by Jason Wasserman MD PhD FRCPC
September 13, 2023
What is uterine leiomyosarcoma?
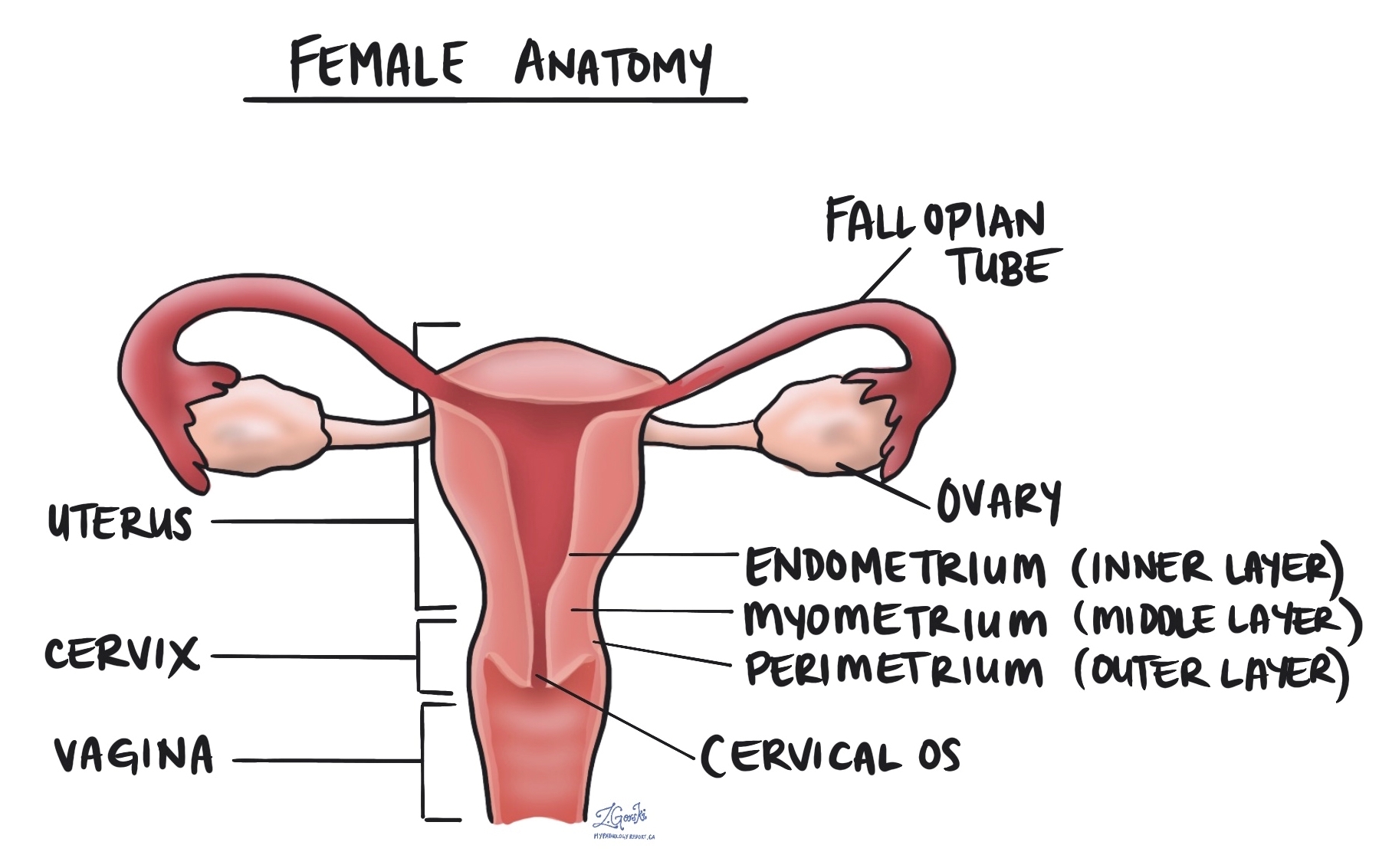
Uterine leiomyosarcoma is a type of uterine cancer. The tumour starts from specialized smooth muscle cells normally found in a part of the uterus called the myometrium. Most patients are over the age of 50 years at the time of diagnosis.
