by Ipshita Kak MD FRCPC
March 25, 2023
What is a well differentiated neuroendocrine tumour in the appendix?
Well differentiated neuroendocrine tumour (NET) is a cancer and the most common type of cancer in the appendix. The tumour is made up of specialized neuroendocrine cells that are normally found inside the appendix. Pathologists divide well differentiated NETs of the appendix into three grades although most are associated with a good prognosis.
What are the symptoms of a well differentiated neuroendocrine tumour of the appendix?
Many patients with a well differentiated NET of the appendix present with symptoms of acute appendicitis. This can include abdominal pain, bloating, nausea, and vomiting. Some patients do not have any symptoms and the tumour is discovered incidentally (by accident) when imaging tests such as a CT scan or MRI of the abdomen are performed for other reasons.
What is the difference between a functional and non-functional neuroendocrine tumour?
Well differentiated neuroendocrine tumours (NETs) can be divided into functional and non-functional tumours based on the types of symptoms they produce. Functional tumours produce proteins that can result in specific symptoms. These symptoms or the detection of specific proteins in the blood or urine can help doctors make the correct diagnosis. Non-functional tumours do not produce proteins, and as a result, may go undetected for many years.
Some patients with a functional well differentiated NET present with a very specific set of symptoms that doctors call “carcinoid syndrome”. The presence of this syndrome suggests that the tumour has spread to the liver.
How is the diagnosis of well differentiated neuroendocrine tumour in the appendix made?
The diagnosis of well differentiated NET is usually made after a small piece of the tumour is removed in a procedure called a biopsy. The diagnosis can also be made after the entire tumour is removed in a larger surgical procedure called a resection. The tissue is sent to a pathologist for examination under a microscope.
What does a well differentiated NET look like under the microscope?
When examined under the microscope, the tumour is made up of medium-sized neuroendocrine cells that can show a variety of growth patterns including nested, trabecular, pseudo-glandular, pseudo-acinar, and solid. The cells throughout the tumour tend to be very similar looking which pathologists describe as monomorphic or monotonous. The genetic material or chromatin inside the nucleus of the cell often appears as small dots which pathologists describe as “salt and pepper”.

What other tests are performed to confirm the diagnosis of well differentiated neuroendocrine tumour of the appendix?
A special test called immunohistochemistry may be performed to confirm the diagnosis. This test allows pathologists to better understand cells based on the specific proteins they produce. This test allows pathologists to better understand both the function and origin of the cell.
The cells in a well-differentiated NET commonly produce three proteins: CD56, synaptophysin and chromogranin. By performing immunohistochemistry, your pathologist can ‘see’ these proteins inside the cell. Most cancers produce all three proteins, but some may produce two or even just one of the three. Cells that produce a protein will be called positive or reactive. Those that do not produce the protein are called negative or non-reactive.
What is the WHO grade for well differentiated neuroendocrine tumour of the appendix?
Pathologists divide well differentiated NETs of the appendix into three grades based on a system created by the World Health Organization (WHO). According to this system, higher grade tumours (grades 2 and 3) are more likely than lower grade (grade 1) tumours to spread to other parts of the body. The grade can only be determined after the tumour is examined under the microscope by your pathologist.
Your pathologist will determine the WHO grade based on the number of tumour cells that are in the process of dividing to create new tumour cells. These cells are called mitotic figures and they are undergoing a process called mitosis. The mitotic rate is the number of mitotic figures seen in a given area of tissue (usually 2 mm2).
Your pathologist may also do a test called immunohistochemistry for Ki-67 to highlight cells that are able to divide. The Ki-67 index (or proliferative index) is the percentage of tumour cells that produce Ki-67. The proliferative index for well-differentiated neuroendocrine tumours can range from 1% to over 20%.
The mitotic rate and/or the Ki-67 index is then used to determine the WHO grade as follows:
- Grade 1 (G1) – These tumours have a mitotic rate of less than 2 or a Ki-67 index of less than 3%.
- Grade 2 (G2) – These tumours have a mitotic rate between 2 and 20 or a Ki-67 index of between 3% and 20%.
