by Jason Wasserman MD PhD FRCPC
August 30, 2025
HPV associated squamous cell carcinoma is a type of cervical cancer that starts in squamous cells. Squamous cells are the flat cells that cover the outside surface of the cervix. The cancer is called HPV associated because it is driven by infection with high-risk types of human papillomavirus. Over time, persistent infection can change the DNA of squamous cells and allow them to grow in an uncontrolled way.
Where on the cervix does it start and why does HPV matter?
Most cases begin in the transformation zone. The transformation zone is the meeting point between the squamous cells on the outside of the cervix and the glandular cells inside the cervical canal. This area is especially vulnerable to infection by high-risk HPV types, most commonly HPV 16 and HPV 18. In most people the immune system clears the virus. When the virus persists, it can cause precancerous changes called high grade squamous intraepithelial lesion. Without treatment, high grade squamous intraepithelial lesion can progress to invasive cancer.

What are the symptoms?
The symptoms of HPV associated squamous cell carcinoma depend on the size of the tumor and how far it has spread. Many people with early-stage disease do not experience any symptoms, and the cancer may only be found through screening.
When symptoms are present, they may include:
-
Unusual vaginal bleeding, such as bleeding after sex, between periods, or after menopause.
-
Increased vaginal discharge, which may be watery, bloody, or have a strong odor.
-
Pain during or after sexual intercourse.
-
Pelvic pain that can become more noticeable as the cancer progresses.
How is the diagnosis made?
The diagnosis of HPV associated squamous cell carcinoma is made by examining tissue from the cervix under the microscope. In most cases, the process begins when abnormal results are found on a Pap test or HPV test.
Tests used to make the diagnosis include:
-
Pap test to look for abnormal squamous cells.
-
HPV test to identify infection with high-risk types of the virus.
-
Colposcopy and biopsy to closely examine the cervix and remove small samples of tissue.
-
Endocervical curettage to scrape cells from inside the cervical canal.
-
Cone biopsy or LEEP to remove a larger piece of tissue, which helps show how deep the cancer has grown and whether the tumor extends to the edge of the removed tissue.
What does HPV associated squamous cell carcinoma look like under the microscope?
Under the microscope, the cancer forms irregular nests, sheets, and cords of squamous cells that grow into the supporting tissue of the cervix. The cells often vary in size and shape, which is called pleomorphism, and many cells are dividing. Early invasion is seen when small, jagged clusters of tumor cells break through the surface layer and grow into the tissue beneath. The nearby tissue often shows a fibrous response called desmoplasia.
Pathologists also describe growth patterns that can help classify the tumor:
-
Non-keratinizing squamous cell carcinoma: This type shows nests or sheets of polygonal squamous cells. Intercellular bridges or small areas of keratin may be present, but keratin pearls are not seen.
-
Keratinizing squamous cell carcinoma: This type shows round whorls of keratin called keratin pearls. The cells look more mature and show prominent intercellular bridges.
-
Basaloid squamous cell carcinoma: This type shows nests of small, immature squamous cells with very little cytoplasm. These cells resemble those seen in high grade squamous intraepithelial lesion.
-
Warty squamous cell carcinoma: This type shows a surface with wart-like projections and cells that resemble koilocytes, which are a common feature of HPV infection.
-
Papillary squamous cell carcinoma: This type grows as finger-like projections called papillae that are lined by abnormal squamous cells. This pattern can be diagnosed even when definite invasion into the deeper tissue is not obvious if there is a visible lesion.
-
Lymphoepithelioma-like squamous cell carcinoma: This is rare type that shows dense inflammation surrounding the tumor. In the cervix this pattern is not linked to Epstein–Barr virus.
Non-keratinizing and basaloid patterns are the most common HPV associated subtypes.
What does “grade” mean?
Grade describes how abnormal the cancer cells look under the microscope compared to normal squamous cells. The grade gives information about how quickly the tumor is likely to grow and spread.
-
Grade 1 (well differentiated) tumors look more like normal squamous cells and usually grow more slowly.
-
Grade 2 (moderately differentiated) tumors look different from normal but can still be recognized as squamous.
-
Grade 3 (poorly differentiated) tumors look very abnormal, may be hard to identify as squamous, and usually grow and spread faster.
What other tests help confirm the diagnosis?
Pathologists often use additional tests to confirm that a tumor is HPV associated squamous cell carcinoma. These tests provide evidence that HPV is driving the cancer and help distinguish it from other tumor types.
