by Bibianna Purgina MD FRCPC
August 9, 2024
Background:
Leiomyosarcoma is a type of cancer that starts in smooth muscle cells. Smooth muscle is the type of muscle that is found in many parts of the body, including the walls of blood vessels, the digestive tract, and the uterus. Unlike the muscles that move our arms and legs, smooth muscle works without us thinking about it, helping to move food through the digestive system and control blood flow. Leiomyosarcoma is a rare cancer that can occur anywhere in the body where smooth muscle is found, but it most commonly affects the uterus, abdomen, or blood vessels.
What are the symptoms of leiomyosarcoma?
The symptoms of leiomyosarcoma can vary depending on the location of the tumour. Common symptoms include:
- A lump or swelling: This is often the first sign of leiomyosarcoma. The lump may or may not be painful.
- Pain: Pain may occur if the tumour presses on nearby nerves or organs.
- Unexplained weight loss: Losing weight without trying can be a sign of many types of cancer, including leiomyosarcoma.
- Fatigue: Feeling unusually tired or weak is a common symptom in many cancers.
- Bleeding: If the tumour is in the uterus or digestive tract, it may cause abnormal bleeding.
What causes leiomyosarcoma?
Leiomyosarcoma is caused by changes (mutations) in the DNA of smooth muscle cells. These mutations cause the cells to grow uncontrollably, leading to the formation of a tumour. Most cases of leiomyosarcoma occur sporadically, meaning they happen by chance and are not inherited. However, some cases may be associated with genetic conditions that increase the risk of developing certain types of cancer.
How is this diagnosis made?
The diagnosis of leiomyosarcoma is usually made after a biopsy or surgery to remove the tumour. During these procedures, a small tumour sample is taken and examined under a microscope by a pathologist. The pathologist looks for specific features in the cells that are characteristic of leiomyosarcoma. Additional tests, such as immunohistochemistry (IHC), may also be performed to help confirm the diagnosis.
Histologic types of leiomyosarcoma
Pathologists classify leiomyosarcoma into three histologic types based on how the tumour cells look under the microscope:
- Well differentiated: In this type, the tumour cells look fairly similar to normal smooth muscle cells. Well differentiated leiomyosarcoma tends to grow more slowly and may have a better prognosis.
- Conventional: This is the most common type of leiomyosarcoma. The tumour cells look more abnormal than in well differentiated leiomyosarcoma, and the tumour may grow more quickly.
- Poorly differentiated/pleomorphic: In this type, the tumour cells look very different from normal cells. Poorly differentiated/pleomorphic leiomyosarcoma tends to be more aggressive and may be more likely to spread to other body parts.
French Federation of Cancer Centres Sarcoma Grading System (FNCLCC)
The French Federation of Cancer Centres Sarcoma Grading system, or FNCLCC, is a system that pathologists use to grade sarcomas like leiomyosarcoma. The grade is important because it helps predict how the tumour is likely to behave, including how fast it might grow and whether it might spread to other parts of the body.
The FNCLCC system assigns a score to the tumour based on three components:
- Mitotic activity: This refers to the number of cells that are actively dividing in the tumour. A higher number of dividing cells means a higher mitotic activity score. For this system, pathologists count the number of mitotic figures in 5 mm2 of tissue.
- Necrosis: Necrosis means the death of cells or tissue. In this context, it refers to areas of the tumour where the cells have died. More necrosis usually indicates a more aggressive tumour.
- Differentiation: Differentiation refers to how much the tumour cells look like normal cells. The more the tumour cells differ from normal cells, the higher the differentiation score. In the FNCLCC system, well differentiated leiomyosarcoma receives a score of 1, conventional leiomyosarcoma receives a score of 2, and poorly differentiated/pleomorphic leiomyosarcoma receives a score of 3.
The scores from these three components are added together to give the tumour an overall grade, which can range from Grade 1 (low grade) to Grade 3 (high grade). A higher grade indicates a more aggressive tumour that is more likely to spread.
Microscopic features of leiomyosarcoma
Under the microscope, leiomyosarcoma comprises abnormal-looking spindle cells, which are long and thin, arranged in long intersecting fascicles (bundles). The tumour cells often have hyperchromatic (dark-staining) and pleomorphic (variably shaped) nuclei, which means the nuclei look very different from normal smooth muscle cells. In some cases, the tumour cells may also show bright pink intranuclear pseudo-inclusions, which are projections of the cytoplasm (cell body) into the nucleus. These features help pathologists distinguish leiomyosarcoma from other types of tumours.

