by Emily Goebel, MD FRCPC
April 28, 2023
What is squamous cell carcinoma of the vulva?
Squamous cell carcinoma (SCC) of the vulva is a type of cancer that starts from cells in the skin on the surface of the vulva.
What causes squamous cell carcinoma of the vulva?
SCC of the vulva commonly develops from one of two pre-cancerous diseases: high-grade squamous intraepithelial lesion (HSIL) or differentiated vulvar intraepithelial neoplasia (dVIN). HSIL is caused by infection with human papillomavirus (HPV). In contrast, dVIN is associated with prolonged chronic inflammation in the skin.
How do pathologists make the diagnosis of squamous cell carcinoma of the vulva?
The diagnosis of squamous cell carcinoma is usually made after a small tissue sample is removed in a procedure called a biopsy. The entire tumour is usually then removed in a procedure called an excision or resection.
What does it mean if squamous cell carcinoma of the vulva is described as well, moderately, or poorly differentiated?
Pathologists divide squamous cell carcinoma of the vulva into three grades – well, moderately, and poorly differentiated – based on how much the tumour cells look like normal squamous cells when examined under the microscope. The grade is important because higher grade tumours (moderately and poorly differentiated tumours) behave in a more aggressive manner and are more likely to spread to other parts of the body.
Squamous cell carcinoma of the vulva is graded as follows:
- Well differentiated squamous cell carcinoma of the vulva– A well differentiated tumour (also known as grade 1) is made up of tumour cells that look almost the same as normal squamous cells.
- Moderately differentiated squamous cell carcinoma of the vulva – A moderately differentiated tumour (also known as grade 2) is made up of tumour cells that clearly look different from normal squamous cells, however, they can still be recognized as squamous cells.
- Poorly differentiated squamous cell carcinoma of the vulva – A poorly differentiated tumour (also known as grade 3) is made up of tumour cells that look very little like normal squamous cells. These cells can look so abnormal that your pathologist may need to order an additional test such as immunohistochemistry to confirm the diagnosis.

Why is the tumour size important?
After the entire tumour has been removed, your pathologist will measure it in three dimensions and the largest dimension will be described in your pathology report. The size of the tumour is important because it is used to determine the pathologic tumour stage (pT).
What does the depth of invasion mean and why is it important?
Squamous cell carcinoma of the vulva starts in a thin layer of tissue on the surface of the vulva called the epidermis. Depth of invasion is a measurement of how far the tumour cells have spread from the epidermis into the layers of tissue below (the dermis and subcutaneous tissue). For vulvar tumours, the depth of invasion is measured from the surface of the skin to the deepest point of invasion. Some pathology reports describe the depth of invasion as tumour thickness. Tumours that grow deeper into the dermis are more likely to spread to a lymph node or to grow back after treatment.
What does lymphovascular invasion mean and why is it important?
Lymphovascular invasion means that cancer cells were seen inside a blood vessel or lymphatic vessel. Blood vessels are long thin tubes that carry blood around the body. Lymphatic vessels are similar to small blood vessels except that they carry a fluid called lymph instead of blood. The lymphatic vessels connect with small immune organs called lymph nodes that are found throughout the body. Lymphovascular invasion is important because cancer cells can use blood vessels or lymphatic vessels to spread to other parts of the body such as lymph nodes or the lungs.

What is a margin and why are margins important?
A margin is any tissue that was cut by the surgeon in order to remove the tumour from your body. Whenever possible, surgeons will try to cut tissue outside of the tumour to reduce the risk that any tumour cells will be left behind after the tumour is removed.
Your pathologist will carefully examine all the margins in your tissue sample to see how close the tumour cells are to the edge of the cut tissue. Margins will only be described in your report after most or all of the tumour has been removed.
