by Katherina Baranova MD and Matt Cecchini MD PhD FRCPC
October 3, 2022
What is usual interstitial pneumonia?
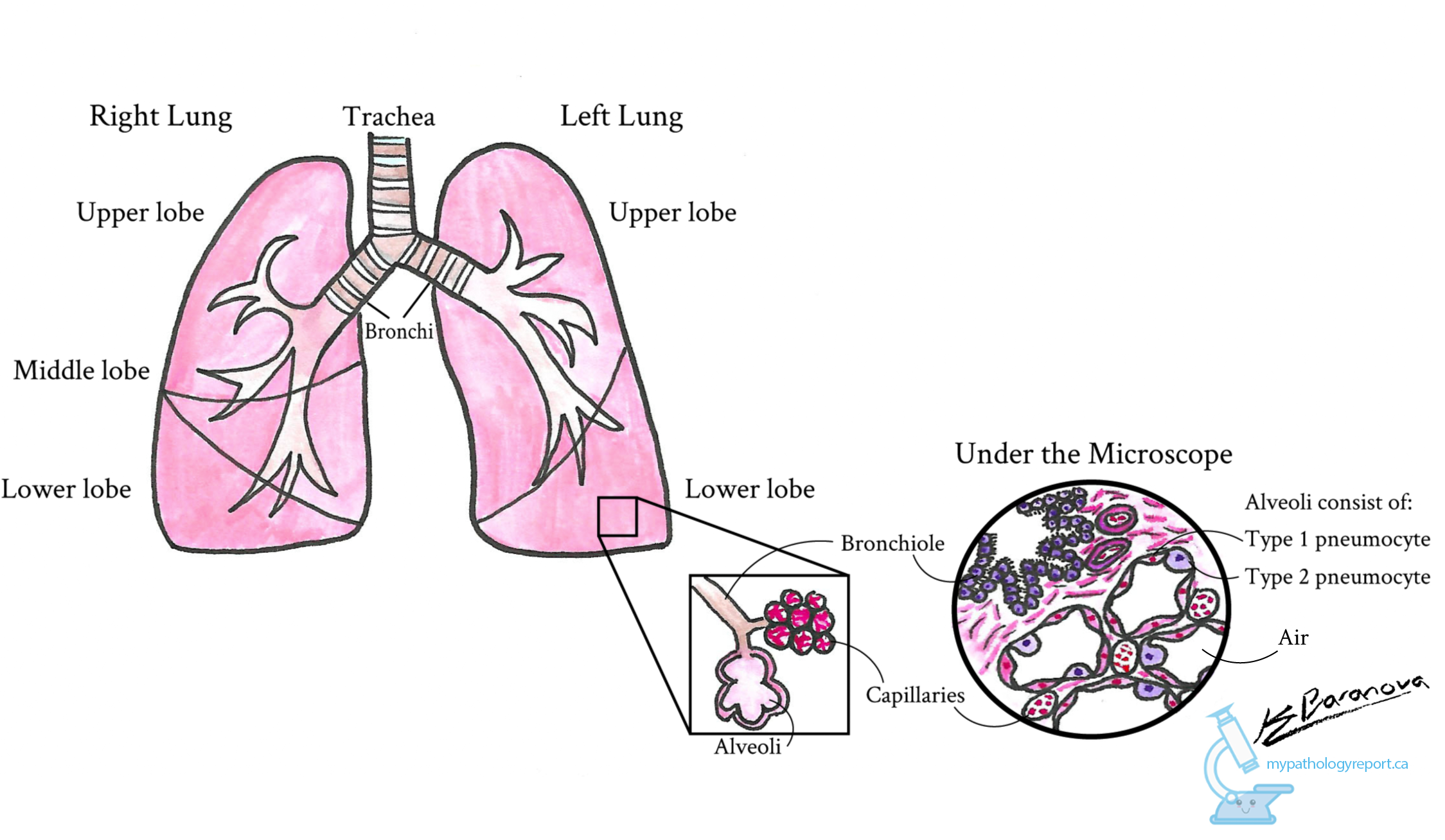
Interstitial pneumonia is a group of diseases where inflammation and fibrosis damage small air-filled spaces inside the lungs called alveoli. Over time, the damage leads to scarring which prevents the lungs from working properly. Although the word pneumonia is used, this does not mean there is an infection in the lung, but rather it is used as a general term that refers to an abnormality in the lung. Usual interstitial pneumonia (UIP) is the most common pattern of disease and the scarring caused by UIP can be seen on imaging such as a CT scan and under the microscope. In fact, the diagnosis of UIP can often be made with imaging alone. The radiology report for UIP often describes severe scarring (fibrosis) that may be worse at the outer (periphery) and lower (bases) parts of the lungs. Radiologists often use the term “honeycomb change” to describe the changes typically seen in UIP. This mirrors what can be seen under the microscope.
What causes usual interstitial pneumonia?
UIP is a pattern of injury that is seen in a number of conditions including connective tissue disorders that can affect the lungs and other parts of the body. The UIP pattern of injury can also be seen in drug toxicity and cases of familial pulmonary fibrosis. In many cases of UIP, there is no specific cause identified and these cases are referred to as idiopathic pulmonary fibrosis (IPF). Before making the diagnosis of IPF, your doctor will consider your symptoms, medical history, and any medications you are taking or have taken in the past. There are new therapies that have some ability to slow down the fibrosis and scarring seen in IPF. Unfortunately, despite these treatments, most patients will have progressive fibrosis and worsening lung function over time.
How do pathologists make this diagnosis?
Some patients with symptoms of interstitial lung disease will undergo a procedure called a biopsy where a piece of tissue is taken from the lung. The tissue sample will then be sent to a pathologist to look for UIP changes under the microscope.