The most common tests include:
-
Immunohistochemistry for p16, which shows a strong and continuous staining pattern in HPV-driven cancers.
-
In situ hybridization for high-risk HPV, which detects HPV DNA or RNA directly in the tumor cells.
-
Additional immunohistochemistry, such as p40 or cytokeratins, which can confirm squamous cell origin when the tumor is very abnormal.
How is the tumor measured and why does depth of invasion matter?
Once the diagnosis is made, the tumor is measured in three directions: length, width, and depth of invasion. These measurements are important because they help determine the stage of the cancer and guide treatment decisions.
-
Length describes how far the tumor extends along the surface of the cervix.
-
Width describes how far it spreads from side to side.
-
Depth of invasion describes how far the tumor has grown from the surface into the supporting tissue of the cervix. Depth is especially important because tumors that invade more deeply are more likely to spread to lymph nodes and nearby organs.
Has the tumor spread outside the cervix?
Pathologists describe tumor extension when cancer grows beyond the cervix. Extension can involve the endometrium, the upper or lower vagina, the parametrium, the pelvic wall, the bladder, or the rectum. The parametrium is the fibrous tissue that surrounds the cervix. Extension into these structures raises the stage and is linked to a higher chance of recurrence.
What does lymphovascular invasion mean?
Lymphovascular invasion (LVI) means that cancer cells are present inside small lymphatic channels or blood vessels in the cervix. This finding increases the chance that cancer has reached the lymph nodes or could travel elsewhere. Lymphovascular invasion is more common in higher-grade tumors and often leads to recommendations for closer lymph node evaluation and consideration of additional therapy.
What does perineural invasion mean?
Perineural invasion (PNI) means that cancer cells are growing along or around small nerves in the cervix. This pattern can be associated with a higher chance of local recurrence. When perineural invasion is present, the treatment plan may include radiation to reduce the risk that cancer remains along nerve pathways.
What are margins and why are they important?
Margins are the cut edges of the tissue removed during surgery. A pathologist inks the edges, examines them under the microscope, and reports whether cancer cells touch the ink.
-
A negative margin means that no cancer cells are present at the edge. This suggests that the tumor was completely removed.
-
A positive margin means that cancer cells reach the edge. This increases the risk that some cancer remains. Doctors may recommend a second surgery or radiation to clear the margin.
Margins are assessed in cone biopsies and in hysterectomy specimens. For small early tumors, a clear margin on a cone biopsy can allow patients to avoid larger surgery. If the margin is involved, further treatment is advised.