- Grade 3 (G3) – These tumours have a mitotic rate of greater than 20 or a Ki-67 index of greater than 20%.
What does tumour extension mean and why is it important?
The appendix is a small, hollow, finger-shaped organ that connects with the first part of the colon by a thin opening. The wall of the appendix is made up of six layers of tissue: mucosa, muscularis mucosa, submucosa, muscularis propria, subserosal adipose tissue, and serosa. The mesoappendix is a layer of fatty tissue on the outside of the appendix that surrounds and supports the appendix. The mesoappendix is part of the abdominal peritoneum.
Most well differentiated NETs start from neuroendocrine cells normally found within the mucosa on the inside of the appendix. Pathologists use the term tumour extension to describe how far the tumour cells have spread from the mucosa into the wall of the appendix or surrounding tissues. Tumour cells that cross the serosa on the outer surface of the appendix can spread into nearby organs and tissues such as the colon, small intestine, or abdominal wall.
Tumour extension is important because tumours that have broken through the serosa are able to spread throughout the abdominal cavity and to other parts of the body. Tumour extension is also used to determine the pathologic tumour stage (pT).
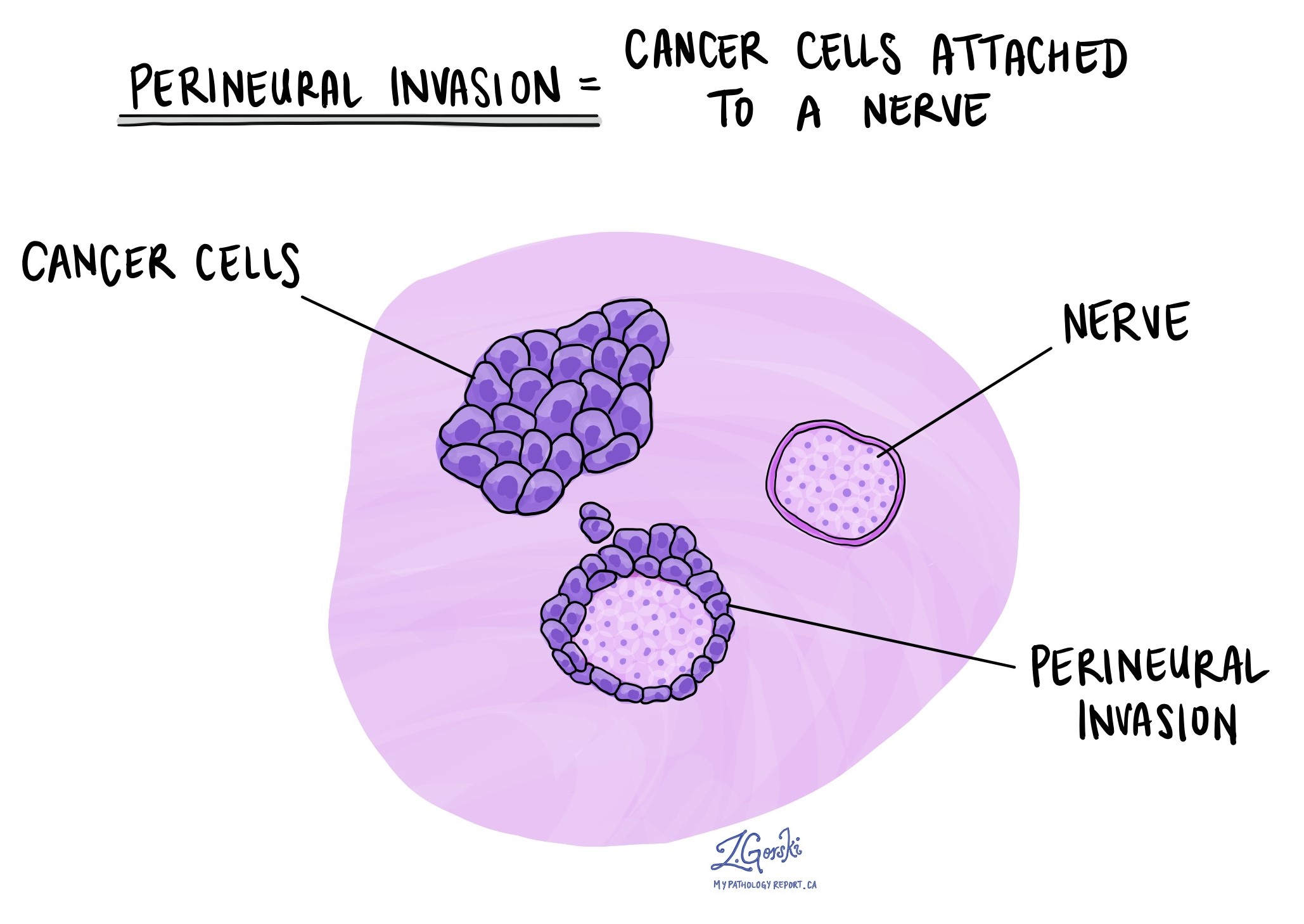
What is perineural invasion and why is it important?
