by Philip Berardi, MD PhD FRCPC
March 19, 2022
What is follicular lymphoma?
Follicular lymphoma (FL) is a type of cancer that starts from specialized immune cells called B cells. FL is the second most common lymphoma to affect adults.
Where in the body is follicular lymphoma found?
FL can start anywhere in the body where B cells gather in large numbers. The most common locations include lymph nodes, the gastrointestinal tract (in particular the stomach and small bowel), the skin, and the breast.
What are the symptoms of follicular lymphoma?
Patients with FL may notice a painless lump or swelling that slowly increases in size over time. Other symptoms of follicular lymphoma include fatigue, unintentional weight loss, loss of appetite, night sweats, and fever.
What causes follicular lymphoma?
What causes FL is currently unknown. However, a number of risk factors that may increase the chance of developing cFL have been identified. These risk factors include cigarette smoking, hepatitis C infection, Sjogren’s syndrome, obesity, and having a first-degree relative who was previously diagnosed with FL.
How is the diagnosis of follicular lymphoma made?
The diagnosis of FL is usually made after a small piece of tissue is removed in a procedure called a biopsy. The tissue is then sent to a pathologist for examination under the microscope.
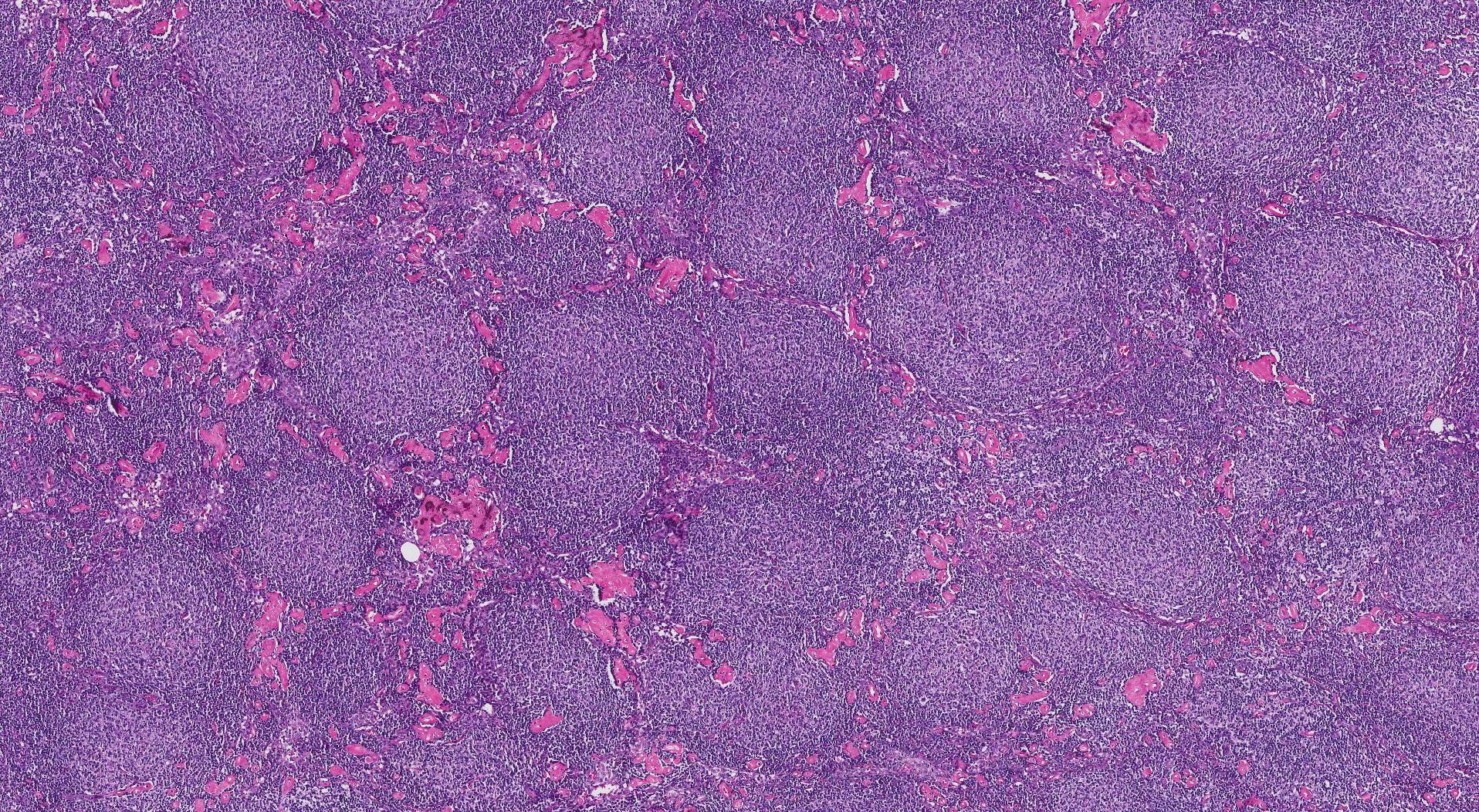
What does follicular lymphoma look like under the microscope?
