by Jason Wasserman MD PhD FRCPC
July 2, 2025
Anaplastic thyroid carcinoma is a rare and very aggressive type of thyroid cancer. Although it starts from the same cells that make up the normal thyroid gland, the tumour cells become so abnormal that they no longer look or behave like typical thyroid cells. For this reason, anaplastic thyroid carcinoma is sometimes called undifferentiated thyroid carcinoma.
This type of cancer grows quickly and often spreads to nearby structures in the neck and other parts of the body. It usually affects older adults, with most people diagnosed between the ages of 65 and 75. It is slightly more common in women than men.
What are the symptoms of anaplastic thyroid carcinoma?
Because anaplastic thyroid carcinoma grows rapidly, people often notice symptoms that develop over a short period of time.
These may include:
-
A rapidly growing lump or mass in the front of the neck.
-
Pain or pressure in the neck.
-
Difficulty swallowing (dysphagia).
-
Difficulty breathing (dyspnea).
-
Hoarseness or voice changes.
-
Cough or feeling of fullness in the throat.
In some cases, anaplastic thyroid carcinoma may also cause symptoms such as fatigue, weight loss, or changes in blood calcium levels (hypercalcemia).
What causes anaplastic thyroid carcinoma?
Doctors do not yet know exactly what causes anaplastic thyroid carcinoma. In many cases, this cancer appears to develop from a pre-existing, slower-growing thyroid cancer, such as papillary thyroid carcinoma or follicular carcinoma. This process is called dedifferentiation, where the original cancer cells lose their usual features and become more aggressive.
Researchers have found that anaplastic thyroid carcinoma often shows a series of genetic changes over time. Some of the most common mutations involve genes such as TP53, TERT, BRAF, and RAS. These changes help explain why the tumour grows so quickly and becomes resistant to treatment.
Certain risk factors may increase the chance of developing this cancer, including:
-
A history of long-standing goiter or thyroid nodules.
-
Prior radiation exposure to the neck.
-
Iodine deficiency.
-
A history of well-differentiated thyroid cancer, such as papillary thyroid carcinoma or follicular carcinoma.
How is anaplastic thyroid carcinoma diagnosed?
The diagnosis usually begins with a physical examination and imaging tests such as an ultrasound or a CT scan. If a suspicious mass is seen, a biopsy is performed—often with a fine-needle aspiration biopsy (FNAB) or core needle biopsy. A pathologist examines the tissue under the microscope and may perform additional tests, such as immunohistochemistry or molecular testing, to confirm the diagnosis.
Microscopic features of anaplastic thyroid carcinoma
When examined under the microscope, anaplastic thyroid carcinoma shows features that reflect its highly aggressive and undifferentiated nature. The tumour cells look very abnormal and bear little to no resemblance to normal thyroid cells. Pathologists use the term undifferentiated to describe this loss of normal structure and appearance.
The tumour may contain a mix of different cell shapes and growth patterns, including:
-
Spindle-shaped cells: Long and thin and often appear loosely arranged in sweeping bundles. These cells may resemble those seen in sarcomas (a type of soft tissue cancer).
-
Epithelioid cells: Rounder, more closely packed, and often form clusters or sheets. These may resemble the cells of other epithelial cancers.
-
Giant cells: Large tumour cells that often contain multiple nuclei. These cells are usually scattered throughout the tumour and are a sign of high-grade, aggressive cancer.
-
Squamous cells: Flat, plate-like cells that may be seen in tumours showing a squamous carcinoma pattern. These tumours may resemble other types of squamous cancers of the head and neck.
Other important microscopic features include:
-
High mitotic activity: This means the tumour cells are dividing rapidly. Pathologists can see many cells in the process of dividing, and often the mitotic figures appear abnormal or atypical. This is a hallmark of aggressive tumours.
-
Tumour necrosis: Large areas of dead tumour cells are frequently seen. Necrosis occurs when the tumour grows so quickly that it outpaces its blood supply.
-
Marked nuclear pleomorphism: The tumour cell nuclei vary widely in size, shape, and appearance. Some are very large, others small, and some contain irregular chromatin (the material that holds genetic information) or prominent nucleoli (small round structures inside the nucleus). This variation is another sign of an aggressive, high-grade tumour.
-
Loss of normal architecture: The tumour does not form the well-organized follicles or gland-like structures seen in normal thyroid tissue or well-differentiated thyroid cancers. Instead, it invades surrounding tissue in a disorganized, sheet-like or infiltrative manner.
-
Inflammatory infiltrate: Many tumours are surrounded by or mixed with immune cells, especially neutrophils, which may be reacting to tumour necrosis or contributing to tumour-related inflammation.
In some cases, the tumour contains small areas of a pre-existing well-differentiated thyroid carcinoma, such as papillary or follicular thyroid carcinoma. These areas may provide a clue that the anaplastic tumour developed from a previously slower-growing thyroid cancer. If present, these components will be mentioned in the pathology report.
