by Jason Wasserman MD PhD FRCPC
May 22, 2025
Low-grade endometrial stromal sarcoma is a type of cancer that arises from the stroma, a supportive tissue within the uterus. It is called “low-grade” because the cancer cells grow slowly and resemble normal endometrial stromal cells, which are typically found in the lining of the uterus. Despite its slow growth, it can spread into the muscle layer of the uterus (myometrium) and sometimes into blood vessels or lymphatic vessels.
What causes low grade endometrial stromal sarcoma?
The exact cause of low grade endometrial stromal sarcoma is unknown. However, some factors may increase the risk, such as long-term exposure to estrogen, use of medications like tamoxifen (often used to treat breast cancer), and previous pelvic radiation therapy. Many cases are associated with genetic changes called gene fusions involving genes like JAZF1 and SUZ12, among others.
What are the symptoms of low grade endometrial stromal sarcoma?
Common symptoms include abnormal vaginal bleeding, pelvic pain or discomfort, and a noticeable uterine mass. In some cases, low-grade endometrial stromal sarcoma might be detected only after it has spread to other parts of the body, such as the lungs or lymph nodes, causing additional symptoms related to these areas.
What is the difference between low grade and high grade endometrial stromal sarcoma?
The main difference between low grade and high grade endometrial stromal sarcoma lies in how the cancer cells appear and behave. Low-grade tumors grow slowly and have cells that closely resemble normal uterine stromal cells. High grade tumors grow more quickly, appear very abnormal under the microscope, and typically have a more aggressive course with a higher risk of spreading to other parts of the body.
How is this diagnosis made?
The diagnosis is typically made after examining a tissue sample under a microscope. Tissue samples are usually obtained during surgery or a biopsy. A pathologist examines the tissue, looking for characteristic patterns of tumor cells infiltrating the uterine muscle and blood vessels.
What other tests may be performed to confirm the diagnosis?
Additional tests may include immunohistochemistry, a method used to detect specific proteins in the tumor cells. Common markers for low-grade endometrial stromal sarcoma include CD10, estrogen receptor (ER), progesterone receptor (PR), and cyclin D1. Molecular testing can also be performed to identify specific genetic fusions like JAZF1-SUZ12, which helps confirm the diagnosis.
Tumour extension
Low grade endometrial stromal sarcoma often extends into different layers of the uterine wall. The uterus consists of three layers: the inner lining (endometrium), the muscular middle layer (myometrium), and the outer layer (serosa). Initially, the tumor arises from the endometrial stromal tissue and can invade into the myometrium and potentially through the serosa into surrounding pelvic tissues. In advanced cases, it may spread to adjacent pelvic organs such as the ovaries, fallopian tubes, bladder, rectum, or other abdominal tissues.
Margins
Margins refer to the edges of the tissue removed during surgery. Margins are classified as either positive or negative based on whether cancer cells are present:
- Positive margins: Cancer cells are present at the edge of the tissue, indicating that not all of the tumor was removed.
- Negative margins: No cancer cells are present at the edge, indicating complete removal.
Positive margins suggest a higher likelihood of tumor recurrence and might necessitate additional treatment, such as further surgery or radiation. Negative margins indicate that the tumor was successfully and fully removed, decreasing the risk of recurrence.
Types of margins commonly assessed in uterine surgery include:
- Endocervical margin: This is the connection between the uterus and cervix.
- Ectocervical margin: This refers to the outer portion of the cervix.
- Parametrial margin: This includes the connective tissue surrounding the uterus.
- Vaginal margin: This applies if part of the vagina is also surgically removed.

