By Jason Wasserman MD PhD FRCPC
June 8, 2023
What is a sinonasal inflammatory polyp?
A sinonasal inflammatory polyp is a non-cancerous growth that may develop in the nasal cavity or paranasal sinuses. It is a very common condition that affects up to 20% of the adult population in some parts of the world.
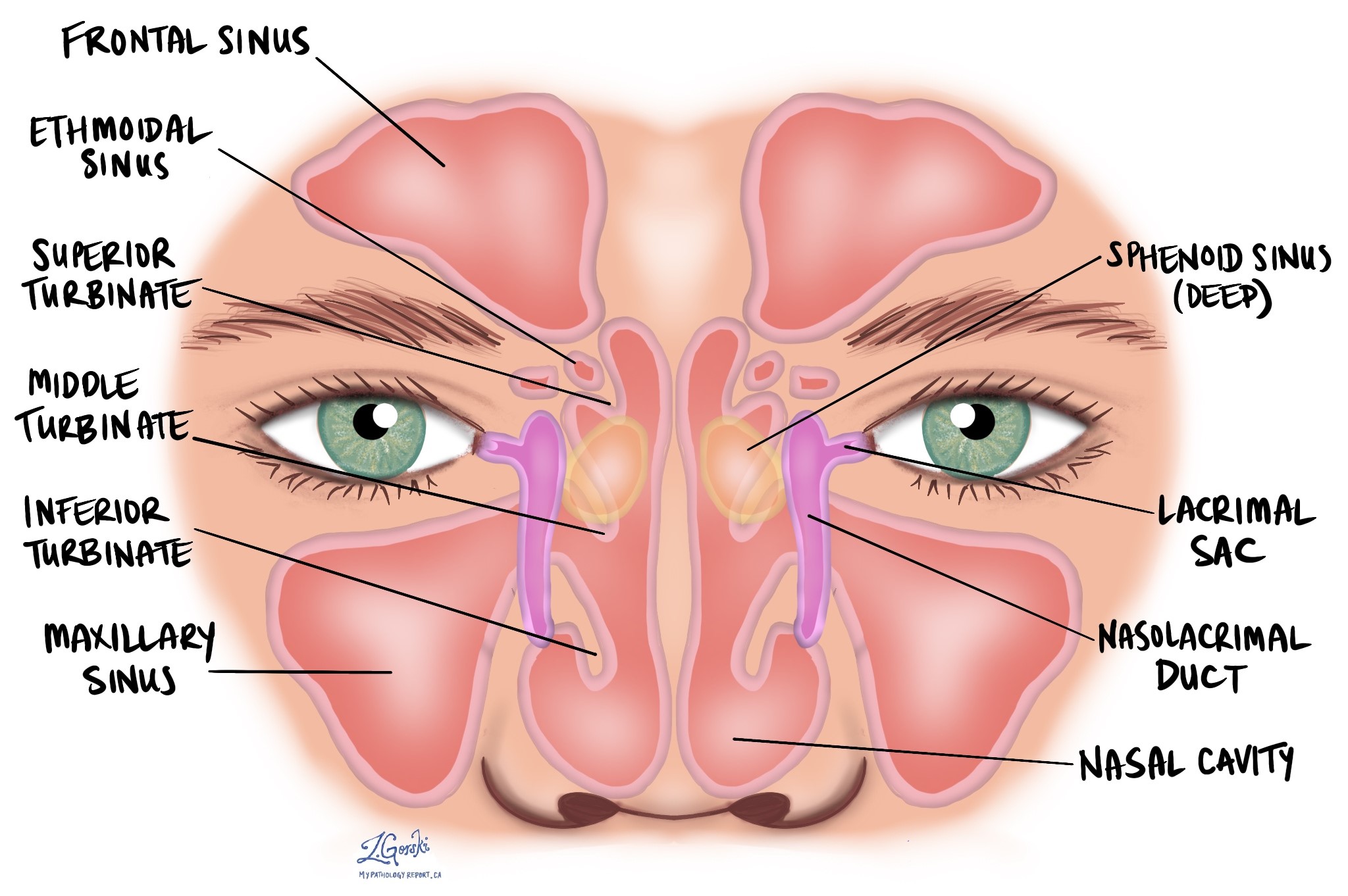
What causes a sinonasal inflammatory polyp?
Sinonasal inflammatory polyps can be caused by anything that leads to chronic inflammation in the nasal cavity and paranasal sinuses including allergies, upper respiratory tract infections, cystic fibrosis, aspirin intolerance, and diabetes.
How do pathologists make this diagnosis?
