by Jason Wasserman MD PhD FRCPC
November 16, 2025
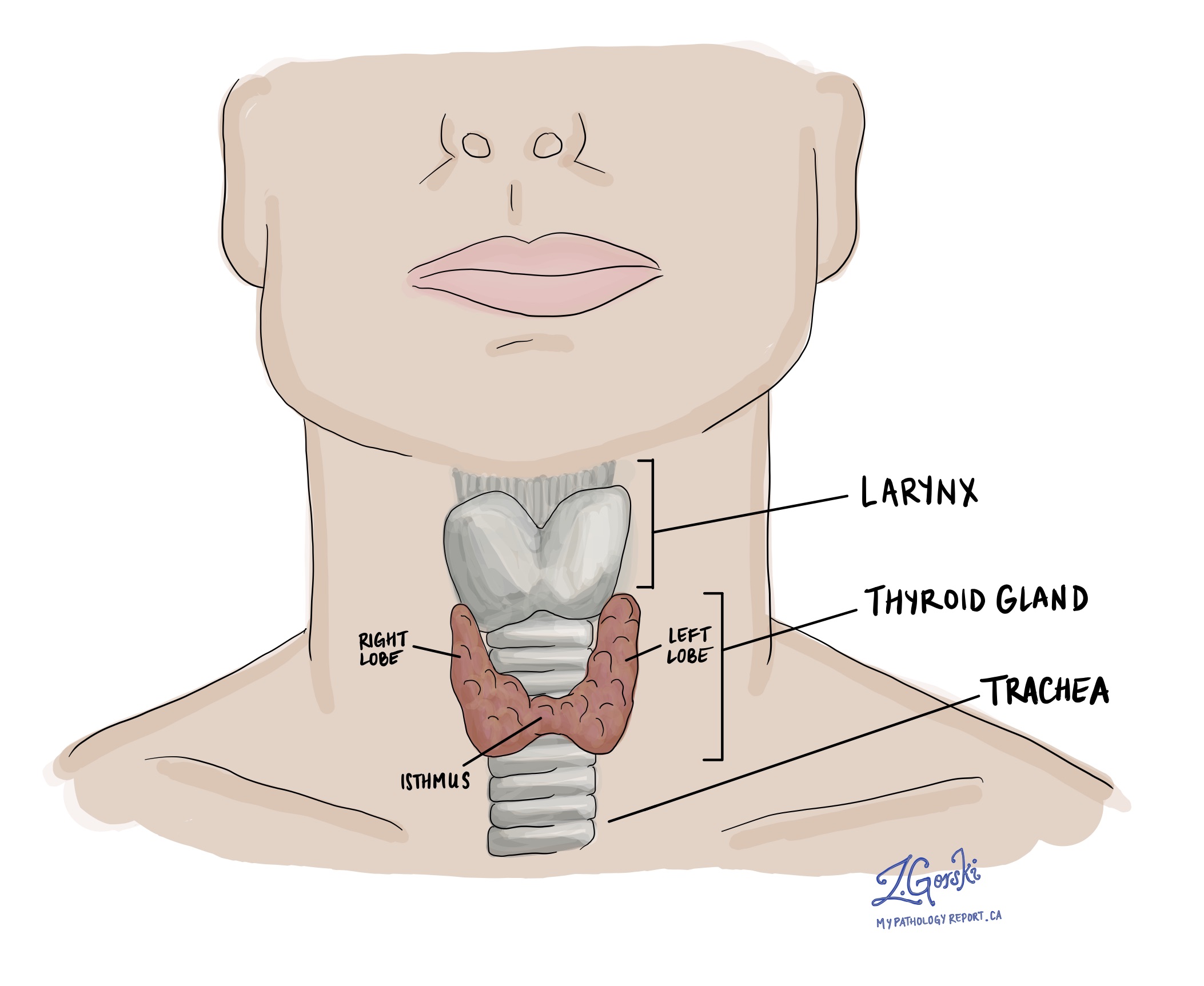
Papillary thyroid carcinoma is the most common type of thyroid cancer, accounting for approximately 80 percent of all cases. It starts in the follicular cells of the thyroid gland, which normally produce thyroid hormone. The thyroid is a butterfly-shaped gland at the front of the neck that plays an important role in regulating metabolism.