What are the symptoms of uterine leiomyosarcoma?
Symptoms of uterine leiomyosarcoma include vaginal bleeding, abdominal pain or pressure, and bloating.
What causes uterine leiomyosarcoma?
Prior radiation therapy to the pelvis is associated with an increased risk of developing uterine leiomyosarcoma. However, for most women who develop leiomyosarcoma, the cause is unknown.
How is the diagnosis of uterine leiomyosarcoma made?
The diagnosis of uterine leiomyosarcoma is usually made after the entire uterus is removed in a procedure called a hysterectomy. The ovaries and cervix may be removed at the same time. Most tumours are found in a part of the uterus called the body or corpus. However, these tumours can also start in the wall of the cervix. The uterus and any other organs or tissues removed are then sent to a pathologist for microscopic examination.
What does a uterine leiomyosarcoma look like under the microscope?
When examined under the microscope, most uterine leiomyosarcomas are made up of long thin smooth muscle cells. Because of their shape, pathologists often describe these cells as spindle cells. These same smooth muscle cells are also found in a non-cancerous type of tumour called a leiomyoma. In order to tell the difference between leiomyosarcoma and leiomyoma, your pathologist will look for the following three histologic features:
- Dividing tumour cells – Tumour cells divide in order to create new cells. This process is called mitosis. A cell that is in the process of dividing is called a mitotic figure. Dividing tumour cells are typically found in leiomyosarcoma. In contrast, very few dividing cells should be found in a non-cancerous leiomyoma.
- Abnormal-looking tumour cells – Pathologists use the terms atypical or atypia to describe cells that are abnormal-looking in shape, size, or colour. Atypical tumour cells are commonly found in leiomyosarcoma.
- Dead or dying tumour cells – Cancers grow more quickly than non-cancerous tumours. As they grow, the tumour cells run out of energy and die. This kind of cell death is called necrosis. Necrosis may be seen in leiomyosarcoma. However, it is rare to see necrosis in a non-cancerous leiomyoma.