The diagnosis of sinonasal inflammatory polyp is usually made after part or all of the polyp is removed in a procedure called an excision. When only small pieces of tissue are removed the procedure may be called a biopsy. In order to make this diagnosis, a pathologist needs to examine the tissue sample under the microscope.
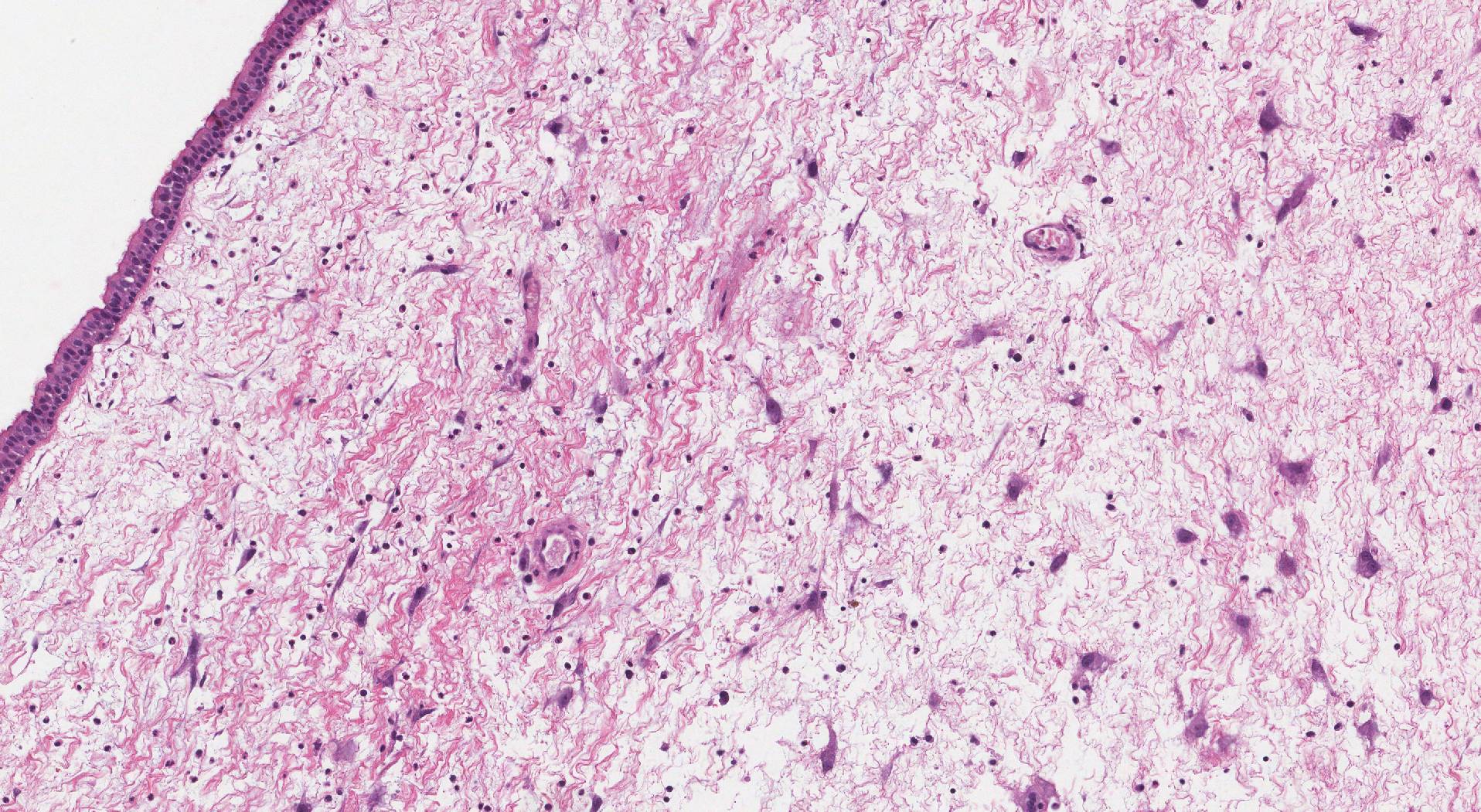
What does a sinonasal inflammatory polyp look like under the microscope?
When examined under the microscope, the polyp is usually made up of one or more round pieces of tissue. Pathologists call these polyps because they stick out from the surface of the tissue. The cells on the outside of the polyp are the same type found in the normal sinonasal epithelium. Large numbers of specialized inflammatory cells including neutrophils, eosinophils, plasma cells, and lymphocytes are typically seen within the stroma. The stroma also tends to look white under the microscope because it is full of fluid. This type of change is called edema. The number of glands in the stroma is also typically decreased.