October 25, 2023
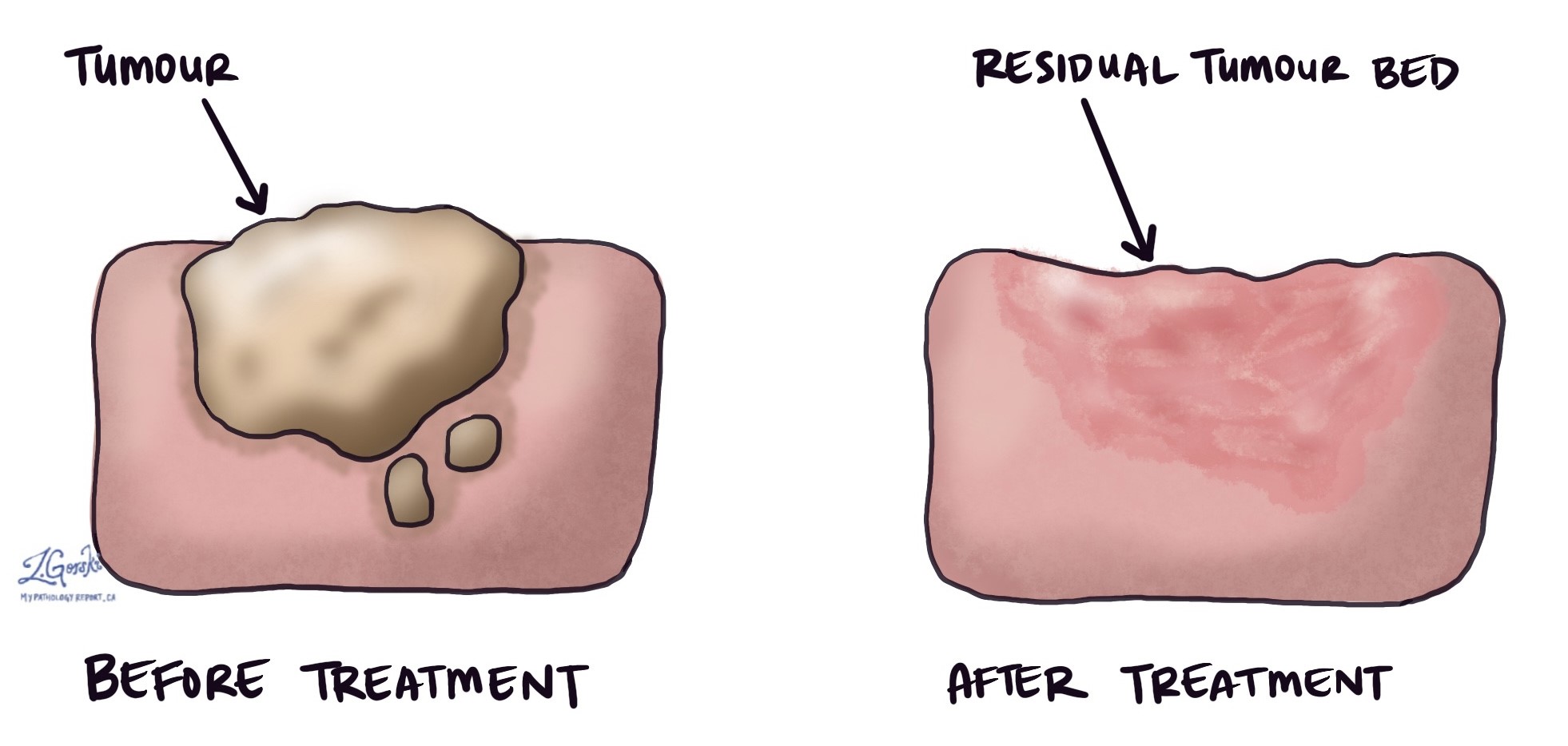
In pathology, the term tumour bed describes an area of the body where a tumour was located before it was removed by surgery or treated with chemotherapy, radiation therapy, or hormone therapy. It is important to examine the tumour bed because it can show how much of the tumour was killed by the treatment and how much of it remains. This can help to determine your prognosis and the need for further treatment. The amount of tissue available for examination depends on the type of cancer. For example, for some types of cancer, such as invasive ductal carcinoma of the breast, the entire tumour bed may be surgically removed and examined. However, for other types of cancer, such as adenocarcinoma of the esophagus, the tumour bed may be left in the body, but biopsies will be performed to look for the tumour bed and any remaining tumour cells.
What systems are used to measure the tumour bed?
Several different systems have been developed to measure the tumour bed. The system used depends on the type of tumour being examined and the location in the body. Here are two systems commonly used by pathologists today.