Immunohistochemistry
Immunohistochemistry (IHC) is a special test that pathologists use to help identify the type of tumour. It involves applying special markers to the tissue sample that stick to specific proteins in the cells. For leiomyosarcoma, common tested markers include SMA (smooth muscle actin), desmin, and h-caldesmon. These markers are typically positive in leiomyosarcoma, which helps confirm the diagnosis. Pathologists may also test for markers like CD34 and S100, which are usually negative in leiomyosarcoma, to help rule out other types of tumours.
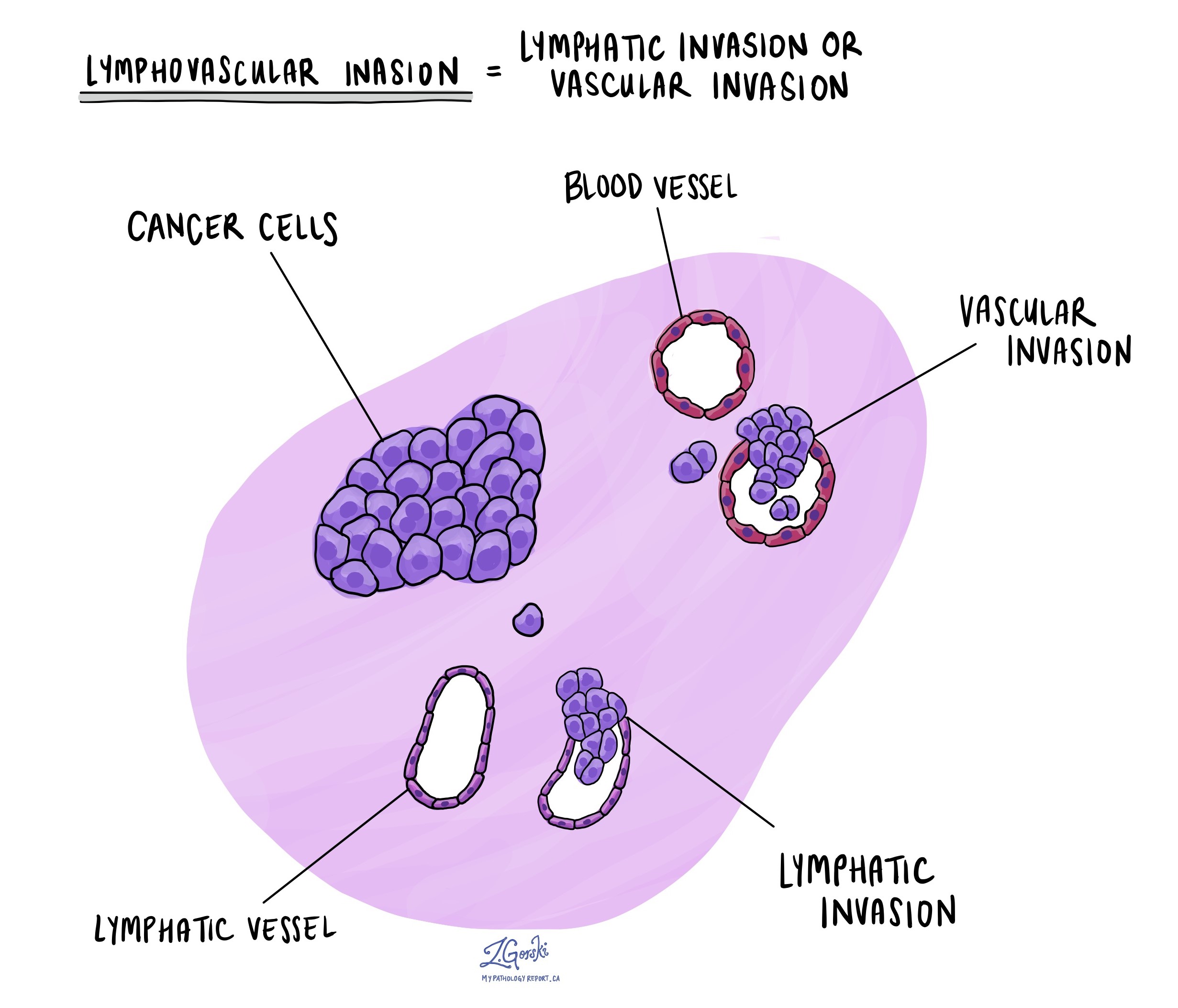
Lymphovascular invasion
Lymphovascular invasion occurs when cancer cells invade a blood vessel or lymphatic vessel. Blood vessels are thin tubes that carry blood throughout the body, unlike lymphatic vessels, which carry a fluid called lymph instead of blood. These lymphatic vessels connect to small immune organs known as lymph nodes scattered throughout the body. Lymphovascular invasion is important because it spreads cancer cells to other body parts, including lymph nodes or the liver, via the blood or lymphatic vessels.