The term “papillary” describes how the tumour often looks under the microscope. Many tumours show tiny, finger-like projections of tissue called papillae. However, not all papillary thyroid carcinomas form obvious papillae, and some subtypes exhibit distinct growth patterns.
What are the symptoms of papillary thyroid carcinoma?
Many people with papillary thyroid carcinoma have no symptoms, and the tumour is found incidentally on imaging or during a routine neck examination. When symptoms are present, they may include a lump or swelling in the neck that can be seen or felt, changes in the voice such as hoarseness, and trouble swallowing or breathing if the tumour presses on nearby structures. Some patients may notice discomfort or a sense of fullness in the neck.
What causes papillary thyroid carcinoma?
The cause of papillary thyroid carcinoma is not fully understood. It appears to arise from a combination of genetic changes within thyroid cells and environmental risk factors.
Important risk factors include prior exposure to ionizing radiation (especially in childhood), iodine intake and other dietary influences, and a personal or family history of thyroid cancer. This cancer is more common in women and often occurs in younger adults compared to other thyroid cancers.
At the cellular level, papillary thyroid carcinoma develops when mutations in specific genes alter the growth and division of follicular cells. These changes allow cells to grow faster and with less control than normal, eventually forming a malignant tumour.
How is the diagnosis of papillary thyroid carcinoma made?
Diagnosis typically begins when a thyroid nodule is detected during a physical examination or on imaging studies, such as ultrasound.
Clinical examination and ultrasound
Your doctor will examine your neck for nodules and enlarged lymph nodes and may order a thyroid ultrasound to evaluate the area further. Ultrasound provides detailed information about the size, shape, and internal characteristics of the nodule, including whether it is solid or cystic and whether it exhibits suspicious features, such as microcalcifications or irregular margins.
Fine needle aspiration (FNA)
The next step is often a fine needle aspiration (FNA). In this procedure, a thin needle is inserted into the nodule under ultrasound guidance to remove cells for examination and analysis. An FNA is usually enough to make a diagnosis of papillary thyroid carcinoma because the tumour has characteristic nuclear features that can be recognized under the microscope.
However, FNA cannot reliably distinguish between benign and malignant follicular tumours. For those lesions, further surgery and histologic examination of the whole nodule are needed. In papillary thyroid carcinoma, FNA is often diagnostic, but final staging and evaluation of features such as extrathyroidal extension and vascular invasion require examination of the surgically removed thyroid tissue.
Surgical removal and microscopic examination
Once papillary thyroid carcinoma is suspected or confirmed by FNA, surgery is usually recommended. This may involve removing half of the thyroid (lobectomy) or the entire gland (total thyroidectomy), depending on tumour size, location, and risk factors.
After surgery, a pathologist examines the thyroid under the microscope. The biopsy or FNA allows the pathologist to identify papillary thyroid carcinoma based on its nuclear features. The resection specimen (surgical removal) enables the pathologist to:
-
Confirm the diagnosis and subtype.
-
Measure tumour size.
-
Determine whether there are multiple tumours (multifocal disease).
-
Assess extrathyroidal extension, vascular invasion, lymphatic invasion, and margin status.
-
Examine lymph nodes, if removed.
These findings are all described in your pathology report and used to stage the cancer and guide treatment.
Subtypes of papillary thyroid carcinoma
Not all papillary thyroid carcinomas are the same. The term “subtype” or “variant” is used to describe tumours that differ in microscopic appearance, behaviour, and sometimes response to treatment. Recognizing the subtype helps doctors predict how the cancer might behave and choose the most appropriate treatment plan.
