by Jason Wasserman MD PhD FRCPC
September 28, 2022
What is minimally invasive oncocytic carcinoma?
Minimally invasive oncocytic cell carcinoma is a type of thyroid cancer. The tumour is separated from the normal thyroid gland by a thin band of tissue called a tumour capsule. In a “minimally invasive” tumour, groups of cancer cells have broken through the tumour capsule and spread into the surrounding normal thyroid gland. This type of cancer was previously called minimally invasive Hurthle cell carcinoma.
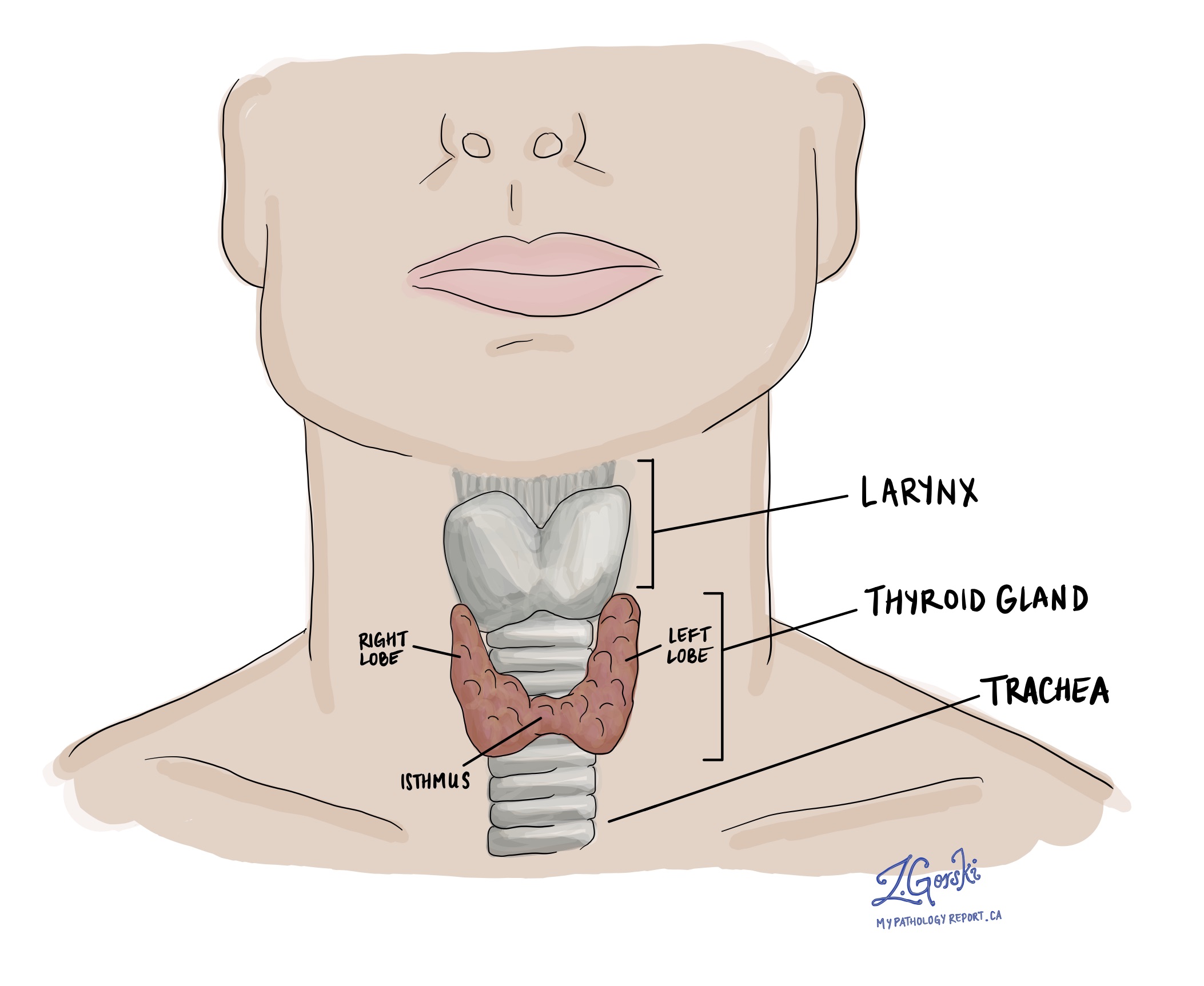
How is minimally invasive oncocytic carcinoma diagnosed?