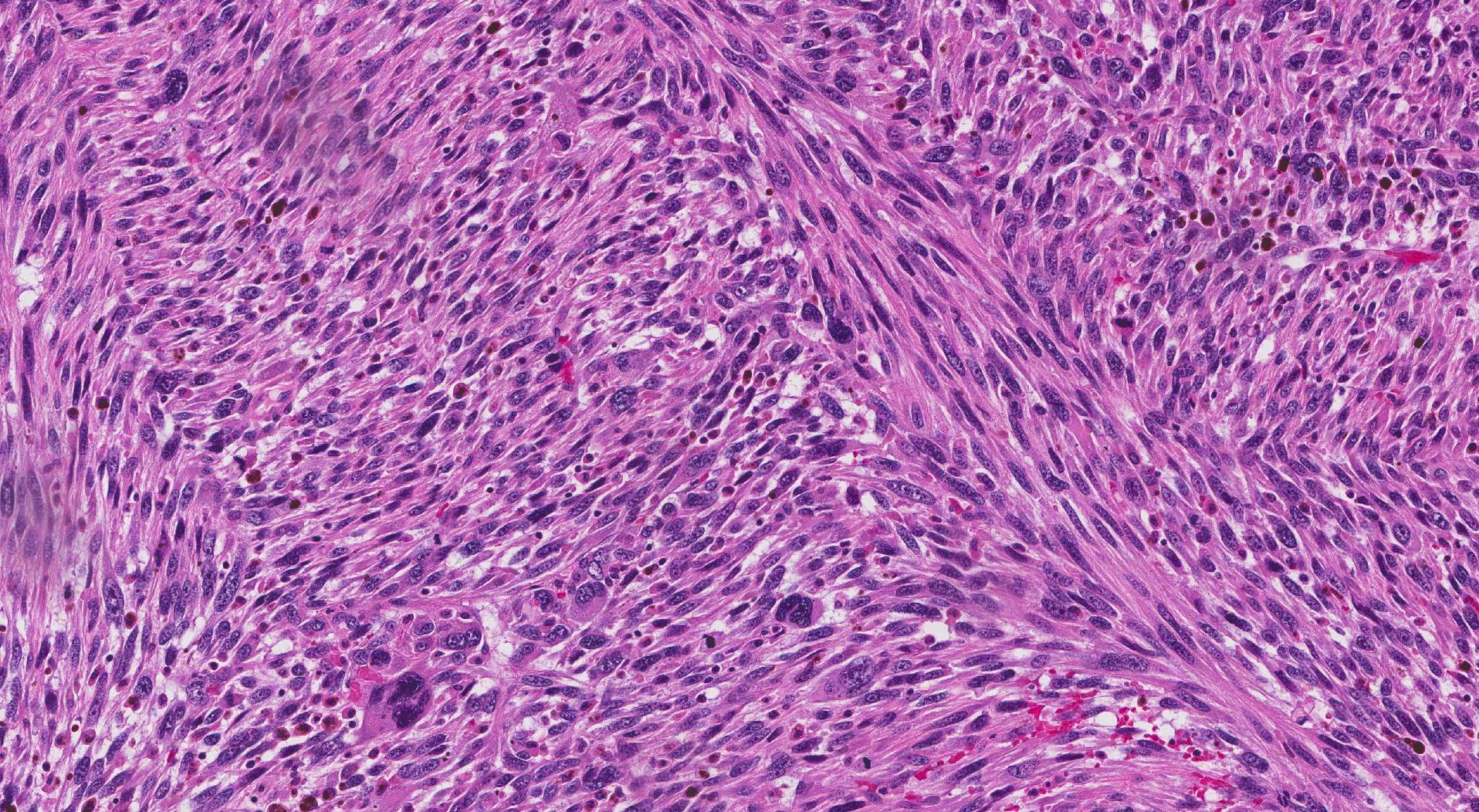
Some uterine leiomyosarcomas are made up of cells that are round. Pathologists call these cells epithelioid because they look similar to specialized epithelial cells found on the surface of many types of tissues. Finally, some uterine leiomyosarcomas are made up of a small number of tumour cells surrounded by loose connective tissue that pathologists describe as myxoid. As with spindle-type leiomyosarcoma, pathologists look for mitotic figures, atypical tumour cells, and necrosis when making the diagnosis of epithelioid or myxoid leiomyosarcoma.

What other tests may be performed to confirm the diagnosis?
Your pathologist may also perform a test called immunohistochemistry to confirm the diagnosis. Immunohistochemistry allows your pathologist to see different types of proteins inside the tumour cells. When this test is performed on a tissue sample from a leiomyosarcoma the tumour cells will be positive proteins normally found in smooth muscle in smooth muscle cells such as h-caldesmon, smooth muscle actin (SMA), and desmin. These immunohistochemical markers are also positive in leiomyoma so these results need to be considered in combination with the histologic features (see above) in order to make the correct diagnosis.
Has the tumour spread into other organs or tissues outside of the uterus?
Several other organs and tissues are directly attached to or are very close to the uterus including the ovaries, fallopian tubes, vagina, bladder, and rectum. Adnexa or adnexal are terms used to describe the fallopian tubes, ovaries, and ligaments connected directly to the uterus. As the tumour becomes bigger, it can grow directly into any of these organs or tissue. When this happens, parts of these other organs or tissues may need to be removed at the same time as the uterus. Your pathologist will carefully examine these other organs or tissues for tumour cells and the results will be described in your pathology report. Finding tumour cells in other organs or tissues is important because it increases the pathologic tumour stage and is associated with a worse prognosis.
What is lymphovascular invasion and why is it important?
