Thyroglobulin is a protein made by the thyroid gland, a small butterfly-shaped gland located in the front of the neck. It plays an important role in producing thyroid hormones, which help regulate metabolism, energy levels, and body temperature.
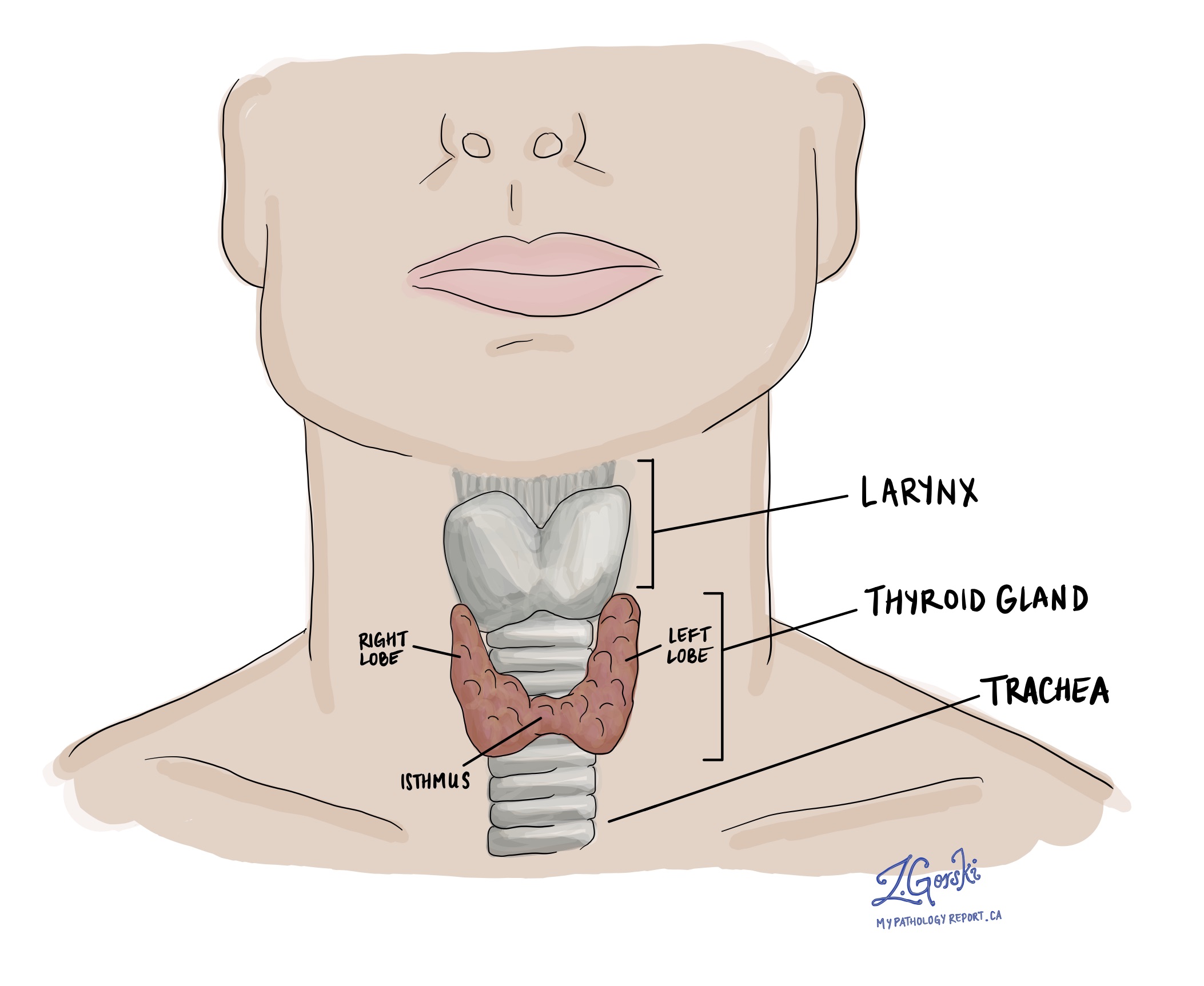
What does thyroglobulin do?
Thyroglobulin acts as a building block for thyroid hormones. Thyroglobulin stores and helps create two important hormones inside the thyroid gland: thyroxine (T4) and triiodothyronine (T3). These hormones control many bodily functions, including heart rate, digestion, and temperature regulation.
Where is thyroglobulin normally found?
Thyroglobulin is normally found inside the thyroid gland, where it is produced by specialized cells called follicular cells. These cells line small structures called thyroid follicles, which store thyroglobulin until it is needed to make thyroid hormones. In a healthy person, only a small amount of thyroglobulin enters the bloodstream, and its levels remain low.
How do doctors test for thyroglobulin?
Doctors test for thyroglobulin using a blood test. This test is often done for people who have had thyroid cancer or thyroid surgery to check for signs of cancer recurrence. Sometimes, the test is also used to evaluate other thyroid conditions. Another test called thyroglobulin antibody (TgAb) testing may be performed to check for antibodies that can interfere with the results.
What types of tumours produce thyroglobulin?
Tumours that come from thyroid follicular cells can produce thyroglobulin.
These include:
- Papillary thyroid carcinoma – The most common type of thyroid cancer.
- Follicular thyroid carcinoma – A less common but still significant type of thyroid cancer.
- Oncocytic carcinoma – A type of thyroid cancer made up of large, pink cells.
Because these tumours make thyroglobulin, measuring thyroglobulin levels can help doctors monitor for recurrence after treatment.
Immunohistochemistry for thyroglobulin
Immunohistochemistry is a special laboratory test that allows pathologists to see whether cells produce specific proteins. For thyroglobulin, this test is used to help determine if a tumour originated in the thyroid. A positive thyroglobulin immunohistochemistry test means that the tumour cells are making thyroglobulin, which confirms that the cancer came from the thyroid. This test is especially helpful when cancer has spread to other parts of the body, and doctors need to find out where it started. Thyroglobulin staining is usually strong and widespread in thyroid cancers that develop from follicular cells, such as papillary and follicular thyroid carcinoma.
What does a high thyroglobulin level mean?
A high thyroglobulin level can mean different things depending on the situation:
- In people with a healthy thyroid, slightly increased levels may be seen with thyroid inflammation (thyroiditis) or an overactive thyroid (hyperthyroidism).
- In people who have had thyroid cancer removed, rising thyroglobulin levels may suggest that cancer has returned.
- In rare cases, other thyroid conditions, such as benign thyroid nodules, may also cause increased thyroglobulin levels.
Doctors interpret thyroglobulin levels and other tests, such as imaging studies and additional blood tests, to determine the cause of an elevated level and whether further treatment is needed.


