by Jason Wasserman MD PhD FRCPC
March 18, 2026
A sentinel lymph node biopsy is a surgical procedure that removes one or two lymph nodes, most likely the first stop for cancer cells spreading from a tumour. The removed nodes are sent to a pathology laboratory where a pathologist examines them carefully under the microscope. The resulting pathology report tells your medical team whether cancer has begun to spread through the lymphatic system — information that is critical for staging your cancer, planning treatment, and understanding your prognosis.
This article explains what sentinel lymph nodes are, how the procedure works, how the laboratory examines the tissue, and what the findings in your report mean.
What are lymph nodes, and what do they do?
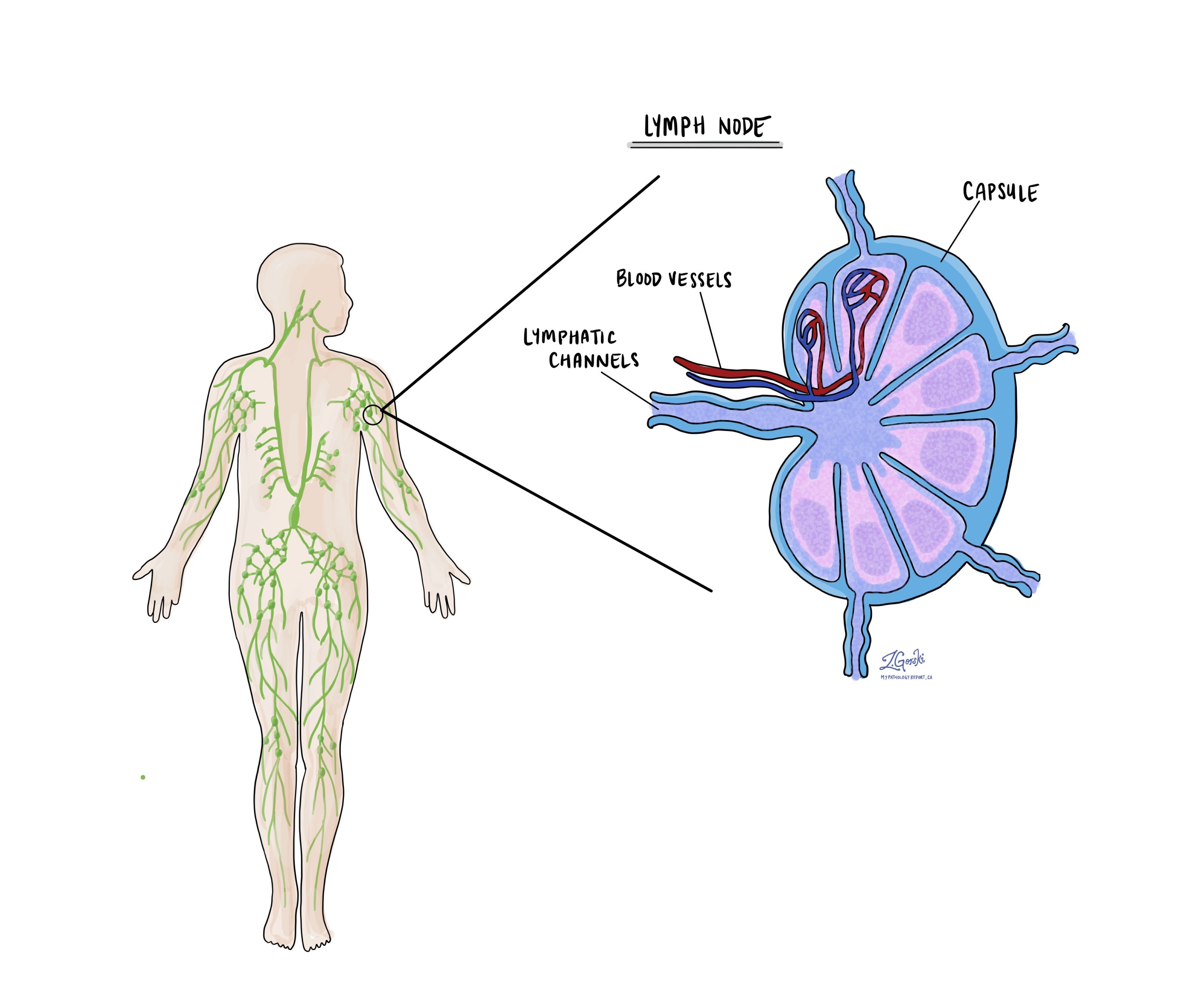
Lymph nodes are small, bean-shaped structures scattered throughout the body that form part of the lymphatic system. The lymphatic system is a network of vessels and organs that helps fight infection and remove waste products from the body’s tissues. Lymphatic vessels carry a fluid called lymph from the tissues back toward the bloodstream. Along the way, lymph passes through lymph nodes, where immune cells monitor the fluid for signs of infection or disease.