The diagnosis can only be made after the entire tumour is removed and sent to a pathologist for examination. This usually involves surgically removing one lobe of the thyroid gland although sometimes the entire thyroid gland is removed. The tumour needs to be removed because the entire tumour capsule needs to be examined under the microscope to look for tumour capsule invasion. Tumour capsule invasion means that cancer cells have broken through the tumour capsule and have spread into the surrounding normal thyroid gland. An oncocytic adenoma is a type of non-cancerous thyroid tumour that looks very similar to minimally invasive oncocytic carcinoma. However, in contrast to minimally invasive oncocytic carcinoma, the tumour cells in a oncocytic adenoma have not broken through the capsule and spread into the surrounding thyroid gland.
What does minimally invasive oncocytic carcinoma look like under the microscope?
When examined under the microscope the tumour is made up of large pink oncocytic cells. Until very recently, these cells were called Hurthle cells. Oncocytic cells appear pink because the cytoplasm (body of the cell) is full of a cellular part called mitochondria. Oncocytic cells also have a large round nucleus (the part of the cell that holds the genetic material) and a prominent central nucleolus (a clump of genetic material in the middle of the nucleus). The oncocytic cells can connect together to form small round structures called follicles or they may be in large groups that pathologists describe as a ‘solid pattern’.
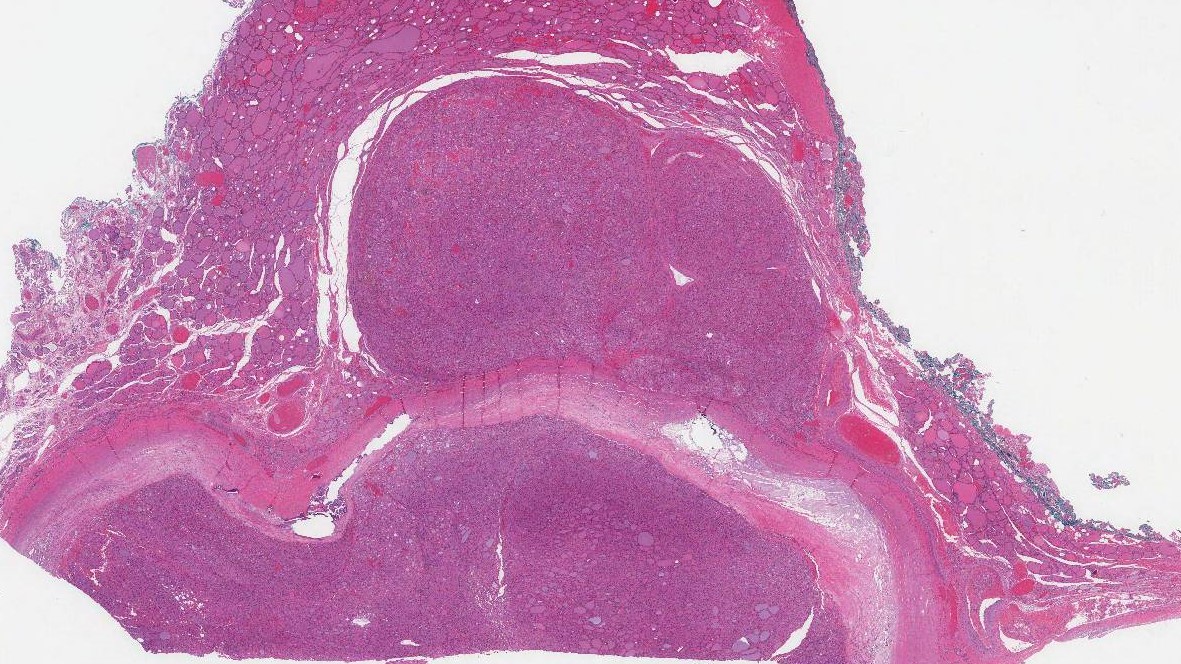
Why is this tumour called minimally invasive?
Oncocytic carcinoma is called “minimally invasive” when only some of the cancer cells have broken through the tumour capsule and spread into the surrounding normal thyroid gland. This is different from a related type of cancer called widely invasive oncocytic carcinoma where very little or no tumour capsule is seen and most of the cancer cells have spread into the surrounding normal thyroid gland.
Why is the tumour size important?
After the entire tumour is removed, it will be measured and the size of the tumour will be included in your pathology report. The size of the tumour is important because it is used to determine the pathologic tumour stage (pT) and because larger tumours are more likely to spread to other parts of the body.