Lymph nodes
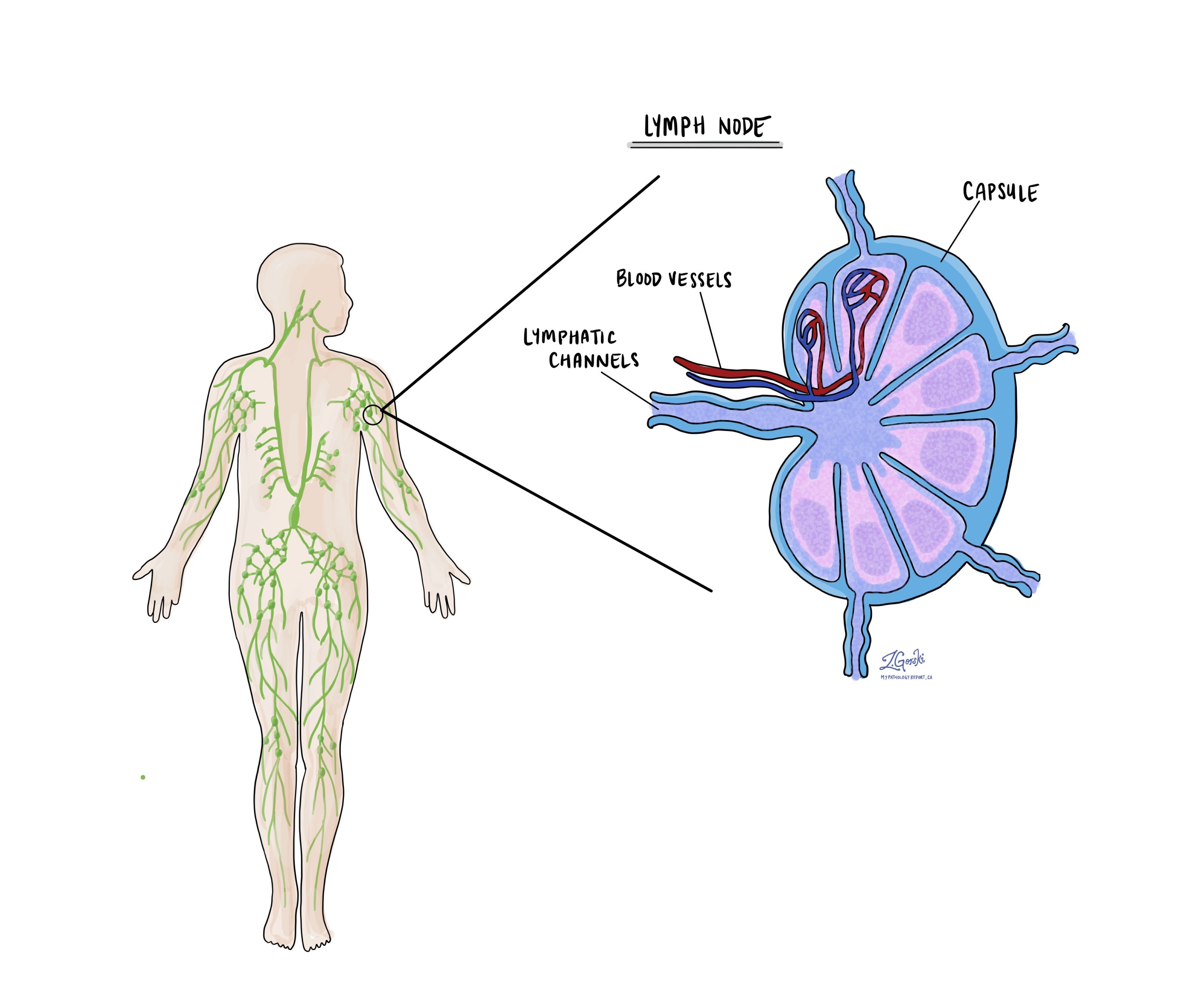
Lymph nodes are small immune system organs that are found throughout the body. They act as filters that help trap and destroy harmful substances such as bacteria, viruses, and cancer cells. Groups of lymph nodes are located in many areas, including the neck, armpits, chest, abdomen, and pelvis.
The cervix drains into lymph nodes in the pelvis and abdomen. If cancer cells enter the lymphatic channels, which are tiny vessels that carry fluid and immune cells, they can travel to nearby lymph nodes. Because of this, lymph nodes are one of the first places that cervical cancer can spread. Examining the lymph nodes helps doctors determine how advanced the cancer is and whether additional treatment such as radiation or chemotherapy is needed.
How are lymph nodes examined?
During surgery for cervical cancer, lymph nodes from the pelvis and sometimes from the para-aortic area (which is higher up in the abdomen near the large blood vessel called the aorta) are removed and sent to the pathology laboratory. A pathologist carefully examines each lymph node under the microscope.
The pathology report usually includes:
-
The total number of lymph nodes removed and examined.
-
The location of the lymph nodes (pelvic, para-aortic, or other specific sites).
-
Whether cancer cells were found in any of the lymph nodes.
-
The size of any deposits of cancer within the nodes.
How are the results reported?
If cancer is found in a lymph node, the pathologist will measure the amount of tumor present and classify it into one of three categories:
-
Isolated tumor cells: Tiny clusters of cancer cells smaller than 0.2 millimeters.
-
Micrometastasis: Clusters of cancer cells between 0.2 and 2 millimeters in size.
-
Macrometastasis: Deposits of cancer larger than 2 millimeters.
The pathology report may use the terms “positive” lymph node to mean that cancer was found in the node, or “negative” lymph node to mean that no cancer cells were seen.
Why are these results important?
The status of the lymph nodes is one of the most important pieces of information for staging cervical cancer.
-
If no cancer is found in any lymph nodes, the risk of spread is lower and surgery alone may be enough for treatment.
-
If cancer is present in one or more lymph nodes, the stage of the cancer increases, and additional treatment such as radiation therapy or chemotherapy is usually recommended.
-
The number of positive lymph nodes and the size of the deposits also help doctors predict the risk of recurrence and choose the best treatment plan.
How is HPV associated cervical cancer staged?
Staging describes how far the cancer has spread within the cervix and beyond. It is the most important factor for predicting outcome and deciding on treatment. Two systems are commonly used for cervical cancer: TNM and FIGO.
