by Jason Wasserman MD PhD FRCPC
July 29, 2024
Background:
Minimally invasive encapsulated follicular variant papillary thyroid carcinoma (FVPTC) is a type of thyroid gland cancer and a subtype of papillary thyroid carcinoma (PTC). As its name suggests, it has features of both follicular and papillary thyroid carcinoma. In particular, it displays the follicular growth pattern of follicular carcinoma, while the cells have the nuclear features characteristic of papillary carcinoma.
What are the symptoms of minimally invasive encapsulated follicular variant papillary thyroid carcinoma?
The symptoms of minimally invasive encapsulated follicular variant papillary thyroid carcinoma can be similar to other thyroid cancers and may include:
- A palpable nodule or lump in the neck.
- Swelling in the neck.
- Hoarseness or changes in voice.
- Difficulty swallowing.
- Difficulty breathing.
- Persistent cough not related to a cold.
What causes minimally invasive encapsulated follicular variant papillary thyroid carcinoma?
The exact cause of minimally invasive encapsulated follicular variant papillary thyroid carcinoma is not well understood, but several risk factors and genetic mutations have been identified:
- Radiation exposure: Previous exposure to radiation, especially during childhood, increases the risk of developing follicular variant papillary thyroid carcinoma.
- Genetic mutations: Follicular variant papillary thyroid carcinoma is often associated with mutations in the RAS family of genes. Only a minority of cases show BRAF alterations, which are more commonly seen in the classic subtype of papillary thyroid carcinoma.
How is the diagnosis of minimally invasive encapsulated follicular variant papillary thyroid carcinoma made?
The diagnosis of minimally invasive encapsulated follicular variant papillary thyroid carcinoma involves several steps:
- Physical examination: Evaluation of the neck for lumps or nodules.
- Ultrasound: Imaging to assess the thyroid and surrounding structures, providing details about the nodule’s size, composition, and vascularity.
- Fine-needle aspiration (FNA) biopsy: A sample of cells is taken from the nodule and examined under a microscope. However, FNA cannot definitively distinguish between benign and malignant follicular tumours.
- Thyroid function tests: Blood tests to measure levels of thyroid hormones and thyroid-stimulating hormone (TSH).
- Surgical to remove the nodule: Surgery is often required to make the final diagnosis of follicular variant papillary thyroid carcinoma. This often involves removing the half of the thyroid gland. The nodule is then sent to a pathologist for histopathological examination. This is necessary to assess for capsular and vascular invasion.
Capsular invasion
Follicular variant papillary thyroid carcinoma is described as “encapsulated” when the tumour is almost entirely surrounded by a thin layer of tissue called a tumour capsule. The term “minimally invasive” means that upon microscopic examination, small groups of tumour cells were seen breaking through the capsule and spreading into the surrounding thyroid gland.
These terms are important because they help distinguish this type of cancer from two related tumours: noninvasive follicular thyroid neoplasm with papillary-like nuclear features (NIFTP) and infiltrative follicular variant papillary thyroid carcinoma. Unlike NIFTP, minimally invasive encapsulated follicular variant papillary thyroid carcinoma is a malignant (cancerous) tumour that can spread beyond the thyroid gland. However, patients with minimally invasive encapsulated tumours tend to have a good overall prognosis. In contrast, infiltrative follicular variant papillary thyroid carcinoma is a more aggressive type of cancer that frequently spreads to other parts of the body.
Tumour size
After the tumour is removed completely, it will be measured. The tumour is usually measured in three dimensions, but only the largest dimension is described in your report. For example, if the tumour measures 4.0 cm by 2.0 cm by 1.5 cm, your report will describe the tumour as being 4.0 cm. The size of the tumour is important for minimally invasive encapsulated follicular variant papillary thyroid carcinoma because it is used to determine the pathologic stage (pT) and because tumours greater than 4 cm are more likely to metastasize (spread) to other parts of the body.
Extrathyroidal extension
Extrathyroidal extension (ETE) refers to the spread of cancer cells beyond the thyroid gland into surrounding tissues. It is an important prognostic factor in thyroid cancer, as it can significantly influence both the staging and management of the disease.
Extrathyroidal extension is classified into two types based on the extent of the spread:
- Microscopic extrathyroidal extension: This form of extension is only visible under a microscope and indicates that the cancer has spread just beyond the thyroid capsule but cannot be seen with the naked eye. It may involve minimal infiltration into surrounding soft tissues.
- Macroscopic (or gross) extrathyroidal extension: This type is visible to the naked eye or detectable during surgery. It involves more obvious and extensive invasion into neighbouring structures such as muscles, trachea, esophagus, or major blood vessels.