What is angioinvasion (vascular invasion)?
Angioinvasion (vascular invasion) means that cancer cells were seen inside a blood vessel. In order to make the diagnosis of minimally invasive oncocytic carcinoma, your pathologist should not see angioinvasion (vascular invasion). If angioinvasion (vascular invasion) is seen, the tumour should be diagnosed as encapsulated angioinvasive oncocytic carcinoma.
What is lymphatic invasion?
Lymphatic invasion means that cancer cells were seen inside a lymphatic vessel. Lymphatic vessels are small thin channels that allow waste, extra fluid, and cells to leave a tissue. Lymphatics are found all over the body. Lymphatic invasion is important because it increases the risk that cancer cells will be found in a lymph node. Lymphatic invasion is not commonly seen in minimally invasive oncocytic carcinoma.
What is extrathyroidal extension?
Extrathyroidal extension means that cancer cells have spread beyond the thyroid gland and into the surrounding tissues. Cancer cells that move far enough out of the thyroid gland may come into contact with other organs such as muscles, the esophagus, or the trachea.
There are two types of extrathyroidal extension:
- Microscopic – The cancer cells outside of the thyroid gland were only found after the tumour was examined under the microscope.
- Macroscopic (gross) – The tumour can be seen growing into the surrounding tissues without the use of a microscope. This type of extrathyroidal extension may be seen by your surgeon at the time of surgery or by the pathologist assistant performing the gross examination of the tissue sent to pathology.
Macroscopic (gross) extrathyroidal extension is important because it increases the pathologic tumour stage (pT) and is associated with a worse prognosis. In contrast, microscopic extrathyroidal extension does not change the tumour stage and is not associated with a worse prognosis.
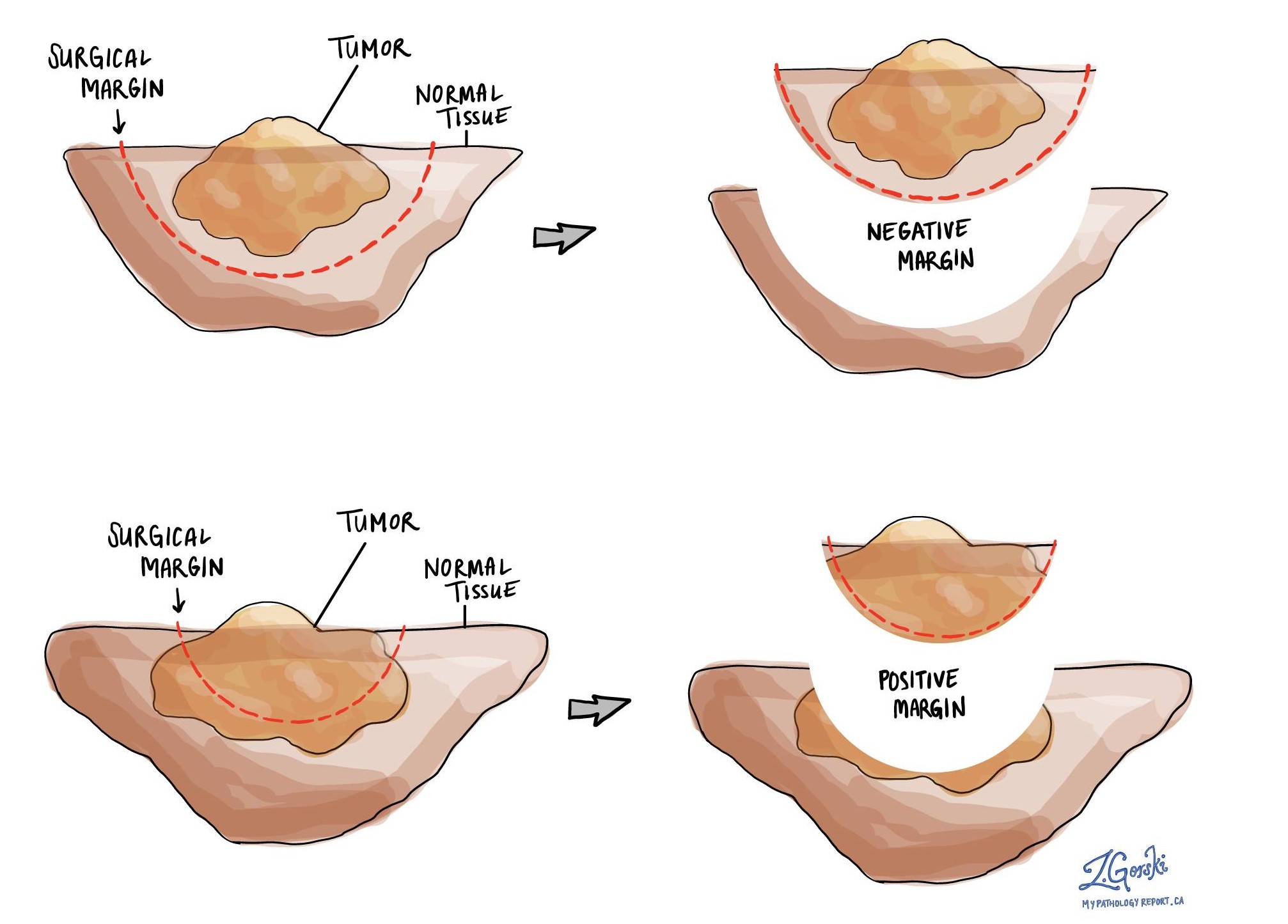
What is a margin?