This kind of biopsy is usually performed in the operating room and is called a surgical wedge biopsy. Sometimes, another type of biopsy called a cryobiopsy may be performed. This type of biopsy uses a specialized bronchoscope to freeze a small amount of tissue that can be removed and studied by the pathologist under a microscope. Your pathologist may order special tests which will help determine if the pattern of injury can be explained by another cause. Smaller biopsies from needles such as core needle biopsies and fine needle aspirations do not provide enough material to make the diagnosis of UIP and pathologists recommend against performing these procedures on patients with symptoms of interstitial lung disease. Sometimes, features of another condition called acute lung injury can be seen at the same time as the UIP changes. This is often seen in patients who recently experienced sudden worsening of their symptoms.
What does usual interstitial pneumonia look like under the microscope?
When a tissue sample is examined under the microscope, your pathologist will look for scarring that involves some areas of the lung while other areas appear normal. Pathologists often describe these kinds of changes that involve some, but not all, of the tissue as patchy or focal. The scarring is usually worst near the outer and lower parts of the lung and underneath a thin tissue, a layer called the pleura which lines the outside surface of the lungs.
The damage caused by UIP changes the normal look of the lungs. The normal well-organized alveoli (airspaces) are replaced by large open spaces that connect to form a pattern similar to a honeycomb. Instead of pneumocytes, the large open spaces are often lined by specialized epithelial cells that are normally found in the large airways leading into the lungs. Pathologists describe this change as metaplastic bronchial epithelium.
The damage that UIP causes in the lungs takes place slowly over time. When examined under the microscope your pathologist will see different phases of fibrosis with areas of the lung that were damaged in the past and areas that are only starting to be damaged by the disease. Pathologists describe this as temporal heterogeneity.
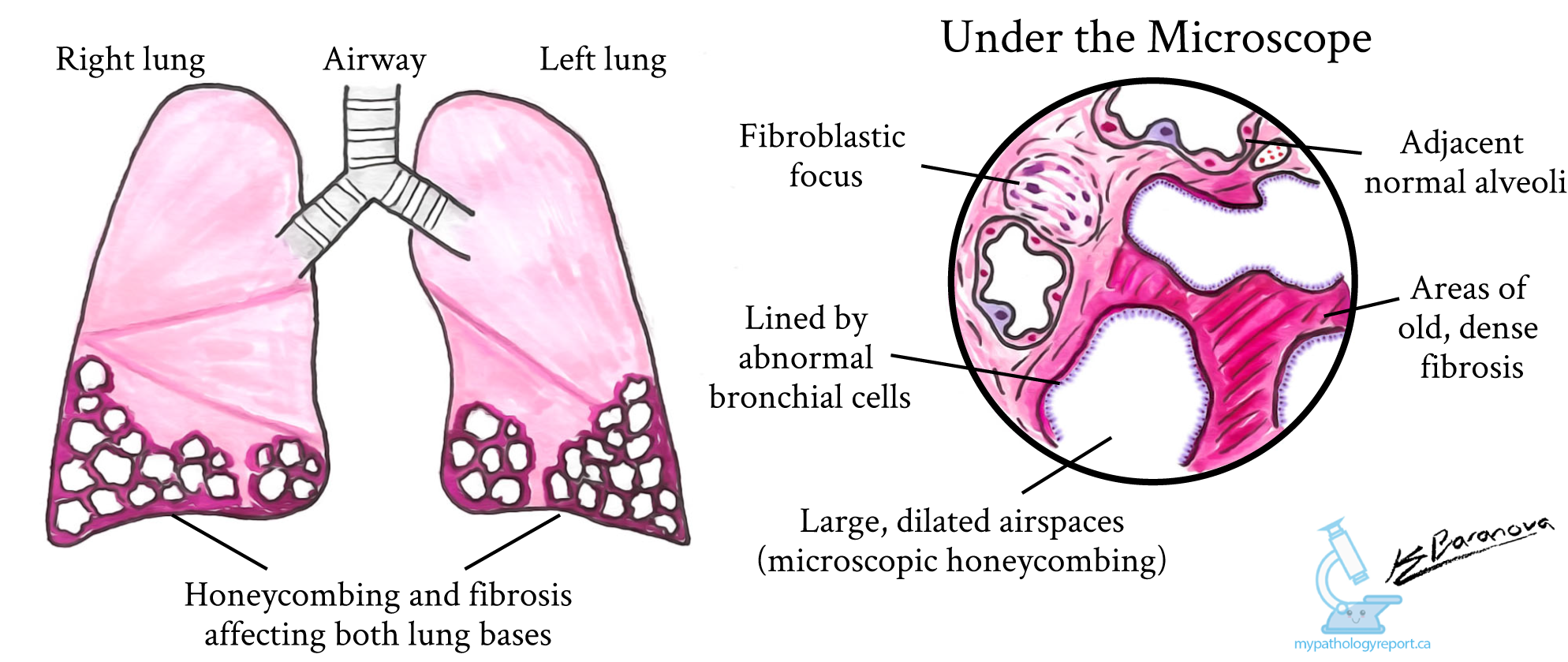
Areas of the lung that were damaged in the past will show dense fibrosis which is how pathologists describe the look of a scar under the microscope. The scar prevents the lung tissue from working properly.
Areas of the lung that are only starting to be damaged by the disease will show small groups of specialized cells called fibroblasts. Pathologists describe this as a loose fibroblast proliferation because the cells are less tightly packed than in a mature scar. The groups of fibroblasts are often found close to areas of the lung that look normal and healthy. These fibroblastic foci (singular: fibroblastic focus) are thought to represent areas of active disease progression.
Pathologists describe the appearance of damaged lung mixed with areas of normal, healthy lung as spatial heterogeneity. Both spatial and temporal heterogeneity are common features of UIP.