Classic subtype
The classic subtype (also called the conventional subtype) is the most common form. It is characterized by papillae—finger-like projections lined by tumour cells—and by the characteristic nuclear features of papillary thyroid carcinoma. Tumour cells from this subtype commonly spread to lymph nodes in the neck.
Infiltrative follicular subtype
In the infiltrative follicular subtype, tumour cells grow in small circular groups called follicles, which can resemble normal thyroid follicles. Unlike invasive encapsulated follicular subtype papillary thyroid carcinoma, the infiltrative follicular subtype is not surrounded by a well-defined tumour capsule. It tends to infiltrate into the surrounding thyroid tissue.
Tall cell subtype
The tall cell subtype is more aggressive and often presents at a higher stage. The tumour cells are at least three times taller than they are wide and have the nuclear features of papillary thyroid carcinoma. This subtype is more common in older adults and is rarely seen in children. Tall cell tumours are more likely to extend beyond the thyroid and spread to lymph nodes.
Hobnail subtype
The hobnail subtype is an aggressive variant in which tumour cells appear to “hang off” the surface of papillae. These cells often have a hobnail shape, with bulging nuclei and a tapered base. The hobnail subtype tends to spread beyond the thyroid gland and can metastasize to lymph nodes and distant sites such as bone.
Solid/trabecular subtype
In the solid/trabecular subtype, tumour cells grow in solid nests or long cords (trabeculae) rather than papillae. This subtype is also considered more aggressive and has a higher risk of spreading to distant organs such as the lungs.
Oncocytic subtype
In the oncocytic subtype, tumour cells are larger than normal and appear bright pink under the microscope because they contain numerous mitochondria. These cells are called oncocytic or Hürthle cells. The prognosis for this subtype is generally similar to the classic subtype.
Diffuse sclerosing subtype
The diffuse sclerosing subtype is more common in children and young adults. It often involves both lobes of the thyroid (bilateral involvement) rather than a single nodule. This subtype shows extensive scarring (sclerosis), lymphocyte infiltration, and numerous small tumour foci. Compared to the classic subtype, it is more likely to spread beyond the thyroid and to distant sites.
Columnar subtype
The columnar subtype is a rare but aggressive variant. The tumour is composed of tall, column-shaped cells arranged in a pseudostratified pattern, meaning the nuclei appear layered, even though the cells are attached to the same base. This subtype is more likely to spread to lymph nodes and distant organs.
Biomarkers for papillary thyroid carcinoma
Papillary thyroid carcinoma often involves specific genetic changes that affect how tumour cells grow and respond to treatment. These are called biomarkers and are identified by specialized tests performed on tumour tissue.
Types of biomarker testing
The main types of tests used to identify biomarkers in papillary thyroid carcinoma include:
-
Tumour sequencing (NGS or PCR): Next-generation sequencing (NGS) or polymerase chain reaction (PCR) tests detect mutations and gene rearrangements in tumour DNA.
-
FISH (fluorescence in situ hybridization): Detects specific gene rearrangements or amplifications using fluorescent probes on tumour slides.
-
Immunohistochemistry (IHC): Uses antibodies to detect specific proteins whose presence may correlate with underlying genetic alterations.
Results are usually reported as “mutation detected,” “no mutation detected,” or as a specific fusion or rearrangement. The report may name the gene (for example, BRAF) and the exact mutation (such as V600E).
BRAF mutations
The BRAF gene encodes a protein involved in the MAPK signalling pathway, which helps regulate cell growth and division. The BRAF V600E mutation produces an abnormal protein that remains continuously active, leading to uncontrolled cell growth. BRAF V600E is one of the most common mutations in papillary thyroid carcinoma and is often associated with more aggressive disease, especially in variants such as tall cell and hobnail.
BRAF testing is typically performed using NGS or PCR on tumour tissue.