A margin is any tissue that has to be cut by the surgeon in order to remove the thyroid gland from your body. A margin is considered positive when there are cancer cells at the very edge of the cut tissue. A negative margin means there were no cancer cells seen at the cut edge of the tissue.
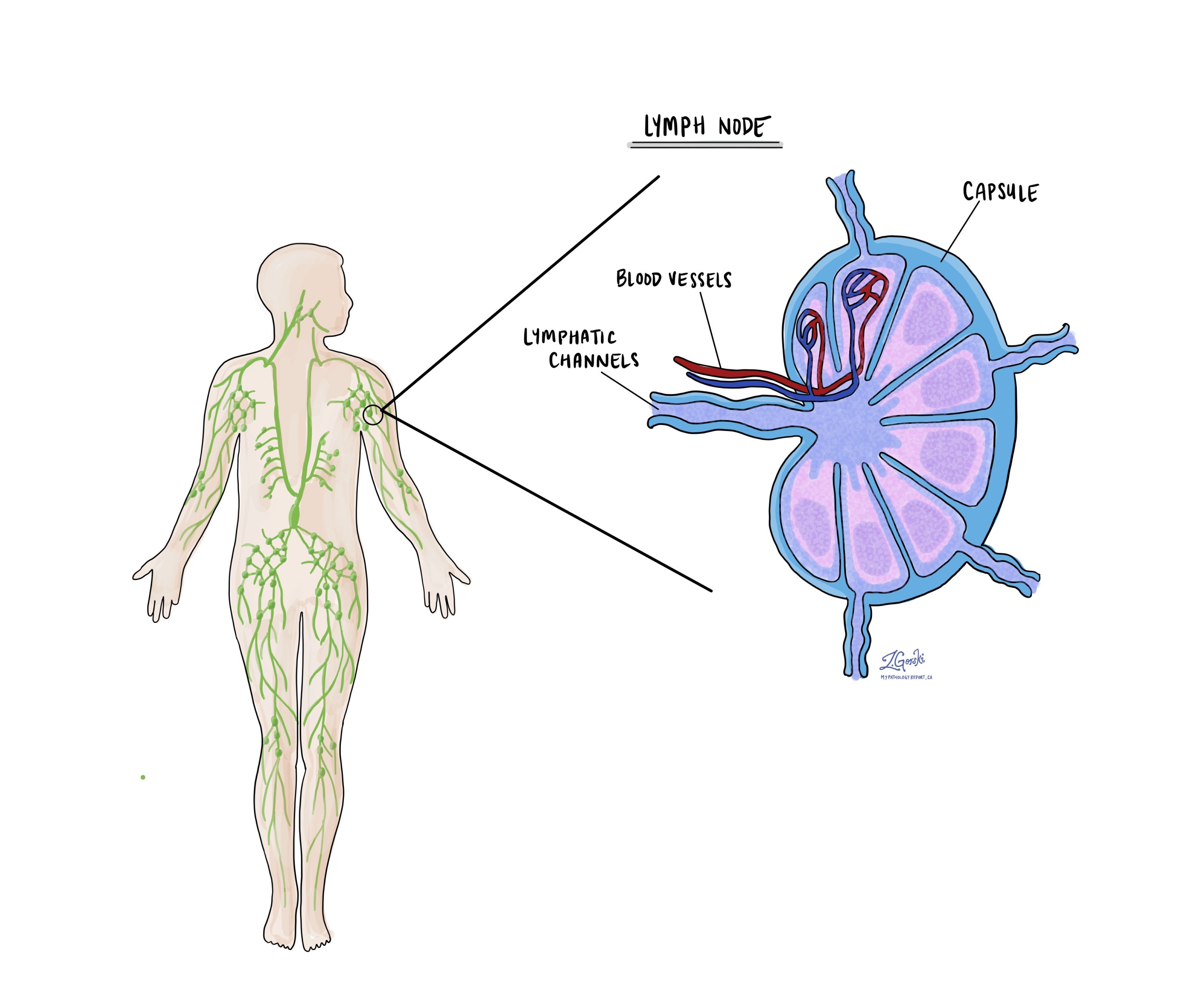
Were lymph nodes examined and did any contain cancer cells?