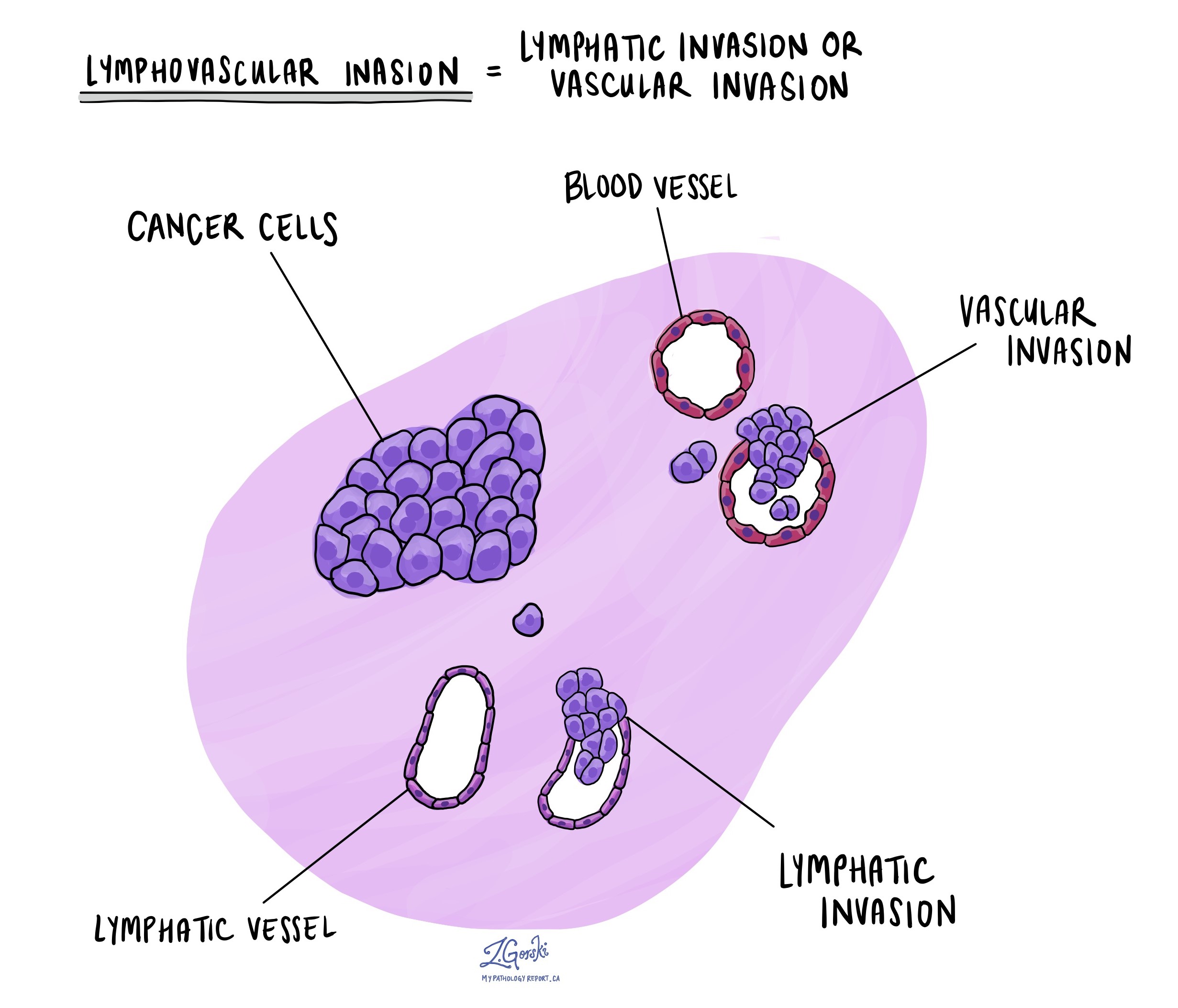
Lymphovascular invasion
Lymphovascular invasion refers to the presence of tumor cells within blood vessels or lymphatic vessels. If present, this indicates that the tumor cells have a higher potential for spreading to other parts of the body and may require more aggressive monitoring or treatment.
AJCC stage
The American Joint Committee on Cancer (AJCC) staging system uses categories to describe the extent of tumor spread:
- T category: Describes the size and extent of the tumor in the uterus and surrounding tissues.
- T1: Tumor limited to the uterus (further subdivided by tumor size).
- T2: Tumor extends beyond the uterus but within the pelvis.
- T3: Tumor infiltrates abdominal tissues.
- T4: Tumor invades the bladder or rectum.
- N category: Indicates whether the cancer has spread to lymph nodes.
- N0: No lymph node spread.
- N1: Spread to regional lymph nodes.
- M category: Indicates distant spread beyond the pelvis.
- M0: No distant spread.
- M1: Cancer has spread to distant organs (e.g., lungs).
FIGO stage
The International Federation of Gynecology and Obstetrics (FIGO) staging system provides a clinical staging approach:
- Stage I: Tumor limited to the uterus.
- IA: Tumor size ≤5 cm.
- IB: Tumor size >5 cm.
- Stage II: Tumor extends beyond the uterus, within the pelvis.
- IIA: Involves the ovaries or fallopian tubes.
- IIB: Involves other pelvic tissues.
- Stage III: Tumor invades abdominal tissues or lymph nodes.
- IIIA: Invasion at one site.
- IIIB: Invasion at multiple sites.
- IIIC: Spread to lymph nodes.
- Stage IV: Tumor invades bladder/rectum or distant organs.
- IVA: Invades bladder or rectum.
- IVB: Distant metastasis.
What is the prognosis for someone diagnosed with low grade endometrial stromal sarcoma?
Low grade endometrial stromal sarcoma typically has a good prognosis, especially when diagnosed at an early stage. The five-year survival rate is greater than 90% for early-stage disease (stages I and II). However, if the tumor has spread beyond the uterus (stages III and IV), the survival rate decreases to around 50%. Even though this cancer grows slowly, careful monitoring and treatment are important because recurrence can occur many years after the initial treatment.
Questions to ask your doctor
- What stage is my low grade endometrial stromal sarcoma?
- What treatments are available, and what do you recommend?
- How often should I have follow-up appointments or tests?
- What symptoms should I watch out for after treatment?
- Should my family members consider any genetic testing?
- Are there lifestyle changes or precautions I should take?