Most FLs are made up of small, dark cells that look similar to normal B cells. However, some tumours contain larger, more abnormal-looking cells. Pathologists use the term pattern of growth to describe the way the cancer cells are arranged. When the tumour cells are arranged in small round groups the pattern is called follicular. When the tumour cells grow in very large shapeless groups and there is no space between the groups, the pattern is called diffuse. The diffuse pattern is important because it can be associated with a worse prognosis. In particular, if a grade 3B tumour (see Grade below) shows a diffuse pattern of growth, the diagnosis changes from FL to diffuse large B-cell lymphoma (DLBCL).
What other tests may be performed to confirm the diagnosis of follicular lymphoma?
Pathologists often perform immunohistochemistry (IHC) to confirm the diagnosis and exclude other conditions that can look like FL under the microscope. Another test called flow cytometry may also be performed.
IHC is a special test that allows pathologists to learn more about the types of proteins made by different types of cells. Cells that produce a protein are called positive or reactive. Cells that do not produce a protein are called negative or non-reactive.
Follicular lymphoma commonly shows the following immunohistochemistry results:
- CD20 – Positive.
- CD10 – Positive.
- BCL2 – Positive.
- BCL6 – Positive.
- CD23 – Negative.
- CD3 – Negative.
- CD5 – Negative.
- Cyclin D1 – Negative.
What is the Ki-67 labelling index and why is it important?
The Ki-67 labelling index is a way of estimating how quickly cells are dividing. Generally, the quicker the tumour cells divide (the higher the Ki-67 labelling index), the more concerned your doctor will be that your lymphoma will behave aggressively.
How do pathologists grade follicular lymphoma and why is the grade important?
Pathologists use the term grade to describe the difference between the tumour cells in FL and normal B cells. After examining the tumour under the microscope, FL is given a grade from 1 to 3. Grade 3 FL can be further subdivided into grades 3A and 3B.
Pathologists determine the tumour grade by counting the number of large cancer cells called centroblasts in a given area. Tumours with more large cells are given a higher grade.
Grade 1 and grade 2 tumours are grouped together and are referred to as low-grade or grade 1-2 because they tend to grow and spread very slowly. Tumours that behave in this manner are also referred to as indolent. Grade 3 tumours are referred to as high-grade because they tend to behave in a more aggressive manner and are associated with a poorer overall outcome.
Over time, low-grade (grade 1 or grade 2) tumours can change into high-grade (grade 3) tumours. If you develop new symptoms and were initially diagnosed with low-grade FL, your doctor may perform another biopsy to see if the tumour has changed to a higher grade.
What does transformation mean and why is it important for follicular lymphoma?
Over time, some FLs will change to become a more aggressive type of lymphoma called diffuse large B cell lymphoma (DLBCL). This change is called transformation. All tumours are carefully examined for any evidence of transformation and if seen, it will be described in your report.