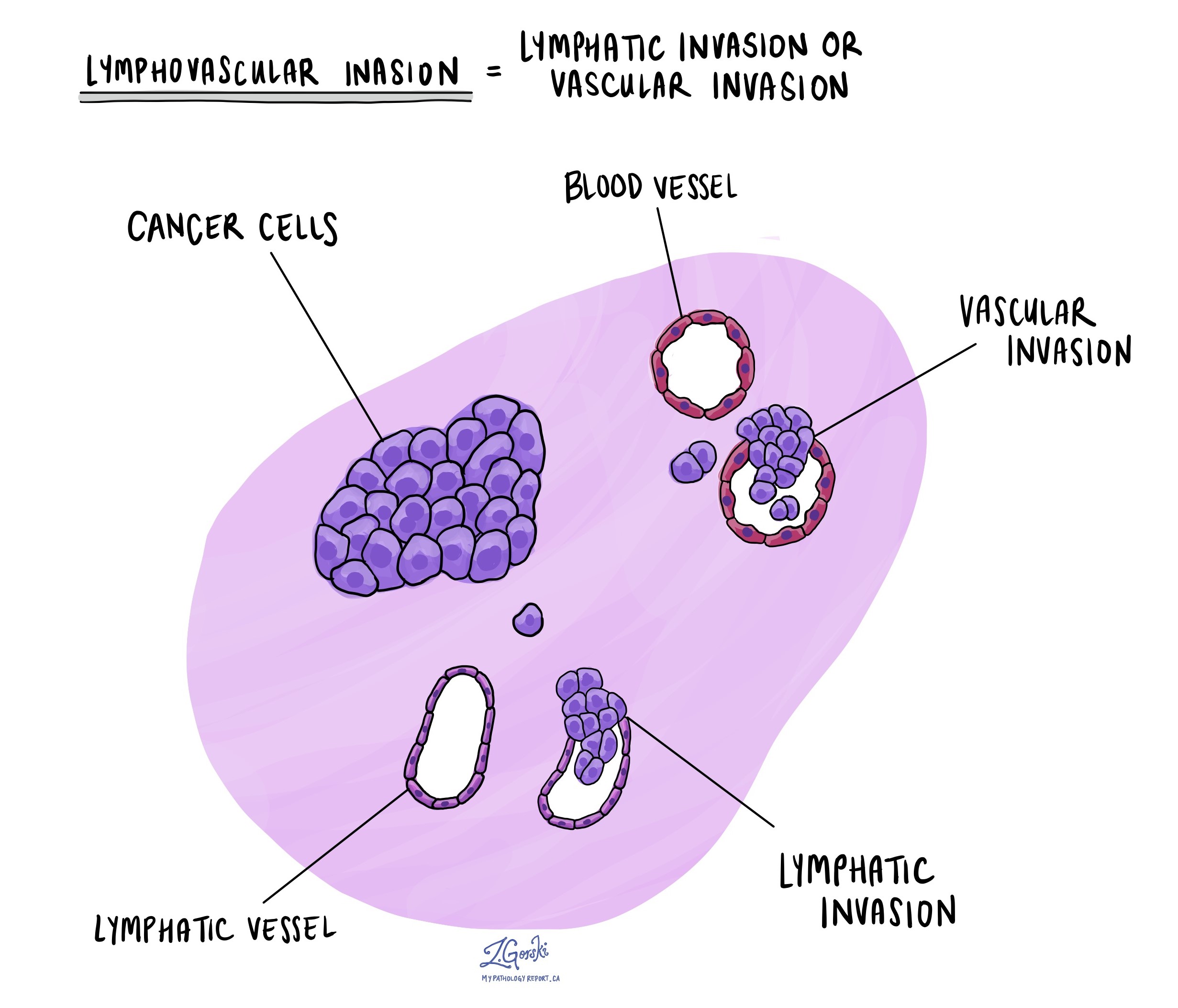
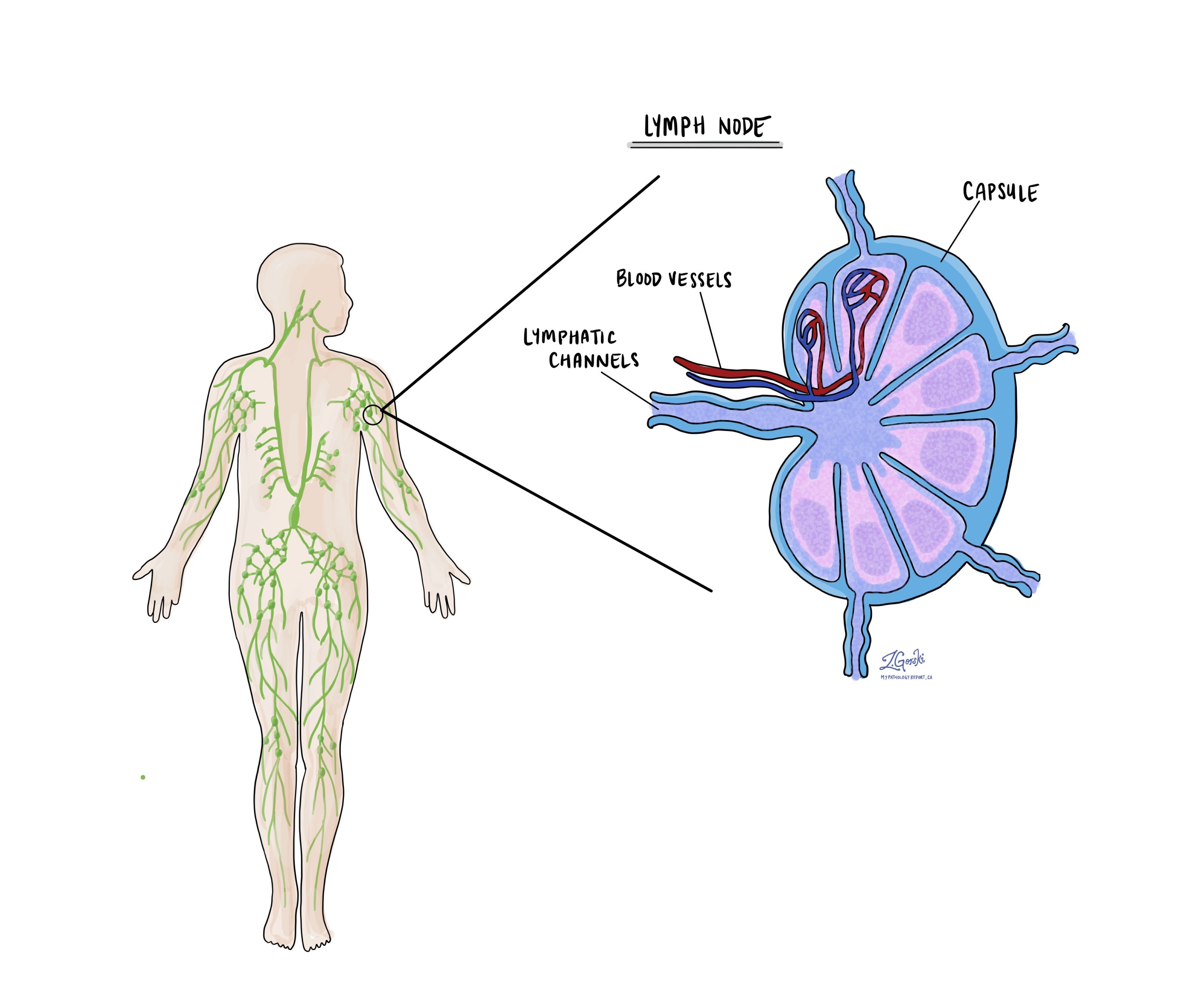
Lymphovascular invasion means that cancer cells were seen inside a blood vessel or lymphatic vessel. Blood vessels are long thin tubes that carry blood around the body. Lymphatic vessels are similar to small blood vessels except that they carry a fluid called lymph instead of blood. The lymphatic vessels connect with small immune organs called lymph nodes that are found throughout the body. Lymphovascular invasion is important because cancer cells can use blood vessels or lymphatic vessels to spread to other parts of the body such as lymph nodes or the lungs.
What is a margin and why are margins important?