Extrathyroidal extension is important for the following reasons:
- Prognosis: Macroscopic (gross) extrathyroidal extension is associated with a worse prognosis. It suggests a more aggressive cancer that is more likely to recur and metastasize.
- Staging: Extrathyroidal extension impacts the staging of thyroid cancer. For instance, in the TNM (Tumor, Node, Metastasis) classification system used for thyroid cancer, macroscopic extrathyroidal extension results in a higher pathologic tumour stage (pT).
- Treatment and follow-up: The presence of macroscopic (gross) extrathyroidal extension might lead to more aggressive treatment strategies and closer follow-up to reduce the risk of recurrence.
Vascular invasion (angioinvasion)
Vascular invasion, or angioinvasion, is a term used to describe the spread of cancer cells into a blood vessel. Vascular invasion is important because the cancer cells can use blood vessels to metastasize (spread) to other body parts, such as the lungs or bones. To make the diagnosis of minimally invasive encapsulated follicular variant papillary thyroid carcinoma, your pathologist should not see any evidence of vascular invasion. If vascular invasion is seen, the tumour should be diagnosed as encapsulated angioinvasion follicular variant papillary thyroid carcinoma.
Lymphatic invasion
Lymphatic invasion in the context of minimally invasive encapsulated follicular variant papillary thyroid carcinoma of the thyroid gland refers to the infiltration and spread of cancer cells into the lymphatic system. Cancer cells that enter the lymphatic system can travel to lymph nodes. It is relatively uncommon to find lymphatic invasion with minimally invasive encapsulated follicular variant papillary thyroid carcinoma, and unlike vascular invasion, the presence of lymphatic invasion is not necessarily associated with a more aggressive disease or a worse prognosis.
Margins
In pathology, a margin is the edge of tissue removed during tumour surgery. The margin status in a pathology report is important as it indicates whether the entire tumour was removed or if some was left behind. This information helps determine the need for further treatment.
Pathologists examine margins to check if tumour cells are present at the tissue’s cut edge. A positive margin, where tumour cells are found, suggests that some tumour cells may remain in the body. In contrast, a negative margin, with no tumour cells at the edge, suggests the tumour was fully removed. Some reports also measure the distance between the nearest tumour cells and the margin, even if all margins are negative.

Lymph nodes
Lymph nodes are small immune organs found throughout the body. Cancer cells can spread from a tumour to lymph nodes through small lymphatic vessels. For this reason, lymph nodes are commonly removed and examined under a microscope to look for cancer cells. The movement of cancer cells from the tumour to another part of the body, such as a lymph node, is called metastasis.
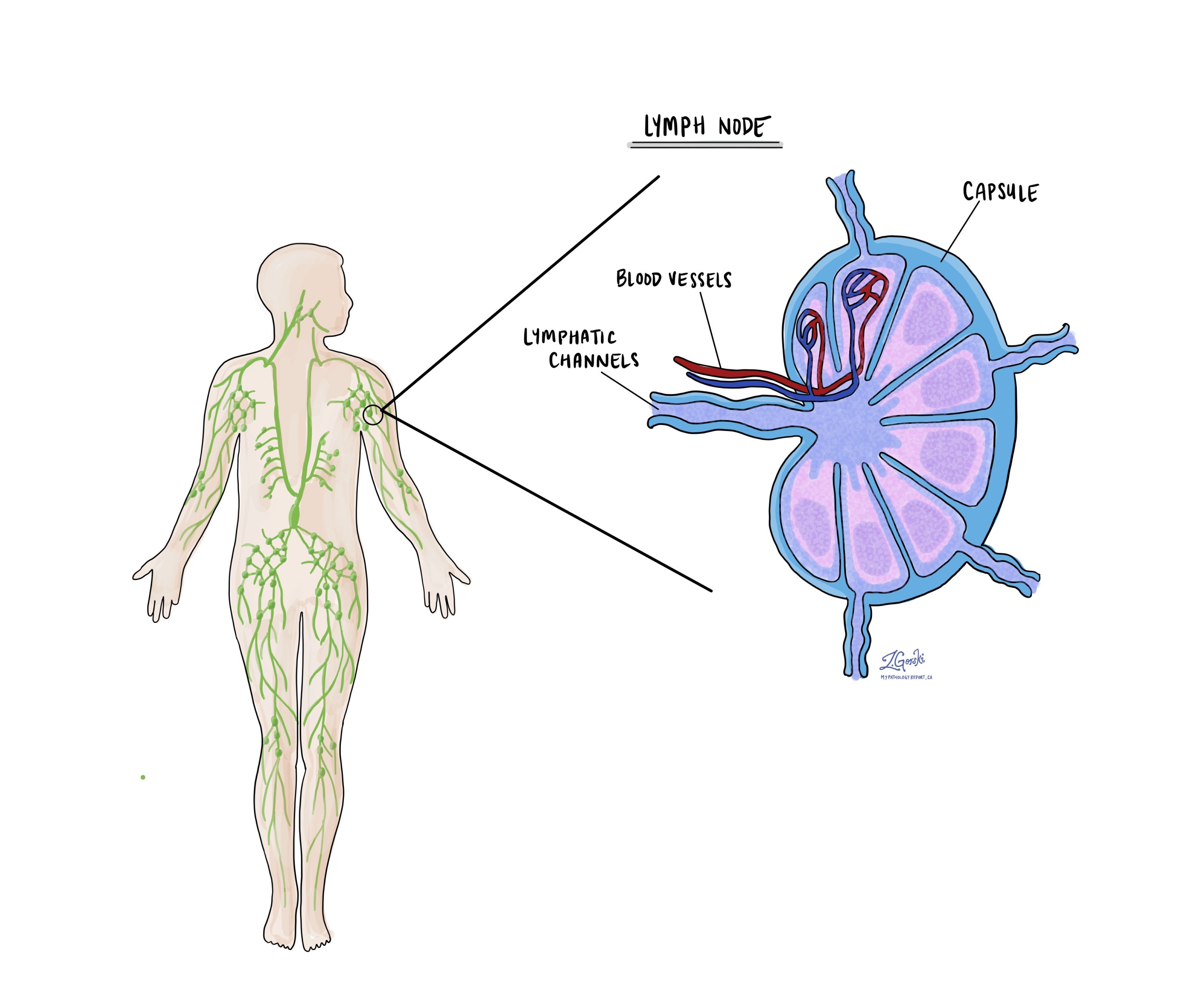