Perineural invasion means that tumour cells were seen attached to a nerve. Nerves are found all over the body and they are responsible for sending information (such as temperature, pressure, and pain) between your body and your brain. Perineural invasion is important because tumour cells that have become attached to a nerve can spread into surrounding tissues by growing along the nerve. This increases the risk that the tumour will regrow after treatment.
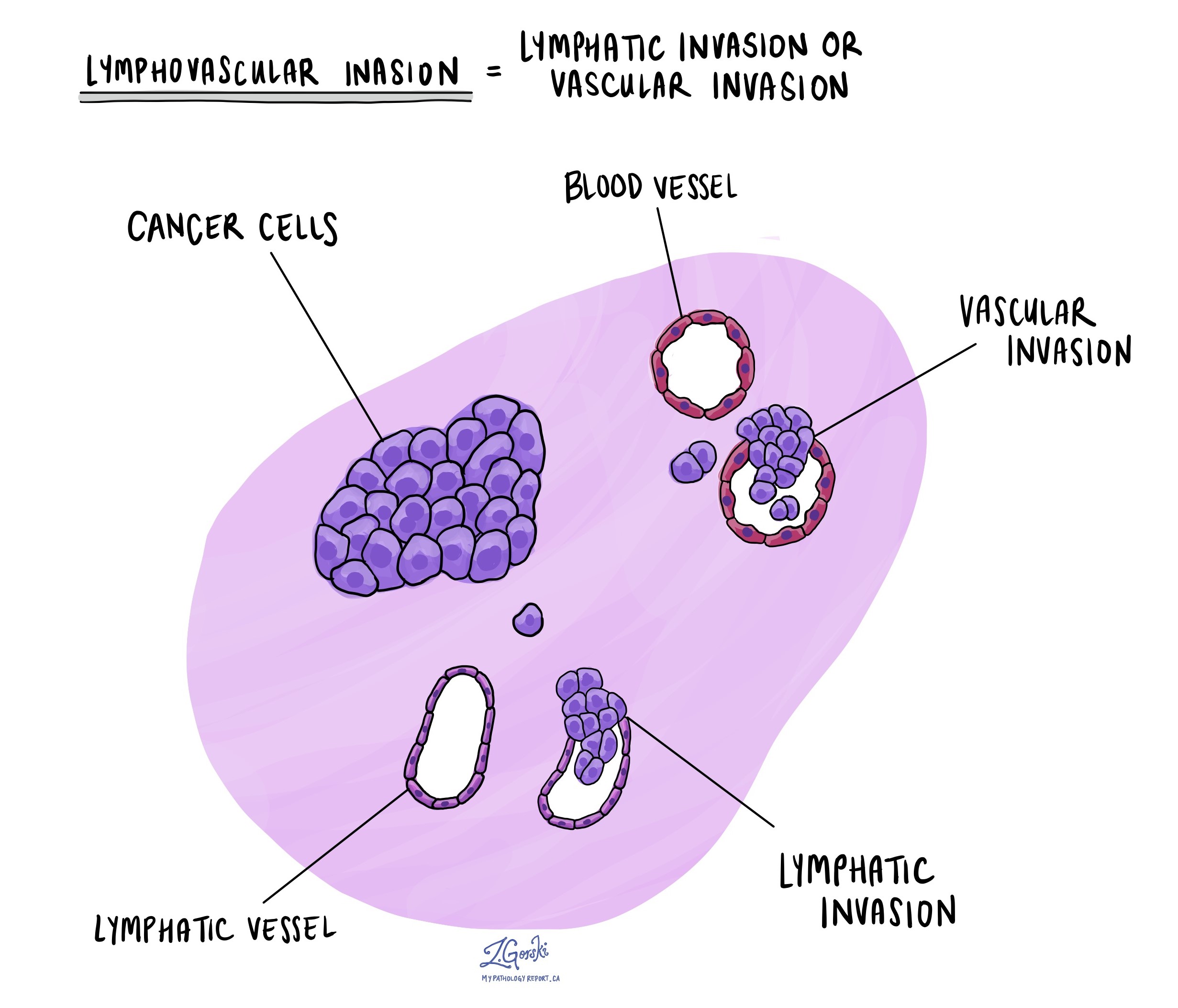
What is lymphovascular invasion and why is it important?