RET/PTC rearrangements
The RET gene encodes a receptor that sends growth signals into the cell. In papillary thyroid carcinoma, parts of the RET gene can become fused with other genes (RET/PTC rearrangements), resulting in the formation of an abnormal protein that sends continuous growth signals.
RET/PTC rearrangements are more common in patients with a history of radiation exposure and in children and young adults. They promote tumour growth via the same MAPK pathway and can be targeted by specific drugs in some cases.
RAS mutations
RAS genes (KRAS, NRAS, HRAS) encode proteins that help regulate cell division and growth. When mutated, RAS proteins can become permanently active and drive tumour development. RAS mutations are seen in a subset of papillary thyroid carcinomas and are more commonly associated with follicular-pattern tumours.
RAS mutations may influence prognosis and response to specific therapies and are detected by sequencing tests.
Tumour size
After the tumour is removed, it is measured in three dimensions. The largest dimension is recorded in your pathology report.
Tumour size is important because it helps determine the pathologic tumour stage (pT). Larger tumours are more likely to spread to lymph nodes or beyond the thyroid and may require more intensive treatment and follow-up.
Multifocal tumours
It is not unusual for more than one papillary thyroid carcinoma to be found in the same thyroid gland. Multifocal means more than one tumour of the same subtype is present.
If different subtypes are present, each tumour is described separately in the pathology report. When more than one tumour is found, the largest tumour is used to determine the pathologic tumour stage (pT), but the presence of multiple tumours can still be important for risk assessment and follow-up.
Extrathyroidal extension
Extrathyroidal extension refers to the growth of cancer cells beyond the thyroid gland into surrounding tissues.
Microscopic extrathyroidal extension
This type of extension is visible only under the microscope. It involves minimal spread through the thyroid capsule into nearby soft tissue.
Macroscopic (gross) extrathyroidal extension
This type is visible during surgery or on imaging. It involves an obvious invasion into neighbouring structures, such as the neck muscles, larynx (voice box), trachea (windpipe), esophagus (food pipe), or major blood vessels.
Macroscopic extrathyroidal extension is associated with a worse prognosis, leads to a higher tumour stage, and often results in more intensive treatment and closer follow-up.
Vascular invasion (angioinvasion)
Vascular invasion, also known as angioinvasion, refers to the presence of cancer cells within blood vessels outside the tumour. This finding is a marker of more aggressive disease.
Vascular invasion increases the risk that cancer cells will spread through the bloodstream to distant sites such as the lungs and bones. Its presence is associated with a higher risk of metastasis and may influence treatment decisions and follow-up planning.
Lymphatic invasion
Lymphatic invasion means cancer cells have entered lymphatic channels, which are tiny tubes that carry lymph fluid to lymph nodes. Papillary thyroid carcinoma commonly spreads through lymphatic vessels to the neck lymph nodes.
While lymphatic invasion suggests a higher chance of lymph node involvement, it is not always associated with a significantly worse prognosis in papillary thyroid carcinoma, especially in younger patients. It is still reported because it provides useful staging and risk information.
Margins
Margins refer to the edges of tissue removed during surgery. Pathologists examine these edges to see if cancer cells are present at or near the cut surface.
-
A negative margin means no cancer cells are seen at the edge, suggesting the tumour was completely removed.
-
A positive margin means cancer cells are present at the edge, suggesting that some tumour may remain.
Even with negative margins, the distance between the tumour and the nearest margin may be measured. Margin status helps determine whether additional treatment is needed and informs the risk of local recurrence.
Lymph nodes
Papillary thyroid carcinoma frequently spreads to lymph nodes in the neck.
Lymph nodes are small immune organs that filter lymph fluid. Cancer cells can travel from the thyroid through lymphatic vessels to nearby nodes. Nodes closest to the tumour are usually affected first.
Neck dissections
A neck dissection is a surgical procedure in which lymph nodes are removed from specific regions of the neck, known as levels 1 through 5. Lymph nodes on the same side as the tumour are called ipsilateral, while those on the opposite side are called contralateral.