In cancer, the lymphatic system can act as a highway for cancer cells to travel away from the original tumour. When cancer spreads to a lymph node, it is called metastasis. Knowing whether cancer has reached the lymph nodes is one of the most important pieces of information in cancer staging because it affects how likely the cancer is to have spread further, and what treatment is needed.
What is a sentinel lymph node?
The sentinel lymph node is the first lymph node or small group of nodes that drains lymph directly from the area of the tumour. It is the first checkpoint that cancer cells would reach if they left the tumour and entered the lymphatic system. The idea behind sentinel lymph node biopsy is straightforward: if cancer has not yet reached the sentinel node — the first place it would go — then it is very unlikely to have spread to any other lymph nodes further along the drainage pathway.
The location of the sentinel node depends on the location of the tumour. Common examples include:
- Breast cancer. The sentinel nodes are almost always located in the armpit (axilla), and sometimes near the breastbone (internal mammary chain).
- Melanoma of the skin. The sentinel nodes are in the nearest lymph node basin — the armpit for tumours on the arm or upper trunk, the groin for tumours on the leg or lower trunk, and the neck for tumours on the head or face.
- Vulvar cancer. The sentinel nodes are typically in the groin (inguinal region).
- Endometrial (uterine) cancer. The sentinel nodes are found in the pelvis, along major blood vessels.
- Oral cavity cancers. The sentinel nodes are located in the neck.
How is a sentinel lymph node biopsy performed?
The procedure is almost always performed at the same time as the surgical removal of the primary tumour, though in some cases it is done as a separate procedure beforehand.
To identify the sentinel node, the surgical team injects a tracer — a radioactive substance, a blue dye, or both — into the tissue around the tumour before or during the operation. The tracer travels through the lymphatic vessels in the same direction as cancer cells and collects in the sentinel node first. The surgeon locates the sentinel node using a handheld probe that detects radioactivity, by looking for the blue-stained node, or by both methods. Once identified, the sentinel node or nodes are removed through a small incision and immediately sent to the pathology laboratory.
By removing only the sentinel node rather than all the lymph nodes in the region, this technique avoids the complications of extensive lymph node removal, particularly lymphedema — a long-term swelling of the limb caused by disruption of lymphatic drainage.
What does the pathology laboratory do with sentinel lymph nodes?
Sentinel lymph nodes are examined with much greater care than routine lymph nodes because the result is so critical to staging and treatment decisions. The standard processing is more thorough than for lymph nodes removed in other surgical procedures.
Gross examination
The pathologist first examines the node with the naked eye, measuring its size and noting any visible abnormalities such as firm white areas that might represent cancer deposits. This is called the gross description.
Sectioning and microscopic examination
The node is sliced into thin sections, which are embedded in paraffin wax, mounted on glass slides, and stained. For sentinel nodes, pathologists typically examine multiple levels through each section — meaning they cut and examine the slides at several depths rather than looking at a single slice. This significantly increases the likelihood of detecting small cancer deposits that might be missed in a single section.