Lymphovascular invasion means that tumour cells were seen inside of a blood vessel or lymphatic vessel. Blood vessels are long thin tubes that carry blood around the body. Lymphatic vessels are similar to small blood vessels except that they carry a fluid called lymph instead of blood. Lymphovascular invasion is important because tumour cells can use blood vessels or lymphatic vessels to spread to other parts of the body such as lymph nodes or the lungs.
What is a margin?
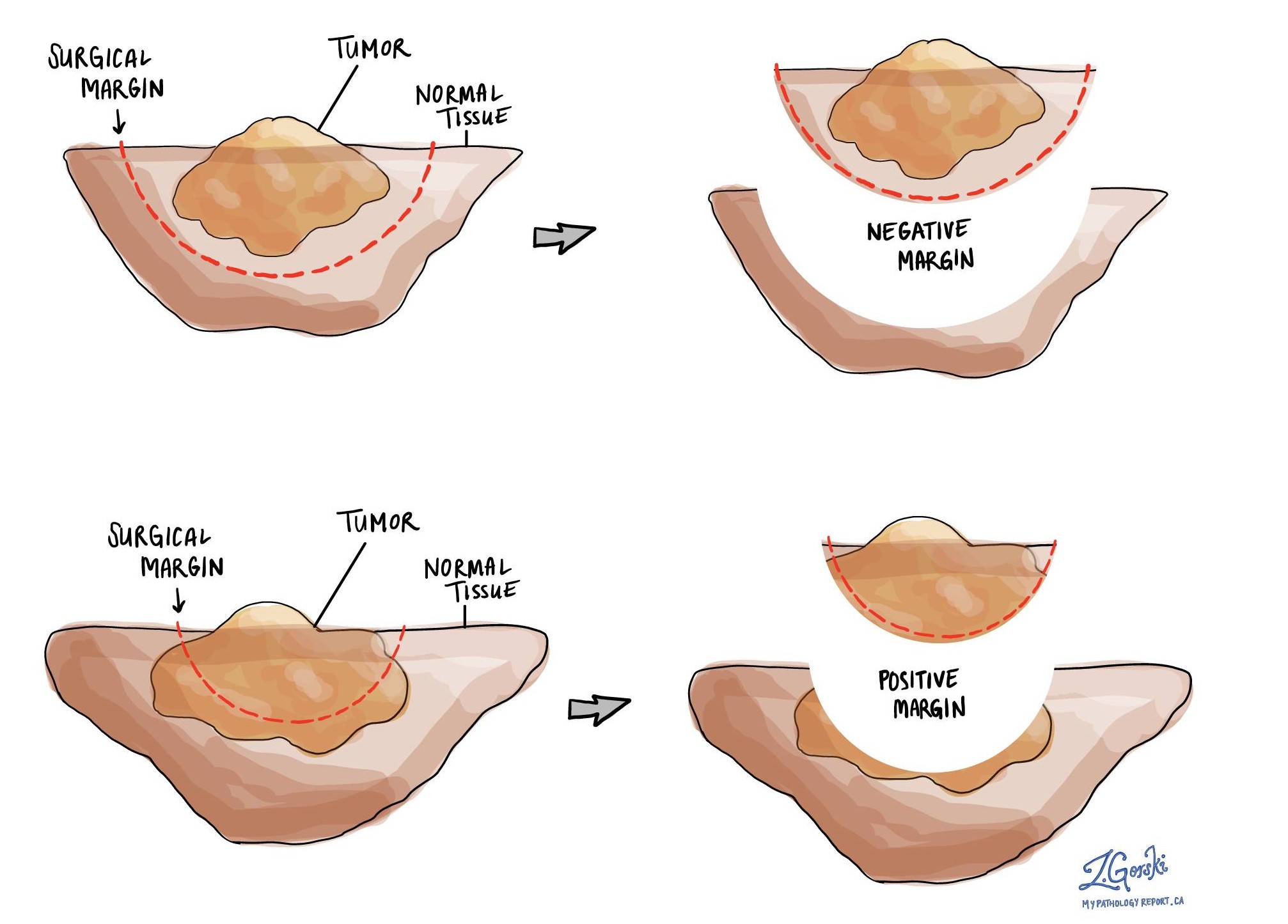
A margin is any tissue that was cut by the surgeon in order to remove the tumour from your body. For most appendiceal tumours, the margin is the area of the appendix that was previously attached to the colon. In some cases, the margin may include a part of the right colon such as the cecum. Margins will only be described in your report after the entire tumour has been removed.
A negative margin means that no tumour cells were seen at any of the cut edges of tissue. A margin is called positive when there are tumour cells at the very edge of the cut tissue. A positive margin is associated with a higher risk that the tumour will recur in the same site after treatment.
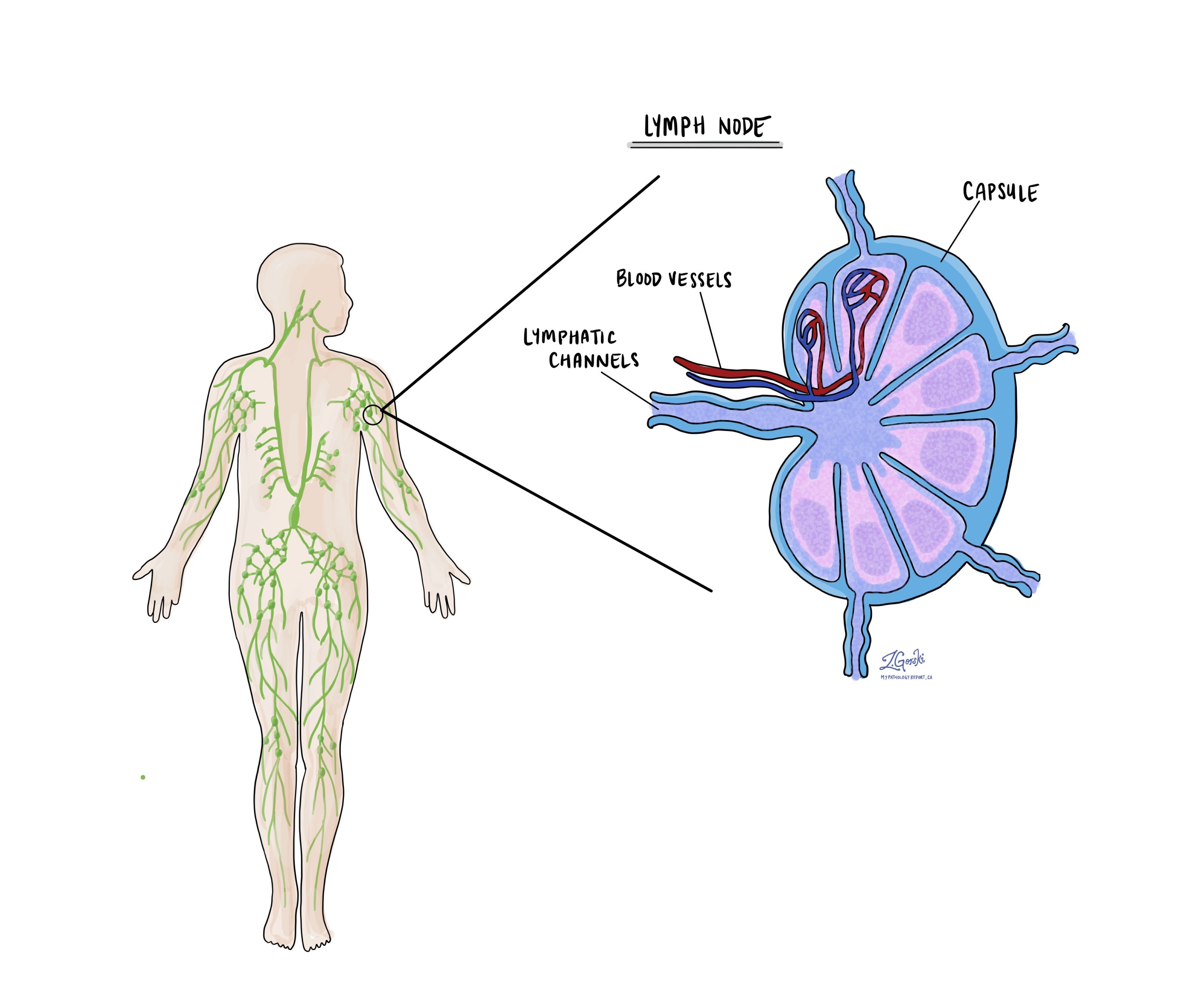
Were lymph nodes examined and did any contain cancer cells?