Tumour regression score
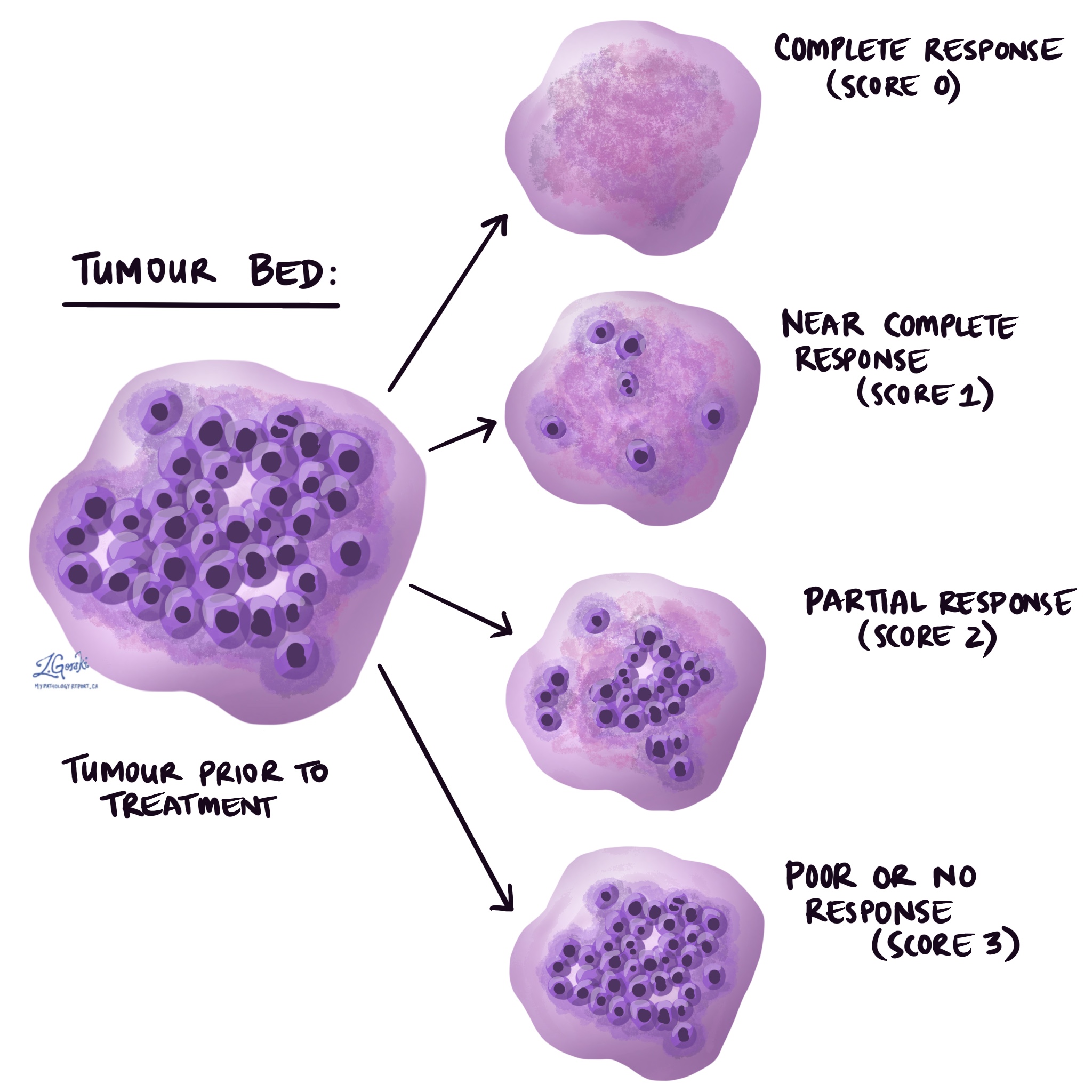
The tumour regression score (also known as the modified Ryan score) is the most commonly used system for measuring the tumour bed. Pathologists determine the tumour regression score by measuring the number of viable (living) tumour cells within the tumour bed. Using this measurement, the tumour regression score is divided into four categories: complete response (best outcome) to poor or no response (worst outcome).
The four categories of the tumour regression score are as follows:
- Complete response (score 0) – No viable (living) tumour cells are seen.
- Near complete response (score 1) – Rare or single viable (living) tumour cells are seen.
- Partial response (score 2) – More than rare or single viable (living) tumour cells are seen
- Poor or no response (score 3) – Large numbers of viable (living) tumour cells are seen.
Residual cancer burden
The residual cancer burden (RCB) system is used to measure the tumour bed for different types of breast cancer, including invasive ductal carcinoma and invasive lobular carcinoma.
Three variables are used to calculate the RCB:
- The size of the area containing viable (living) tumour cells. This measurement only includes areas with invasive cancer.
- The cellularity of the tumour cells (the number of tumour cells in a given area of tissue). Any non-invasive tumour cells are subtracted from this measurement.
- Tumour cells in a lymph node.
Using the above information, the RCB can be classified into four categories:
- RCB-0 (no residual cancer)
- RCB-I (minimal residual cancer)
- RCB-II (moderate residual cancer)
- RCB-III (extensive residual cancer)
The lower the RCB, the better the outcome. To learn more about the RCB score, visit the Residual Cancer Burden Calculator hosted by the MD Anderson Cancer Center.
What else do pathologists look for in the tumour bed?
The tumour bed can also show other relevant pathology features, such as the presence of in situ disease (cancer cells that have not invaded beyond their original site), fibrosis (scar tissue), necrosis (dead cells), and inflammation. These features can provide clues about the type, aggressiveness, and origin of the tumour, as well as its response to treatment.