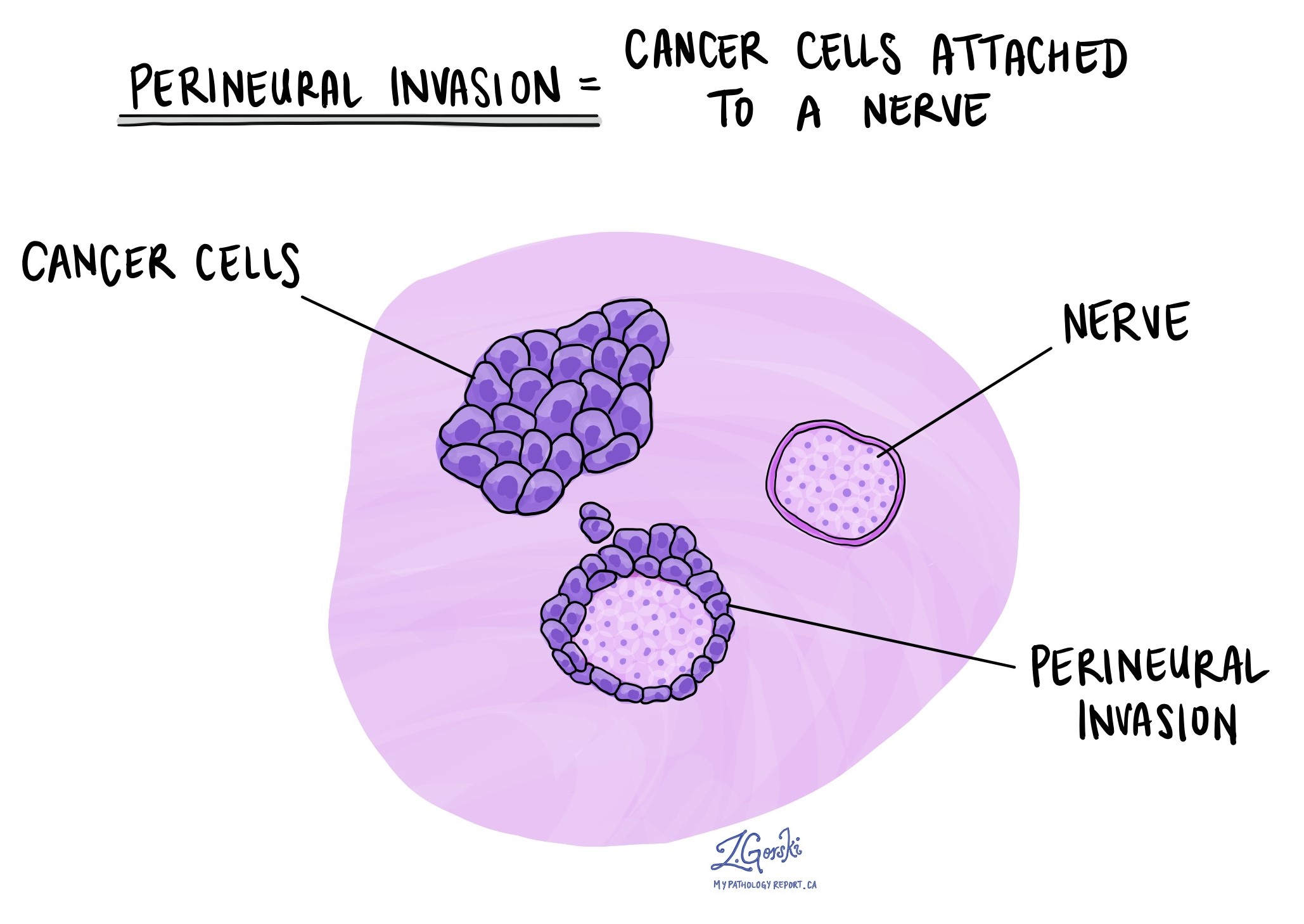
Perineural invasion
Pathologists use the term “perineural invasion” to describe a situation where cancer cells attach to or invade a nerve. “Intraneural invasion” is a related term that specifically refers to cancer cells found inside a nerve. Nerves, resembling long wires, consist of groups of cells known as neurons. These nerves, present throughout the body, transmit information such as temperature, pressure, and pain between the body and the brain. The presence of perineural invasion is important because it allows cancer cells to travel along the nerve into nearby organs and tissues, raising the risk of the tumour recurring after surgery.