Lymph nodes are small immune organs located throughout the body. Cancer cells can spread from the tumour to a lymph node through lymphatic channels located in and around the tumour. The movement of cancer cells from the tumour to a lymph node is called metastasis.
Your pathologist will carefully examine each lymph node for cancer cells. Lymph nodes that contain cancer cells are often called positive while those that do not contain any cancer cells are called negative. Most reports include the total number of lymph nodes examined and the number, if any, that contain cancer cells.
The examination of lymph nodes is used to determine the pathologic nodal stage (pN). Finding cancer cells in a lymph node increases the nodal stage and is associated with a worse prognosis.
What information is used to determine the pathologic stage for well differentiated neuroendocrine tumour of the appendix?
The pathologic stage for well differentiated neuroendocrine tumours (NETs) is based on the TNM staging system, an internationally recognized system originally created by the American Joint Committee on Cancer (AJCC). This system uses information about the primary tumour (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathologic stage (pTNM). Your pathologist will examine the tissue submitted and give each part a number. In general, a higher number means more advanced disease and a worse prognosis.
Tumour stage (pT) for well differentiated neuroendocrine tumour
These tumours are given a tumour stage between 1 and 4 based on the size of the tumour and how far the tumour cells have travelled into the wall of the appendix or the surrounding tissues.
- T1 – The tumour is 2 cm or less in size.
- T2 – The tumour is greater than 2 cm in size but less than or equal to 4 cm in size.
- T3 – The tumour is greater than 4 cm in size or it has spread into the subserosa or the mesoappendix.
- T4 – The tumour has spread beyond the serosa of the appendix or it has spread into surrounding organs.
Nodal stage (pN) for well differentiated neuroendocrine tumour
These tumours are given a nodal stage of 0 or 1 based on the presence or absence of cancer cells in a lymph node.
- N0 – No cancer cells are seen in any of the lymph nodes examined.
- N1 – Cancer cells are seen in at least one lymph node.
- NX – No lymph nodes were sent for pathologic examination.
Metastatic stage (pM) for well differentiated neuroendocrine tumour
A well differentiated NET is given a metastatic stage of 0 or 1 based on the presence of tumour cells at a distant site in the body (for example the liver). The metastatic stage can only be assigned if tissue from a distant site is submitted for pathological examination. Because this tissue is rarely present, the metastatic stage cannot be determined and is listed as MX.



