by Katherina Baranova MD and Matt Cecchini MD FRCPC
May 9, 2023
What is small cell carcinoma of the lung?
Small cell carcinoma is a type of lung cancer. It is made up of neuroendocrine cells that are normally found in the lungs. Small cell carcinoma is considered a very aggressive type of cancer and the tumour cells have often spread to other parts of the body by the time a diagnosis is made. Another name for this type of cancer is small cell neuroendocrine carcinoma.
What are the symptoms of small cell carcinoma of the lung?
The tumour often starts in the central portion of the lung, closest to the larger airways and the heart. As a result, when these cancers grow and start to invade, they can cause narrowing of the airways leading to symptoms of cough and trouble breathing.
Because small cell carcinoma is made up of neuroendocrine cells, the tumour can make and release hormones that can cause patients to have bloodwork abnormalities such as high calcium or low sodium, although these bloodwork changes also have many other causes aside from cancer.
What causes small cell carcinoma?
These cancers develop when cells are damaged (often by the chemicals in cigarette smoke) and start to grow abnormally. The most common cause of this damage is cigarette smoke.
How is small cell carcinoma diagnosed?
The diagnosis of small cell carcinoma is usually made after a small sample of tissue is removed in a procedure called a biopsy or a fine needle aspiration (FNA). The biopsy or FNA may be performed on the lung or another body site such as a lymph node.