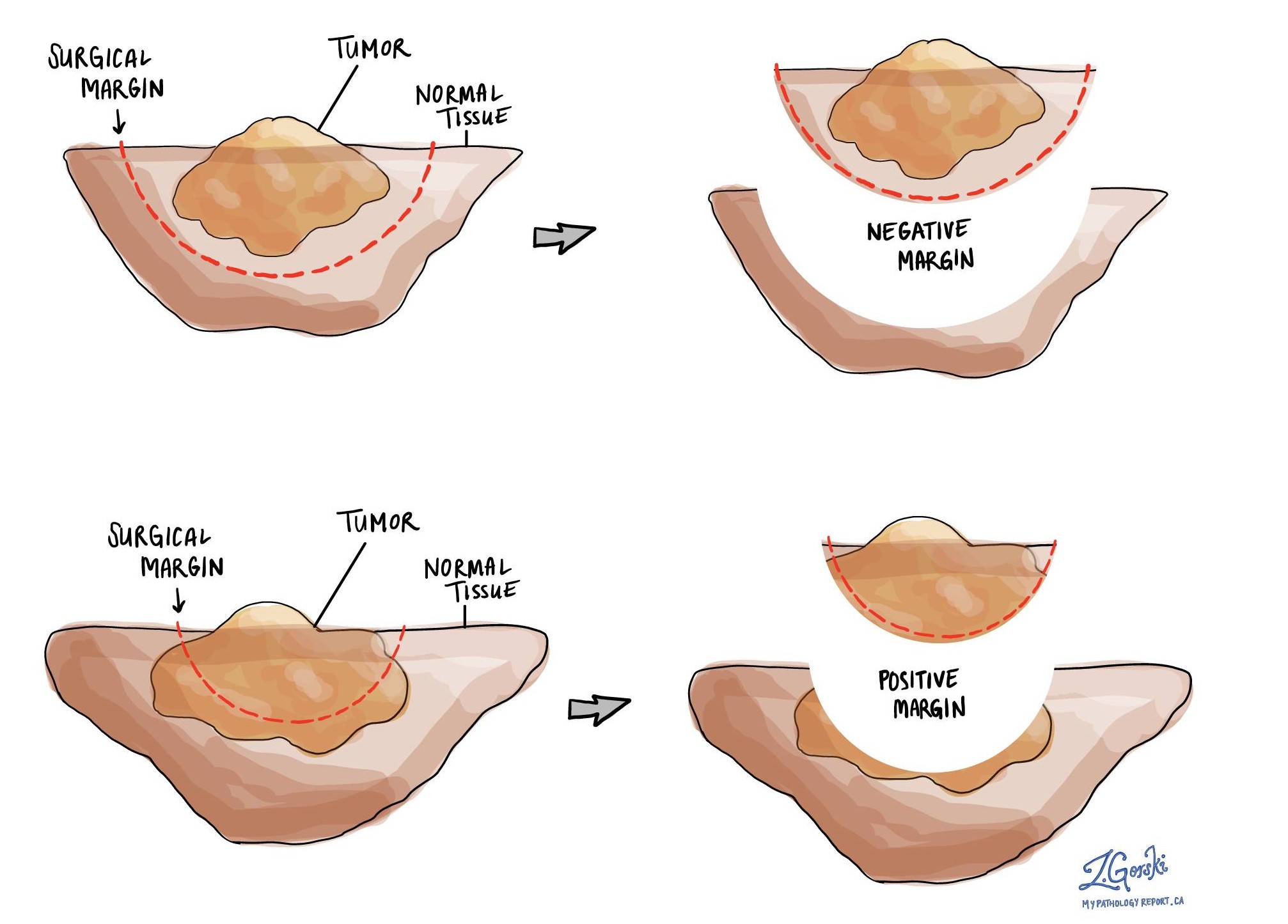
A margin is the normal tissue that surrounds a tumour and is removed with the tumour at the time of surgery. The margins will only be described in cases where the tumour extends into the cervical stroma or other tissues surrounding the uterus and after the entire tumour has been removed.
The type and number of margins described in your report will depend on the type of surgical procedure performed to remove the tumour. A margin is called positive when there are tumour cells at the very edge of the cut tissue. A positive margin is associated with a higher risk that the tumour will recur in the same site after treatment. A negative margin means that no tumour cells were seen at any of the cut edges of tissue.
Were lymph nodes examined and did any contain cancer cells?
Lymph nodes are small immune organs found throughout the body. Cancer cells can spread from a tumour to lymph nodes through small vessels called lymphatics. For this reason, lymph nodes are commonly removed and examined under a microscope to look for cancer cells. The movement of cancer cells from the tumour to another part of the body such as a lymph node is called a metastasis.