Immunohistochemistry
If the initial stained slides do not show cancer but features raise concern, or if the clinical situation warrants it, the pathologist may apply immunohistochemistry — special stains that use antibodies to detect proteins expressed by cancer cells. For breast cancer, the most commonly used markers are cytokeratin stains such as CK7 or AE1/AE3, which highlight epithelial (carcinoma) cells and make even very small deposits of cancer visible against the background of normal lymph node tissue. For melanoma, markers such as Melan-A, S100, and HMB-45 are used.
Intraoperative (frozen section) analysis
In some hospitals and for some cancer types, the sentinel node is also examined during the operation itself using a technique called frozen section. A small piece of the node is rapidly frozen, sliced, and examined under the microscope while the patient is still in the operating room. If cancer is found, the surgeon can immediately perform a more extensive lymph node removal in the same operation, avoiding a second procedure. However, intraoperative analysis is less sensitive than the more detailed analysis performed after the operation, so a negative frozen section does not definitively rule out cancer in the sentinel node.
What does the sentinel lymph node report contain?
The pathology report for a sentinel lymph node biopsy describes several important features. Understanding what each term means will help you read your report and have a more informed conversation with your doctor.
Number of nodes examined
The report will state how many sentinel nodes were removed and examined. Typically, one to three nodes are removed, though occasionally more are identified. Each node is examined individually, and the findings in each are reported separately.
Negative result
A negative sentinel lymph node means that no cancer cells were found in any of the nodes examined after thorough examination of multiple sections and, where appropriate, immunohistochemistry. This is the most favorable result. A negative sentinel node indicates that cancer has not been detected in the lymphatic drainage pathway of the tumour and significantly reduces the likelihood that cancer has spread to other lymph nodes or distant organs.
A negative result does not provide a guarantee that no cancer cells exist anywhere in the lymphatic system — no test is perfect — but it is a very reassuring finding and, in most cancer types, spares the patient from more extensive lymph node surgery.
Positive result — and the size of the deposit
If cancer cells are found in the sentinel node, the report will state that the result is positive and specify the size of the deposit. The size of the cancer deposit in the lymph node is one of the most important aspects of the report because it directly influences staging and treatment decisions. Cancer deposits in lymph nodes are classified into three categories based on size:
- Isolated tumour cells (ITCs)—the smallest category. An isolated tumour cell deposit consists of a single cell or a cluster of fewer than 200 cells, measuring 0.2 millimetres or less. Isolated tumour cells are detected only because of the thorough multi-level examination and immunohistochemistry routinely applied to sentinel nodes — they would rarely be found in a standard lymph node examination. In many cancer types, particularly early-stage breast cancer and endometrial cancer, the presence of isolated tumour cells does not change the nodal stage. It does not routinely prompt additional lymph node surgery, though your doctor will discuss this with you based on your specific situation.
- Micrometastasis. A cancer deposit measuring more than 0.2 millimetres but no more than 2 millimetres. Micrometastases are a genuine finding of cancer spread but represent early, small-volume nodal involvement. In breast cancer, a micrometastasis changes the nodal stage to pN1mi. Whether additional lymph node surgery or changes to systemic treatment are needed depends on the overall clinical picture, including tumour size, grade, and receptor status.
- Macrometastasis. A cancer deposit measuring more than 2 millimetres. This is the largest category and represents a clearly established spread to the lymph node. Macrometastasis changes the nodal stage to pN1 or higher, depending on the number of involved nodes. It typically has a more significant impact on staging and treatment decisions than a micrometastasis.
Extranodal extension
If cancer is present in the sentinel node, the pathologist will also assess whether the cancer has broken through the outer capsule of the lymph node and spread into the surrounding fatty tissue. This is called extranodal extension (ENE).
Extranodal extension is a sign of more aggressive cancer behaviour and is associated with a higher risk of the cancer recurring after treatment. Its presence can raise the cancer stage and often leads to more intensive treatment, such as radiation therapy directed at the lymph node region. The report may describe extranodal extension as microscopic (visible only under the microscope) or gross (visible to the naked eye). It may note the distance that cancer has spread beyond the capsule, as this measurement can influence treatment planning in certain cancer types, particularly head and neck cancers.