Cancer cells typically spread first to lymph nodes close to the tumour, although lymph nodes far away from the tumour can also be involved. For this reason, the first lymph nodes removed are usually close to the tumour. Lymph nodes further away from the tumour are only typically removed if they are enlarged and there is a high clinical suspicion that there may be cancer cells in the lymph node.
A neck dissection is a surgical procedure performed to remove lymph nodes from the neck. The lymph nodes removed usually come from different neck areas, and each area is called a level. The levels in the neck include 1, 2, 3, 4, and 5. Your pathology report will often describe how many lymph nodes were seen in each level sent for examination. Lymph nodes on the same side as the tumour are called ipsilateral, while those on the opposite side of the tumour are called contralateral.

If any lymph nodes are removed from your body, they will be examined under the microscope by a pathologist, and the examination results will be described in your report. “Positive” means that cancer cells were found in the lymph node. “Negative” means that no cancer cells were found. If cancer cells are found in a lymph node, the size of the largest group of cancer cells (often described as “focus” or “deposit”) may also be included in your report. Extranodal extension means that the tumour cells have broken through the capsule on the outside of the lymph node and have spread into the surrounding tissue.
The examination of lymph nodes is important for two reasons. First, this information determines the pathologic nodal stage (pN). Second, finding cancer cells in a lymph node increases the risk that cancer cells will be found in other parts of the body in the future. As a result, your doctor will use this information when deciding if additional treatment, such as radioactive iodine, chemotherapy, radiation therapy, or immunotherapy, is required.
Genetic changes in minimally invasive encapsulated follicular variant papillary thyroid carcinoma
Like many cancers, minimally invasive encapsulated follicular variant papillary thyroid carcinoma often involves changes in the DNA of thyroid cells. These changes allow the cells to grow faster and under less control than normal cells.
Some of the common genetic changes associated with this type of cancer include:
- BRAF mutations: While BRAF mutations, particularly the BRAF V600E mutation, are highly prevalent in classic variant papillary thyroid carcinoma, their frequency can vary in minimally invasive encapsulated follicular variant papillary thyroid carcinoma. This mutation leads to the activation of the MAPK signalling pathway, promoting tumour growth and progression.
- RAS mutations: Mutations in RAS genes (NRAS, HRAS, KRAS) are more commonly associated with follicular-patterned thyroid cancers, including minimally invasive encapsulated follicular variant papillary thyroid carcinoma. These mutations also activate the MAPK pathway, albeit through a different mechanism than BRAF mutations, and are linked to tumour proliferation and differentiation.
- TERT promoter mutations: Mutations in the promoter region of the TERT gene can be found in minimally invasive encapsulated follicular variant papillary thyroid carcinoma. These mutations increase telomerase activity, allowing cancer cells to maintain their telomere length and continue dividing indefinitely.