Margins
In pathology, a margin is the edge of tissue removed during tumour surgery. The margin status in a pathology report is important as it indicates whether the entire tumour was removed or if some was left behind. This information helps determine the need for further treatment.
Pathologists typically assess margins following a surgical procedure, like an excision or resection, that removes the entire tumour. Margins aren’t usually evaluated after a biopsy, which removes only part of the tumour. The number of margins reported and their size—how much normal tissue is between the tumour and the cut edge—vary based on the tissue type and tumour location.
Pathologists examine margins to check if tumour cells are present at the tissue’s cut edge. A positive margin, where tumour cells are found, suggests that some cancer may remain in the body. In contrast, a negative margin, with no tumour cells at the edge, suggests the tumour was fully removed. Some reports also measure the distance between the nearest tumour cells and the margin, even if all margins are negative.

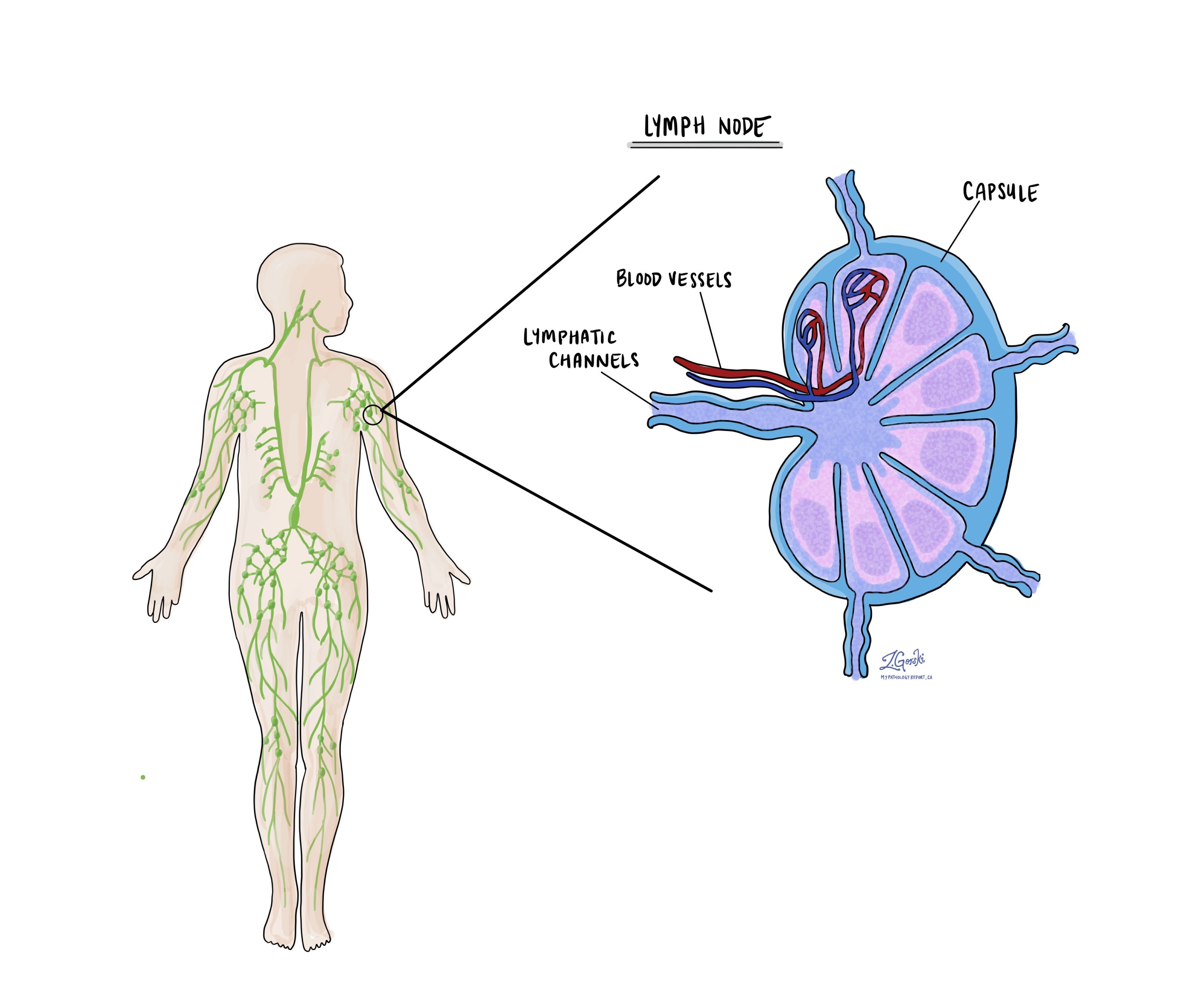
Lymph nodes
Small immune organs, known as lymph nodes, are located throughout the body. Cancer cells can travel from a tumour to these lymph nodes via tiny lymphatic vessels. For this reason, doctors often remove and microscopically examine lymph nodes to look for cancer cells. This process, where cancer cells move from the original tumour to another body part, like a lymph node, is termed metastasis.