What does small cell carcinoma look like under the microscope?
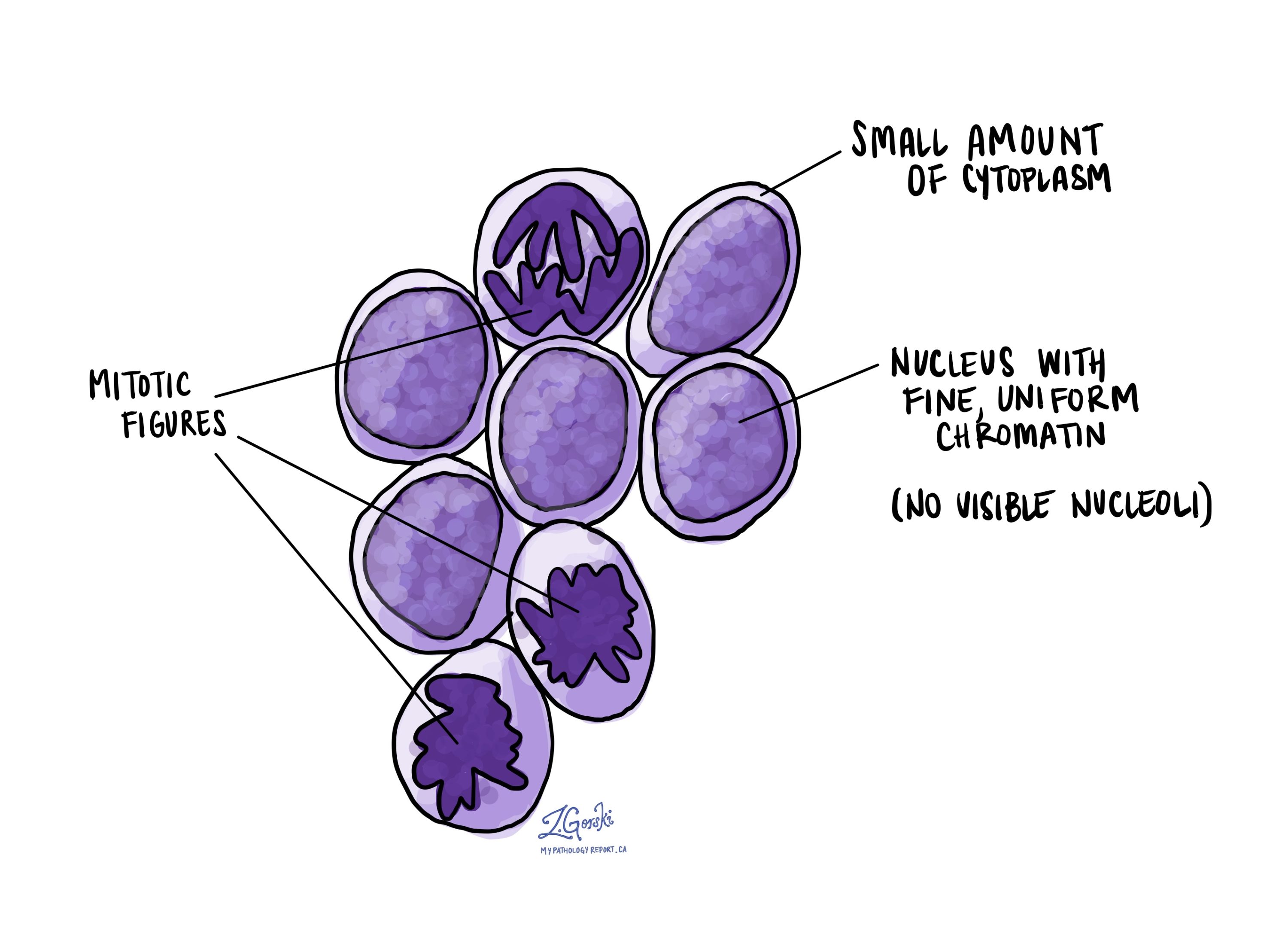
Under the microscope, the tumour cells in small cell carcinoma are smaller than normal cells because they have less material in their cytoplasm (cell body). This also makes the cells look dark blue. Pathologists these cells as hyperchromatic. The chromatin (genetic material) inside the nucleus of the cell is often described as fine or uniform. Large clumps of genetic material called nucleoli are usually not seen.
The tumour cells in small cell carcinoma are constantly dividing to create new tumour cells. This process is called mitosis and a cell that is actively dividing is called a mitotic figure. Pathologists often describe these tumours as having a very high rate of cell proliferation.
What other tests may be ordered to confirm the diagnosis?
Your pathologist may perform a test called immunohistochemistry to confirm the diagnosis. The results will be described as positive (reactive) or negative (non-reactive).
Small cell carcinoma usually shows the following results:
- Chromogranin – Positive.
- Synaptophysin – Positive.
- CD56 – Positive.
- TTF-1 – Positive.
These tests are used to confirm the diagnosis of small cell carcinoma. Your report may not include all the results shown above. In addition, since small cell carcinoma shows a high rate of cell division, the Ki-67 index (a type of immunohistochemistry that highlights dividing cells) is often reported as high.
What is a margin?
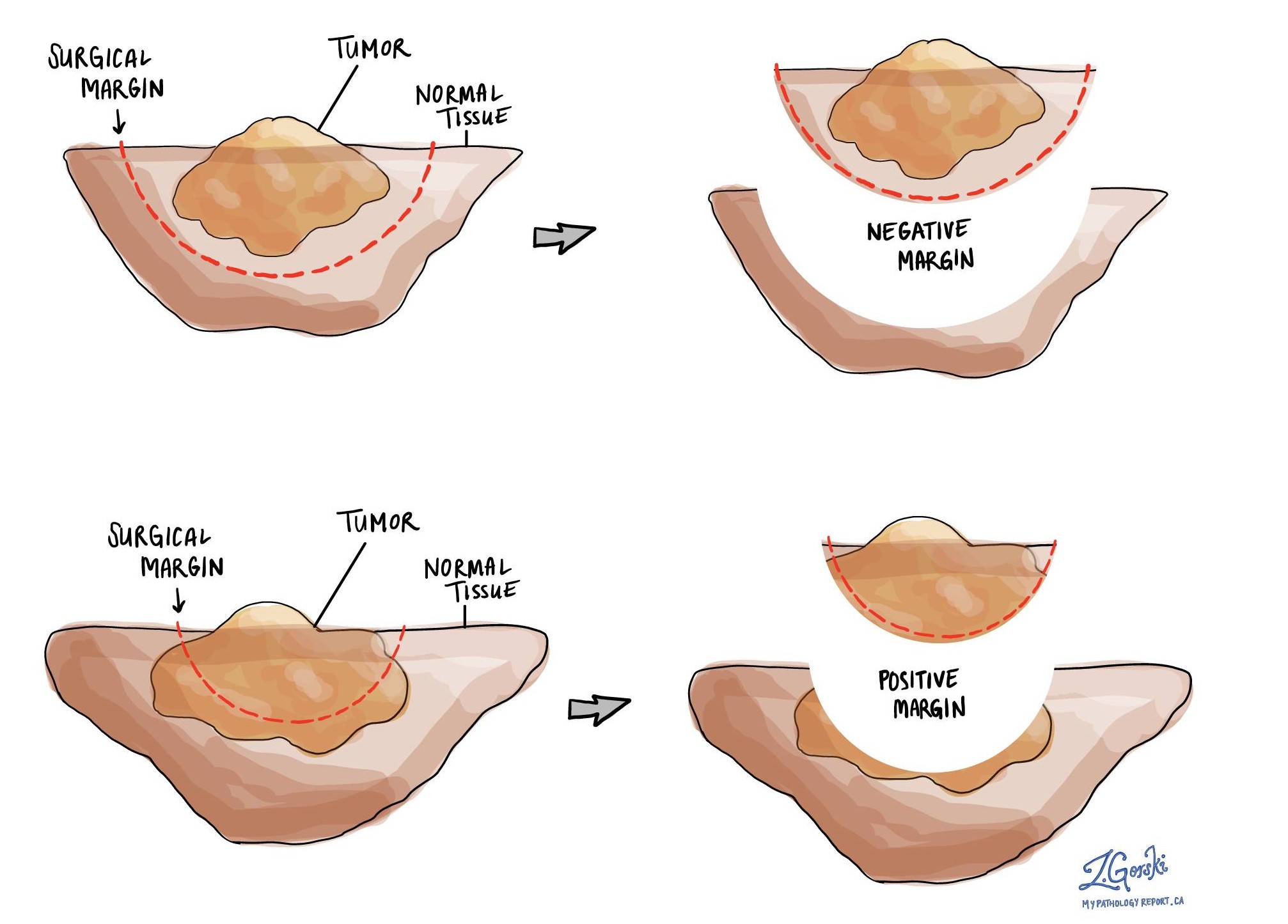