Lymph nodes are small immune organs located throughout the body. Cancer cells can travel from the thyroid to a lymph node through lymphatic channels located in and around the tumour (see Lymphatic invasion above). The movement of cancer cells from the thyroid to a lymph node is called metastasis. Minimally invasive oncocytic carcinoma is less likely than other types of thyroid cancer to spread to lymph nodes.
Lymph nodes from the neck are sometimes removed at the same time as the thyroid in a procedure called a neck dissection. The lymph nodes removed usually come from different areas of the neck and each area is called a level. The levels in the neck are numbered 1 through 7. Your pathology report will often describe how many lymph nodes were seen in each level sent for examination. Lymph nodes on the same side as the tumour are called ipsilateral while those on the opposite side of the tumour are called contralateral.
Your pathologist will carefully examine each lymph node for cancer cells. Lymph nodes that contain cancer cells are often called positive while those that do not contain any cancer cells are called negative. Most reports include the total number of lymph nodes examined and the number, if any, that contain cancer cells.
What is a tumour deposit?
A group of cancer cells inside of a lymph node is called a tumour deposit. If a tumour deposit is found, your pathologist will measure the deposit and the largest tumour deposit found will typically be described in your report.
What is extranodal extension (ENE)?
All lymph nodes are surrounded by a thin layer of tissue called a capsule. Extranodal extension (ENE) means that cancer cells have broken through the capsule and spread into the tissue that surrounds the lymph node.
How is the pathologic stage (pTNM) for minimally invasive oncocytic carcinoma determined?
The pathologic stage for minimally invasive oncocytic carcinoma is based on the TNM staging system, an internationally recognized system originally created by the American Joint Committee on Cancer. This system uses information about the primary tumour (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathologic stage (pTNM). Your pathologist will examine the tissue submitted and give each part a number. In general, a higher number means more advanced disease and a worse prognosis.
Tumour stage (pT) for minimally invasive oncocytic carcinoma
Minimally invasive oncocytic carcinoma is given a tumour stage between 1 and 4 based on the size of the tumour and the presence of cancer cells outside of the thyroid.
- T1 – The tumour is less than or equal to 2 cm and the cancer cells do not extend beyond the thyroid gland.
- T2 – The tumour is greater than 2 cm but less than or equal to 4 cm and the cancer cells do not extend beyond the thyroid gland.
- T3 – The tumour is greater than 4 cm OR the cancer cells extend into the muscles outside of the thyroid gland.
- T4 – The cancer cells extend to structures or organs outside of the thyroid gland including the trachea, larynx, or esophagus.
Nodal stage (pN) for minimally invasive oncocytic carcinoma
Minimally invasive oncocytic carcinoma is given a nodal stage of 0 or 1 based on the presence or absence of cancer cells in a lymph node and the location of the involved lymph nodes.
- N0 – No cancer cells were found in any of the lymph nodes examined.
- N1a – Cancer cells were found in one or more lymph nodes from levels 6 or 7.
- N1b – Cancer cells were found in one or more lymph nodes from levels 1 through 5.
- NX – No lymph nodes were sent to pathology for examination.
Metastatic stage (pM) for minimally invasive oncocytic carcinoma
Minimally invasive oncocytic carcinoma is given a metastatic stage of 0 or 1 based on the presence of tumour cells at a distant site in the body (for example the lungs). The metastatic stage can only be determined if tissue from a distant site is sent for pathological examination. Because this tissue is rarely sent, the metastatic stage cannot be determined and is listed as MX.



