the knees and elbows. However, this tumour can develop in any bone that is formed by cartilage. Because this type of tumour is associated with the growth plate it typically affects younger people with the average age being 21 years old.
What are the most common symptoms of osteochondroma?
Most osteochondromas do not cause any symptoms. Some patients notice a firm painless lump under their skin. When symptoms do occur, they vary depending on the size and location of the tumour. Larger tumours can cause muscle soreness, pressure, pain, or decreased movement. If the tumour presses on a nerve or blood vessel, it can lead to numbness/tingling, weakness, or colour change in the affected area. The most serious complication is a broken bone.
What genetic syndromes are associated with osteochondroma?
Most cases of osteochondromas are single and non-hereditary. Doctors describe these as sporadic because they have no known genetic cause. In contrast, multiple osteochondromas can be a manifestation of a genetic condition called hereditary multiple osteochondromas (or hereditary multiple exostoses).
How is this diagnosis made?
This diagnosis can be made after a small tissue sample is removed in a procedure called a biopsy or when the entire tumour is removed in a procedure called resection or curettage. The tissue is then sent to a pathologist for examination under the microscope. In some cases, the diagnosis can be made without a tissue examination because the appearance on imaging is unique (the tumour sticks out from the side of the bone).
What does an osteochondroma look like under the microscope?
Under the microscope, an osteochondroma resembles a disorganized growth plate. The outer layer has dense fibrous tissue with a cartilage cap. Usually, the cartilage cap is less than 1.0 cm. The specialized chondrocytes that make up the cartilage cap typically increase in amount and size in deeper layers. These cells look similar to the chondrocytes in normal cartilage. At the base of the growth plate, the tumour gives rise to newly formed bone by a process called endochondral ossification.
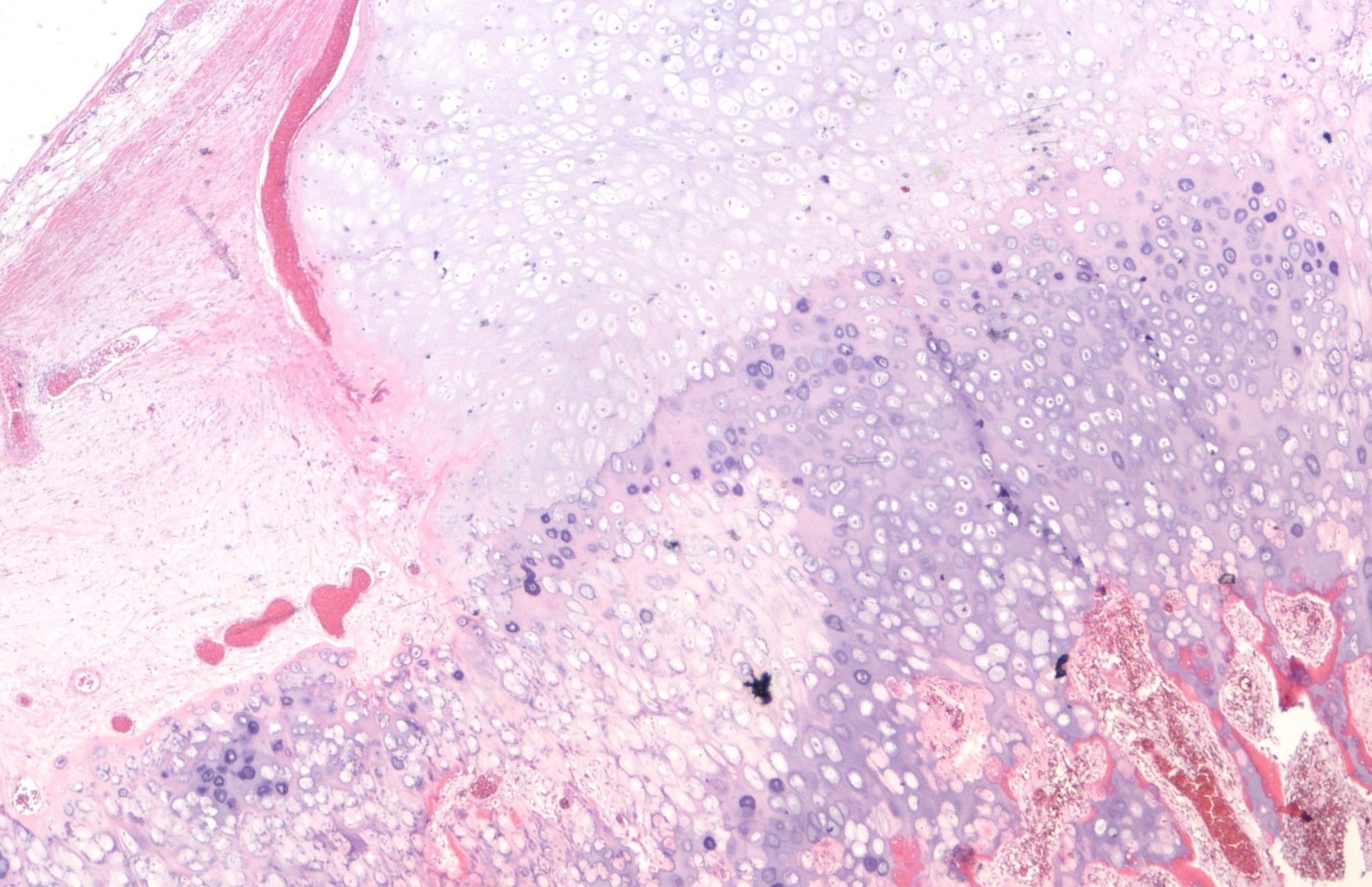
Can osteochondroma change into cancer over time?
In very rare cases a previously benign (noncancerous) osteochondroma will transform (change) into a malignant (cancerous) type of bone tumour called chondrosarcoma, When this happens the amount of cartilage in the osteochondroma will increase and the chondrocytes will look more abnormal. Pathologists use the word atypical to describe abnormal-looking cells. Your pathologist and radiologist will measure the cartilage cap that forms part of the osteochondroma. When an osteochondroma transforms into chondrosarcoma, the cartilage cap thickness is typically more than 2.0 cm.
What is the typical treatment for osteochondroma?
No treatment is necessary for single osteochondromas that are not causing any symptoms. These tumours are usually monitored with regular x-rays. If symptoms develop, which include pain, limitation of movement, or nerve or vessel impingement, then surgical removal is curative. Another indication for surgical removal is when the tumour grows in size quickly as this may indicate progression towards cancer, which is overall a very rare event. Even though surgical removal is curative, re-occurrence can happen when the lesion is not completely removed.
About this article
This article was written by doctors to help you read and understand your pathology report. Contact us if you have any questions about this article or your pathology report. Read this article for a more general introduction to the parts of a typical pathology report.