How lymph nodes are described in the report
If lymph nodes are removed, the pathologist examines them under the microscope and reports:
-
The number of nodes examined.
-
The number of positive (involved) nodes.
-
The size of the largest tumour deposit.
-
Whether extranodal extension is present, meaning the tumour has grown beyond the lymph node capsule into surrounding tissue.
This information determines the nodal stage (pN) and helps estimate the risk of recurrence and spread, which in turn guides decisions about radioactive iodine therapy, radiation, or systemic treatment.
Pathologic stage (pTNM)
The pathologic stage for papillary thyroid carcinoma is determined after the entire tumour has been removed and examined. It includes tumour stage (pT), nodal stage (pN), and metastatic stage (pM). Most pathology reports provide details for pT and pN. Staging helps guide further treatment and estimate prognosis.
Tumour stage (pT)
-
T0: No evidence of primary tumour.
-
T1: Tumour 2 cm or smaller and confined to the thyroid.
-
T1a: Tumour 1 cm or smaller.
-
T1b: Tumour larger than 1 cm but not larger than 2 cm.
-
-
T2: Tumour larger than 2 cm but not larger than 4 cm and still confined to the thyroid.
-
T3: Tumour larger than 4 cm or showing minimal extension beyond the thyroid.
-
T3a: Tumour larger than 4 cm but still confined to the thyroid.
-
T3b: Tumour with gross extrathyroidal extension into neck muscles.
-
-
T4: Advanced disease with extensive local invasion.
-
T4a: Tumour extends into subcutaneous soft tissues, larynx, trachea, esophagus, or recurrent laryngeal nerve.
-
T4b: Tumour invades the prevertebral space and surrounds major blood vessels such as the carotid artery or mediastinal vessels.
-
Nodal stage (pN)
-
N0: No spread to regional lymph nodes.
-
N1: Spread to regional lymph nodes.
-
N1a: Metastasis to central neck lymph nodes (around the thyroid: pretracheal, paratracheal, prelaryngeal/Delphian, and perithyroidal).
-
N1b: Metastasis to other cervical (lateral neck) or superior mediastinal lymph nodes.
-
What happens after the diagnosis?
After diagnosis, your healthcare team will review your pathology report, imaging studies, thyroid function tests, and overall health to create a personalized treatment plan tailored to your specific needs. The team may include an endocrinologist, a thyroid surgeon, a nuclear medicine specialist, a radiation oncologist, and a medical oncologist.
Most patients are treated with surgery to remove the thyroid (total thyroidectomy) or the affected lobe (lobectomy). Depending on the stage and risk factors, additional treatments may include radioactive iodine, thyroid hormone suppression therapy, external beam radiation, or, in rare cases, systemic therapies in advanced cases.
Risk factors, such as tumour size, subtype, extrathyroidal extension, vascular invasion, lymph node involvement, and genetic alterations (for example, BRAF mutations), influence the choice of therapy.
After treatment, you will require regular follow-up, including blood tests (such as thyroglobulin in most non-oncocytic cases), ultrasound or other imaging, and clinical exams, to monitor for recurrence. Thyroid hormone replacement is usually required after total thyroidectomy. Lifestyle, long-term surveillance, and management of any treatment-related side effects are important parts of ongoing care.
Questions to ask your doctor
-
What subtype of papillary thyroid carcinoma do I have?
-
What did my pathology report say about tumour size, multifocality, and extrathyroidal extension?
-
Was there vascular invasion or lymphatic invasion?
-
Were surgical margins negative?
-
Were lymph nodes involved, and was there extranodal extension?
-
What is my pathologic stage (pT and pN)?
-
Were any genetic changes, such as BRAF, RET/PTC, or RAS mutations, identified, and do they affect my treatment?
-
Do I need radioactive iodine treatment?
-
How will my thyroid hormone levels and long-term health be monitored?
-
How often will I need follow-up visits and imaging?