-
The TNM system records tumor size and spread in the cervix (T), whether lymph nodes contain cancer (N), and whether the cancer has spread to distant organs (M).
-
The FIGO system focuses on how far the cancer has spread beyond the cervix into surrounding tissues, lymph nodes, or distant sites. It is widely used by gynecologic oncologists to guide treatment planning.
TNM pathologic stage
-
The letter T describes how far the tumor has grown in and around the cervix.
-
T1a means that the tumor is only visible under the microscope and measures no more than five millimeters in depth and no more than seven millimeters in width.
-
T1b means that the tumor is visible or measures deeper than five millimeters or wider than seven millimeters.
-
T2a means that the tumor has spread beyond the cervix and uterus but has not entered the parametrium.
-
T2b means that the tumor has grown into the parametrium.
-
T3a means that the tumor involves the lower part of the vagina.
-
T3b means that the tumor reaches the pelvic wall or blocks a ureter, which can harm the kidneys.
-
T4 means that the tumor has grown into the bladder or rectum or has extended beyond the pelvis.
-
-
The letter N describes lymph nodes.
-
NX means that no nodes were removed.
-
N0 means that no cancer was found in the nodes.
-
N0 with isolated tumor cells means that only tiny clusters smaller than zero point two millimeters were present.
-
N1 means that a larger deposit of cancer was found in at least one node.
-
-
The letter M describes distant spread to organs such as the lungs or liver.
FIGO stage
-
Stage I means that the cancer is confined to the cervix.
-
Stage IA1 means that the depth of invasion is three millimeters or less.
-
Stage IA2 means that the depth of invasion is between three and five millimeters.
-
Stage IB1 means that the tumor is two centimetres or smaller.
-
Stage IB2 means that the tumor is more than two centimetres and up to four centimetres.
-
Stage IB3 means that the tumor is larger than four centimetres.
-
-
Stage II means that the cancer has spread beyond the cervix but not to the pelvic wall or the lower third of the vagina.
-
Stage IIA1 means that the tumor involves the upper vagina and measures four centimetres or less.
-
Stage IIA2 means that the tumor in the upper vagina is larger than four centimetres.
-
Stage IIB means that the tumor extends into the parametrium.
-
-
Stage III means more extensive local spread.
-
Stage IIIA means that the cancer involves the lower third of the vagina.
-
Stage IIIB means that the cancer reaches the pelvic wall or blocks a ureter.
-
Stage IIIC1 means that cancer is present in pelvic lymph nodes.
-
Stage IIIC2 means that cancer is present in para-aortic lymph nodes.
-
-
Stage IV means spread to nearby organs or to distant sites.
-
Stage IVA means invasion of the bladder or rectum.
-
Stage IVB means distant metastasis to organs such as the lungs, liver, or bones.
-
Staging guides treatment and helps predict outcome.
What is the prognosis?
Outcome for patients diagnosed with HPV associated squamous cell carcinoma of the cervix depends on stage and on several pathologic features.
-
Stage is the strongest predictor. When the cancer is confined to the cervix, five-year survival is usually higher than ninety percent. Spread to nearby tissues or lymph nodes lowers survival to a range of roughly fifty to eighty percent depending on how far the cancer has grown. Distant spread has a much lower survival that is often less than twenty percent.
-
Tumor size and depth of invasion matter. Larger and deeper tumors have a higher chance of spread to lymph nodes and a higher risk of recurrence.
-
Margins, lymphovascular invasion, perineural invasion, and lymph node status all influence the need for additional treatment and follow-up intensity.
-
HPV associated tumors often respond well to treatment. Early stage disease is frequently cured with surgery alone. More advanced disease is treated with radiation and chemotherapy, and many patients are still cured.
Regular follow-up visits are important because most recurrences happen within the first few years after treatment. HPV vaccination and routine screening with Pap and HPV tests reduce the risk of developing cervical cancer in the future.
Questions to ask your doctor
- What is my exact stage using both the TNM system and the FIGO system?
-
How large is the tumor and how deep is the invasion into the cervical stroma?
-
Were lymphovascular invasion or perineural invasion present in my specimen?
-
Were the surgical margins negative, and do I need additional surgery to clear the margins?
-
How many lymph nodes were examined and did any contain cancer?
-
What treatment plan do you recommend and why is it the best option for me?
-
Is a fertility-sparing option possible in my situation?
-
What side effects should I expect from surgery, radiation, or chemotherapy?
-
How often will I need follow-up visits and which tests will be used to monitor for recurrence?