When surgery is performed to remove a tumour from the lungs, normal lung tissue, blood vessels, and airways all have to be cut. Any tissue that is cut when removing a tumour is called a margin and all margins are examined closely for any microscopic evidence of tumour.
For small cell carcinoma, a margin is considered positive when there are tumour cells at the edge of the cut tissue. A positive margin is associated with a higher risk that the tumour will re-grow (local recurrence) in the same site after treatment. If no tumour cells are seen at any of the cut edges of tissue, the margins are called negative. Margins will only be described in your report after the entire tumour has been removed.
Were lymph nodes examined and did any contain cancer cells?
Lymph nodes are small immune organs located throughout the body. Tumour cells can travel from the tumour to a lymph node through lymphatic channels located in and around the tumour. The movement of tumour cells from the tumour to a lymph node is called metastasis.
Lymph nodes from the neck, chest, and lungs may be removed at the same time as the tumour. These lymph nodes are divided into areas called stations. There are 14 different stations in the neck, chest, and lungs. Your pathology report will describe the number of lymph nodes examined from each station.

Stations that may be described in your report:
- Station 1 – Lower cervical, supraclavicular, and sternal notch lymph nodes.
- Station 2 – Upper paratracheal lymph nodes.
- Station 3 – Prevascular and retrotracheal lymph nodes.