Cancer cells typically spread first to lymph nodes close to the tumour although lymph nodes far away from the tumour can also be involved. For this reason, the first lymph nodes removed are usually close to the tumour. Lymph nodes further away from the tumour are only typically removed if they are enlarged and there is a high clinical suspicion that there may be cancer cells in the lymph node.
If any lymph nodes were removed from your body, they will be examined under the microscope by a pathologist and the results of this examination will be described in your report. Most reports will include the total number of lymph nodes examined, where in the body the lymph nodes were found, and the number (if any) that contain cancer cells. If cancer cells were seen in a lymph node, the size of the largest group of cancer cells (often described as “focus” or “deposit”) will also be included.
The examination of lymph nodes is important for two reasons. First, this information is used to determine the pathologic nodal stage (pN). Second, finding cancer cells in a lymph node increases the risk that cancer cells will be found in other parts of the body in the future. As a result, your doctor will use this information when deciding if additional treatment such as chemotherapy, radiation therapy, or immunotherapy is required.
What does it mean if a lymph node is described as positive?
Pathologists often use the term “positive” to describe a lymph node that contains cancer cells. For example, a lymph node that contains cancer cells may be called “positive for malignancy”.
What does it mean if a lymph node is described as negative?
Pathologists often use the term “negative” to describe a lymph node that does not contain any cancer cells. For example, a lymph node that does not contain cancer cells may be called “negative for malignancy”.
What are isolated tumour cells (ITCs)?
Pathologists use the term ‘isolated tumour cells’ to describe a group of tumour cells that measures 0.2 mm or less and is found in a lymph node. If only isolated tumour cells are found in all the lymph nodes examined, the pathologic nodal stage is pN1mi.
What is a micrometastasis?
A ‘micrometastasis’ is a group of tumour cells that measures from 0.2 mm to 2 mm and is found in a lymph node. If only micrometastases are found in all the lymph nodes examined, the pathologic nodal stage is pN1mi.
What is a macrometastasis?
A ‘macrometastasis’ is a group of tumour cells that measures more than 2 mm and is found in a lymph node. Macrometastases are associated with a worse prognosis.
What is the pathologic stage for uterine leiomyosarcoma?
The pathologic stage for uterine leiomyosarcoma is based on the TNM staging system, an internationally recognized system originally created by the American Joint Committee on Cancer. This system uses information about the primary tumour (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathologic stage (pTNM). Your pathologist will examine the tissue submitted and give each part a number. In general, a higher number means a more advanced disease and a worse prognosis.
Tumour stage (pT)
The tumour stage for uterine leiomyosarcoma is based on the size of the tumour and the growth of the tumour outside of the uterus.
- T1a – The tumour only involves the uterus and is 5 cm or less in size.
- T1b – The tumour only involves the uterus and is more than 5 cm in size.
- T2a – The tumour has spread into the adnexal structures surrounding the uterus.
- T2b – The tumour has spread to other organs or tissue in the pelvis.
- T3a – The tumour has spread to at least one site inside the abdomen.
- T3b – The tumour has spread to more than one site in the abdomen.
- T4 – The tumour has grown directly into the bladder or the rectum.
Nodal stage (pN)
The nodal stage for uterine leiomyosarcoma is based on the number of lymph nodes in the pelvis that contain tumour cells.
- N0 – No tumour cells were found in any of the lymph nodes examined.
- N0(i+) – Tumour cells were found in at least one lymph node from the pelvis but the area with tumour cells was not larger than 2 millimetres (only isolated tumour cells or micrometastasis).
- N1 – Tumour cells were found in at least one lymph node from the pelvis and the area with tumour cells was greater than 2 millimetres (macrometastasis).
- NX – No lymph nodes were sent for examination.
Metastatic stage (pM)
The metastatic stage for uterine leiomyosarcoma is based on the presence of tumour cells in a lymph node outside of the pelvis or at a distant site in the body (for example the lungs). The metastatic stage can only be determined if tissue from a distant site is submitted for pathological examination. Because this tissue is rarely present, the metastatic stage cannot be determined and is listed as MX.