Cancer cells usually first migrate to lymph nodes near the tumour, although distant lymph nodes may also be affected. Consequently, surgeons typically remove lymph nodes closest to the tumour first. They might remove lymph nodes farther from the tumour if they are enlarged and there’s a strong suspicion they contain cancer cells.
Pathologists will examine any lymph nodes that have been removed under a microscope, and the findings will be detailed in your report. A “positive” result indicates the presence of cancer cells in the lymph node, while a “negative” result means no cancer cells were found. If the report finds cancer cells in a lymph node, it might also specify the size of the largest cluster of these cells, often referred to as a “focus” or “deposit.” Extranodal extension occurs when tumour cells penetrate the lymph node’s outer capsule and spread into the adjacent tissue.
Examining lymph nodes is important for two reasons. First, it helps determine the pathologic nodal stage (pN). Second, discovering cancer cells in a lymph node suggests an increased risk of later finding cancer cells in other body parts. This information guides your doctor in deciding whether you need additional treatments, such as chemotherapy, radiation therapy, or immunotherapy.
Pathologic stage (pTNM)
The pathologic stage for leiomyosarcoma is based on the TNM staging system, an internationally recognized system created by the American Joint Committee on Cancer. This system uses information about the primary tumour (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathologic stage (pTNM). Your pathologist will examine the tissue submitted and give each part a number. In general, a higher number means a more advanced disease and a worse prognosis.
Tumour stage (pT) for leiomyosarcoma
The tumour stage for leiomyosarcoma varies based on the area of the body where the tumour started. For example, a 5-centimetre tumour that starts in the head or neck will be given a different tumour stage than a tumour that starts deep in the back of the abdomen (the retroperitoneum). However, in most body sites, the tumour stage includes the tumour size and whether the tumour has grown into surrounding body parts.
Tumours in the head and neck
T1 – The tumour is no greater than 2 centimetres in size.
T2 – The tumour is between 2 and 4 centimetres in size.
T3 – The tumour is greater than 4 centimetres in size.
T4 – The tumour has grown into surrounding tissues such as the bones of the face or skull, the eye, the larger blood vessels in the neck, or the brain.
Tumours on the chest, back, or stomach and the arms or legs (trunk and extremities)
T1 – The tumour is no greater than 5 centimetres in size.
T2 – The tumour is between 5 and 10 centimetres in size.
T3 – The tumour is between 10 and 15 centimetres in size.
T4 – The tumour is greater than 15 centimetres in size.
Tumours in the abdomen, including the digestive tract and organs inside the chest (thoracic visceral organs)
T1 – The tumour is only seen in one organ.
T2 – The tumour has grown into the connective tissue surrounding the organ from which is started.
T3 – The tumour has grown into at least one other organ.
T4 – Multiple tumours are found.
Tumours in the retroperitoneum (back of the abdomen)
T1 – The tumour is no greater than 5 centimetres in size.
T2 – The tumour is between 5 and 10 centimetres in size.
T3 – The tumour is between 10 and 15 centimetres in size.
T4 – The tumour is greater than 15 centimetres in size.
Tumours around the eye
T1 – The tumour is no greater than 2 centimetres in size.
T2 – The tumour is greater than 2 centimetres in size but has not grown into the bones surrounding the eye.
T3 – The tumour has grown into the bones surrounding the eye or other bones of the skull.
T4 – The tumour has grown into the eye (the globe) or the surrounding tissues such as the eyelids, sinuses, or brain.
Nodal stage (pN) for leiomyosarcoma
Leiomyosarcoma is given a nodal stage between 0 and 1 based on the presence or absence of cancer cells in one or more lymph nodes. If no cancer cells are seen in any lymph nodes, the nodal stage is N0. If no lymph nodes are sent for pathological examination, the nodal stage cannot be determined, and the nodal stage is listed as NX. If cancer cells are found in any lymph nodes, then the nodal stage is listed as N1.