- PIK3CA mutations and PTEN loss: Alterations affecting the PI3K/AKT pathway, including PIK3CA mutations and loss of PTEN expression, can occur in minimally invasive encapsulated follicular variant papillary thyroid carcinoma. These changes lead to enhanced cell survival, growth, and metabolism.
- RET/PTC rearrangements: While less common in minimally invasive encapsulated follicular variant papillary thyroid carcinoma compared to classic variant papillary thyroid carcinoma, RET/PTC rearrangements can occur. These genetic alterations result in the fusion of the RET tyrosine kinase with different partner genes, driving oncogenic signalling.
The presence of these genetic changes influences the tumour’s behaviour, response to therapy, and prognosis. For example, tumours with BRAF V600E mutations or TERT promoter mutations tend to have more aggressive behaviour and a poorer prognosis. Understanding the genetic alterations in minimally invasive encapsulated follicular variant papillary thyroid carcinoma is important for guiding treatment decisions, including the potential use of targeted therapies, and for assessing the risk of disease progression and recurrence.
Prognosis for patients diagnosed with minimally invasive follicular variant papillary thyroid carcinoma
The prognosis for patients with minimally invasive follicular variant papillary thyroid carcinoma is generally very good. Most patients have an excellent outcome with appropriate treatment, typically surgery and, in some cases, radioactive iodine therapy. The five-year survival rate for this type of cancer is over 95%. Factors influencing prognosis include the size of the tumour, whether it has spread beyond the thyroid, and the patient’s age and overall health.
Pathologic features that impact prognosis:
- Tumour size: Smaller tumours (less than 4 cm) tend to have a better prognosis. Larger tumours may indicate a more aggressive disease and a higher risk of spreading to other body parts.
- Extrathyroidal extension: Tumours that grow beyond the border of the thyroid gland into the surrounding soft tissues are more likely to recur after surgery and to spread to other parts of the body.
- Lymph node involvement: If the cancer has spread to the lymph nodes in the neck, it can affect the prognosis. However, even with lymph node involvement, many patients still have a good outcome with appropriate treatment.
- BRAF mutation status: The presence of certain genetic mutations, such as the BRAF mutation, can impact prognosis and treatment decisions. Follicular variant papillary thyroid carcinoma often lacks this mutation, which is commonly found in classic variant papillary thyroid carcinoma, and this can be associated with a more favourable prognosis.
Pathologic stage (pTNM)
The pathologic stage for minimally invasive encapsulated follicular variant papillary thyroid carcinoma can only be determined after the entire tumour has been surgically removed and examined under the microscope by a pathologist. The stage is divided into three parts: tumour stage (pT) which describes the tumour, nodal stage (pN) which describes any lymph nodes examined, and metastatic stage (pM) which describes tumour cells that have spread to other parts of the body. The overall pathologic stage is important because it helps your doctor determine the best treatment plan and predict the outlook for recovery.
Tumour stage (pT)
- T0: No evidence of primary tumour.
- T1: The tumour is 2 cm (about 0.8 inches) or smaller in its greatest dimension and confined to the thyroid.
- T1a: The tumour is 1 cm (about 0.4 inches) or smaller.
- T1b: The tumour is larger than 1 cm but not larger than 2 cm.
- T2: The tumour is larger than 2 cm but not larger than 4 cm (about 1.6 inches) and is still inside the thyroid.
- T3: The tumour is larger than 4 cm or has minimal extension beyond the thyroid gland.
- T3a: The tumour is larger than 4 cm but is still confined to the thyroid.
- T3b: The tumour shows gross extrathyroidal extension (it has spread into the muscles outside of the thyroid).
- T4: This indicates advanced disease.
- T4a: The tumour extends beyond the thyroid capsule to invade subcutaneous soft tissues, the larynx (voice box), trachea (windpipe), esophagus (food pipe), or recurrent laryngeal nerve (a nerve that controls the voice box).
- T4b: The tumour invades prevertebral space (area in front of the spinal column), and encases the carotid artery or the mediastinal vessels (major blood vessels).
Nodal stage (pN)
- N0: No regional lymph node metastasis (the cancer hasn’t spread to nearby lymph nodes).
- N1: There is metastasis to regional lymph nodes (near the thyroid).
- N1a: Metastasis is limited to lymph nodes around the thyroid (pretracheal, paratracheal, prelaryngeal/Delphian, and/or perithyroidal lymph nodes).
- N1b: Metastasis to other cervical (neck) or superior mediastinal lymph nodes (lymph nodes in the upper chest).