- Station 4 – Lower paratracheal lymph nodes.
- Station 5 – Subaortic lymph nodes (aorto-pulmonary window).
- Station 6 – Paraaortic lymph nodes (ascending aorta or phrenic).
- Station 7 – Subcarinal lymph nodes.
- Station 8 – Paraesophageal lymph nodes (below carina).
- Station 9 – Pulmonary ligament lymph nodes.
- Station 10 – Hilar lymph nodes.
- Station 11 – Interlobar lymph nodes.
- Station 12 – Lobar lymph nodes.
- Station 13 – Segmental lymph nodes.
- Station 14 – Subsegmental lymph nodes.
Your pathologist will carefully examine each lymph node for tumour cells. Lymph nodes that contain tumour cells are often called positive while those that do not contain any tumour cells are called negative. If tumour cells are found in a lymph node, the station of the positive lymph node will be described in your report.
Finding tumour cells in a lymph node increases the nodal stage (see Staging below) and is associated with a worse prognosis. The nodal stage selected will depend on where the lymph node with tumour cells was located (the station).
How is small cell carcinoma of the lung staged?
There are two systems currently used to stage small cell carcinoma of the lung. The first system divides the disease into two stages – limited and extensive. The second system is called the TNM staging system and it uses information about the tumour (T), lymph nodes (N), and distant metastatic disease to determine the stage. Both systems are explained in more detail below.
Limited versus extensive stage for small cell carcinoma of the lung
- Limited stage – Limited stage disease means the cancer is found only on one side of the chest – either in part of one lung or in lymph nodes on the same side as the tumour. This stage can be treated with radiation to one side of the body only.
- Extensive stage – Extensive stage disease means the cancer has spread to the other lung, to lymph nodes on the other side of the chest, or to other parts of the body such as the liver, brain, or bone. This stage also includes cases where cancer has spread to fluid around the lung or heart. Most people with small cell lung carcinoma have extensive-stage disease at diagnosis because this type of cancer spreads early and quickly and often does not cause symptoms early on.
TNM stage for small cell carcinoma of the lung
This system uses information about the primary tumour (T), lymph nodes (N), and distant metastatic disease (M) to determine the complete pathologic stage (pTNM). Your pathologist will examine the tissue submitted and give each part a number. In general, a higher number means more advanced disease and a worse prognosis. The pathologic stage will only be described in your report after the entire tumour has been removed. It will not be included after a biopsy.
Tumour stage (pT) for small cell carcinoma of the lung
Small cell carcinoma is given a tumour stage between 1 and 4 based on the size of the tumour, the number of tumours found in the tissue examined, and whether the tumour has broken through the pleural or has spread to organs around the lungs.

Nodal stage (pN) for small cell carcinoma of the lung
Small cell carcinoma is given a nodal stage between 0 and 3 based on the presence or absence of cancer cells in a lymph node and the location of the lymph nodes that contain tumour cells.
- NX – No lymph nodes were sent for pathologic examination.
- N0 – No tumour cells were found in any of the lymph nodes examine
- N1 – Tumour cells were found in at least one lymph node from inside the lung or around the large airways leading into the lung. This stage includes stations 10 through 14.
- N2 – Tumour cells were found in at least one lymph node from the tissue in the middle of the chest and around the large airways. This stage includes stations 7 through 9.
- N3 – Tumour cells were found in the neck or in any lymph nodes on the side of the body opposite (contralateral) to the tumour. This stage includes stations 1 through 6.
Metastatic stage (pM) for small cell carcinoma of the lung
Small cell carcinoma is given a metastatic stage of 0 or 1 based on the presence of tumour cells in the lung on the opposite side of the body or at a distant body site (for example the brain). The metastatic stage can only be determined if tissue from the opposite lung or distant site is sent for pathological examination. Because this tissue is rarely present, the metastatic stage cannot be determined and is listed as pMX.