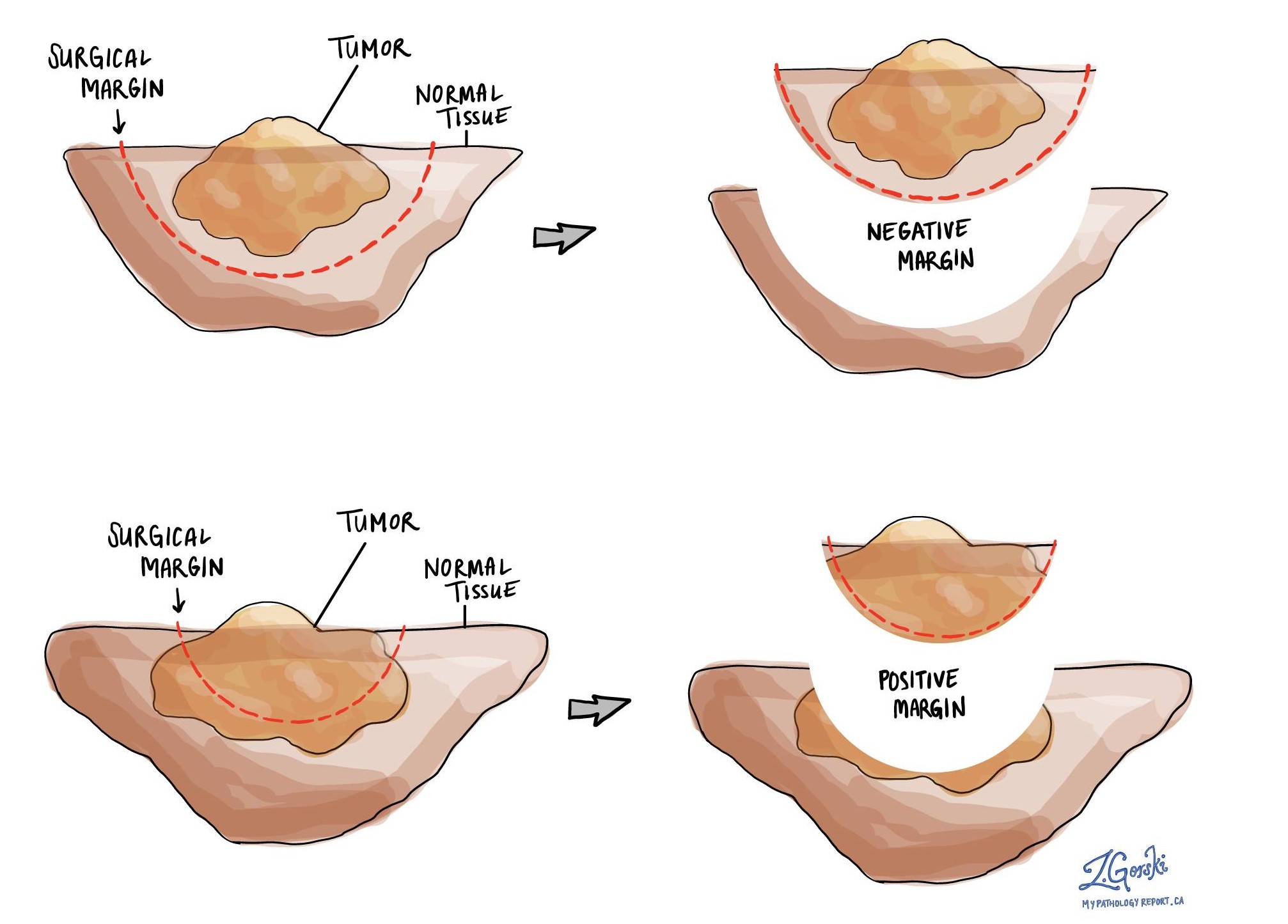
A negative margin means there were no tumour cells at the very edge of the cut tissue. If all the margins are negative, most pathology reports will say how far the closest tumour cells were to a margin. The distance is usually described in millimetres. A margin is considered positive when there are tumour cells at the very edge of the cut tissue. If HSIL or dVIN are seen at the margin that will also be described in your report. A positive margin increases the risk that the tumour will grow back in that location.
What is the pathologic stage (pTNM) for squamous cell carcinoma of the vulva?
The pathologic stage for squamous cell carcinoma of the vulva is based on the TNM staging system, an internationally recognized system originally created by the American Joint Committee on Cancer. This system uses information about the primary tumour (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathologic stage (pTNM). Your pathologist will examine the tissue submitted and give each part a number. In general, a higher number means a more advanced disease and a worse prognosis.
Tumour stage (pT) for squamous cell carcinoma of the vulva
Squamous cell carcinoma is given a tumour stage between 1 and 3. Your pathologist will look for three features in order to determine the tumour stage:
1. The size of the tumour.
2. Depth of invasion.
3. Tumor extension into nearby tissues including the urethra, vagina, bladder or rectum.
Nodal stage (pN) for squamous cell carcinoma of the vulva
Squamous cell carcinoma is given a nodal stage of 0 or 3 based on the number of lymph nodes with tumour cells and the size of the largest tumour deposit in the lymph node. If no tumour cells are seen in any of the lymph nodes examined, the nodal stage is N0. Lymph nodes with isolated tumour cells are also given a nodal stage of N0. If no lymph nodes are submitted for pathological examination, the nodal stage cannot be determined and the nodal stage is listed as NX.
Metastatic stage (pM) for squamous cell carcinoma of the vulva
Squamous cell carcinoma is given a metastatic stage of 0 or 1 based on the presence of tumour cells at a distant site in the body (for example the lungs). The metastatic stage can only be assigned if tissue from a distant site is submitted for pathological examination. Because this tissue is rarely present, the metastatic stage cannot be determined and is listed as MX.