Number of positive nodes
The report will state how many of the sentinel nodes examined contained cancer. For example, “1 of 2 sentinel lymph nodes contains metastatic carcinoma” means that one node was positive and one was negative. The number of positive nodes contributes directly to the nodal stage (pN stage) of the cancer.
How do sentinel lymph node results differ by cancer type?
While the general principles of sentinel lymph node biopsy apply across cancer types, the implications of specific findings — and what happens next — vary by cancer type.
Breast cancer
Sentinel lymph node biopsy has largely replaced routine axillary lymph node dissection as the standard of care for early-stage invasive breast carcinoma. For most patients with a negative sentinel node, no further lymph node surgery is needed. For patients with a macrometastasis, further surgery to remove additional axillary lymph nodes (axillary lymph node dissection) was previously routine. Still, current evidence suggests this can often be avoided in patients receiving systemic therapy, and radiation may be used instead. The sentinel node result is incorporated into the overall pathological staging of breast cancer alongside tumour size, grade, and hormone receptor and HER2 status.
Melanoma
Sentinel lymph node biopsy is a standard staging procedure for melanoma of a significant thickness (typically greater than 0.8 mm, or thinner with certain high-risk features such as a high mitotic rate or ulceration). A positive sentinel node in melanoma significantly changes the stage from Stage II to Stage III disease. It may prompt discussion of adjuvant systemic therapy such as immunotherapy or targeted therapy. For melanoma, the size threshold for a positive result differs slightly from that of breast cancer, and the specific location and size of the deposit within the node are both reported and considered in treatment planning.
Endometrial (uterine) cancer
Sentinel lymph node biopsy is increasingly used in the staging of endometrial carcinoma as an alternative to complete pelvic lymph node dissection. The procedure maps drainage from the uterus to the pelvic lymph nodes. A positive sentinel node changes the stage to Stage IIIC disease and typically leads to additional treatment such as radiation therapy.
Vulvar cancer
Sentinel lymph node biopsy is standard for early-stage vulvar cancers, avoiding the significant morbidity of complete groin lymph node dissection in patients whose sentinel nodes are negative. A positive sentinel node in vulvar cancer is an important prognostic finding and typically prompts groin radiation therapy.
What happens after the sentinel lymph node biopsy report?
Once your doctor has reviewed the sentinel lymph node report alongside the findings from the primary tumour, they will discuss the complete pathological staging with you and explain how it affects your treatment plan.
A negative sentinel node result is reassuring and, in most cancer types, means no further lymph node surgery is needed. Your treatment plan will focus on the primary tumour findings.
A positive sentinel node result means cancer has spread at least to the regional lymphatic system. The size of the deposit, whether extranodal extension is present, and the number of involved nodes all factor into what additional treatment may be recommended. Depending on your cancer type and stage, this may include additional lymph node surgery, radiation to the lymph node region, systemic therapy such as chemotherapy, hormone therapy, immunotherapy, or targeted therapy, or a combination of these.
Questions to ask your doctor
- How many sentinel lymph nodes were removed and examined?
- Were any sentinel nodes positive for cancer?
- If positive, how large was the cancer deposit — isolated tumour cells, micrometastasis, or macrometastasis?
- Was extranodal extension present?
- How does the sentinel node result change my cancer stage?
- Do I need additional lymph node surgery?
- Does this result change what systemic treatment I will receive?
- Will I need radiation therapy to the lymph node region?
- What is my overall prognosis based on the combined findings of the tumour and lymph nodes?
Related articles on MyPathologyReport.com
- Sentinel lymph node (dictionary definition)
- Lymph node (dictionary definition)
- Isolated tumour cells (ITCs) (dictionary definition)
- Extranodal extension (ENE) (dictionary definition)
- Metastasis (dictionary definition)
- Nodal stage (N stage) (dictionary definition)
- Invasive breast carcinoma
- Invasive ductal carcinoma of the breast
- Invasive lobular carcinoma of the breast
- Endometrial carcinoma