These microscopic findings are critical for making the diagnosis and for distinguishing anaplastic thyroid carcinoma from other types of thyroid or neck tumours.
Immunohistochemistry
Immunohistochemistry is a test that uses antibodies to detect specific proteins in tumour cells. This test helps pathologists confirm the diagnosis of anaplastic thyroid carcinoma and distinguish it from other types of cancer.
Typical immunohistochemistry results for anaplastic thyroid carcinoma include:
-
Cytokeratins (proteins found in many epithelial cancers) are often positive in most tumour cells.
-
Thyroid-specific proteins such as thyroglobulin and thyroid transcription factor-1 (TTF-1) are usually negative or only focally positive. This reflects the undifferentiated nature of the tumour.
-
PAX8, a protein normally found in thyroid and kidney cells, may be positive in about half of anaplastic thyroid carcinomas, especially when there is a coexisting differentiated thyroid tumour.
-
p53, a protein involved in controlling cell division, is often abnormally increased in tumour cells, suggesting a mutation in the TP53 gene.
-
Ki-67, a marker of how quickly tumour cells are dividing, is usually very high in anaplastic thyroid carcinoma.
-
In tumours that exhibit a squamous appearance, additional proteins, such as p63, p40, and CK5/6, may be positive.
The results of immunohistochemistry help confirm that the tumour is anaplastic thyroid carcinoma and guide additional testing.
Molecular testing
Molecular testing, including next-generation sequencing (NGS), can be performed on tumour tissue to identify specific genetic changes (mutations) that help confirm the diagnosis and guide treatment. These tests look at the tumour’s DNA to identify changes in genes that are commonly altered in thyroid cancer.
Some of the most important genetic changes found in anaplastic thyroid carcinoma include:
-
BRAF p.V600E mutation: This mutation is found in many tumours that arise from papillary thyroid carcinoma. It is especially important because targeted therapy using BRAF and MEK inhibitors may be effective in treating tumours with this mutation.
-
RAS gene mutations (HRAS, NRAS, KRAS): These are early mutations commonly seen in follicular or poorly differentiated thyroid carcinoma, and they may be present in anaplastic thyroid carcinoma that developed from one of these tumour types.
-
TP53 mutation: TP53 is a tumour suppressor gene that helps control cell growth. Mutations in TP53 are common in anaplastic thyroid carcinoma and are associated with aggressive behaviour and poor prognosis.
-
TERT promoter mutation: This mutation is often seen in advanced thyroid cancers and is associated with a higher risk of spread and death. It may occur in conjunction with BRAF or RAS mutations.
-
PIK3CA and PTEN mutations: These genes are part of a signalling pathway that controls cell growth. Mutations in these genes are associated with tumour progression and may be targets for new therapies.
-
EIF1AX mutation: Found in a small percentage of anaplastic thyroid carcinomas and thought to contribute to tumour development.
-
Other mutations: Additional gene alterations observed in anaplastic thyroid carcinoma include changes in ATM, CDKN2A, CDKN1B, and genes of the SWI/SNF complex, as well as ALK and CTNNB1. Some tumours also show defects in DNA mismatch repair genes (such as MLH1, MSH2, and MSH6), which may predict benefit from immunotherapy.
These molecular findings are important because they can guide decisions about targeted therapy and clinical trials. For example, patients with a BRAF p.V600E mutation may benefit from BRAF/MEK inhibitors.
Tumour size
If the tumour is removed by surgery, it will be measured in three dimensions. The largest dimension is reported in your pathology report. Tumour size is important because larger tumours are more likely to invade nearby structures and spread to other parts of the body.
Extrathyroidal extension
Extrathyroidal extension means that the tumour has spread outside the thyroid gland and into the surrounding tissues in the neck. This is a common feature of anaplastic thyroid carcinoma and indicates more advanced disease. Tumour cells may grow into nearby muscles, the trachea, the esophagus, or blood vessels. This makes surgical removal more difficult and often limits treatment options.
There are two types of extrathyroidal extension:
-
Microscopic extrathyroidal extension: Tumour cells are found outside the thyroid only when examined under a microscope.
-
Macroscopic (gross) extrathyroidal extension: Tumour growth into surrounding tissues is visible to the surgeon during the operation or to the pathologist examining the specimen.
Macroscopic extrathyroidal extension is more serious and increases the tumour stage (pT). It is also associated with a worse prognosis.
Vascular invasion
Vascular invasion means that tumour cells have entered one or more blood vessels near the tumour. Once inside a blood vessel, the tumour cells can travel to distant parts of the body, such as the lungs, bones, or brain, where they can form metastases. Vascular invasion is commonly seen in anaplastic thyroid carcinoma and is an important feature that increases the risk of spread and worsens the prognosis.
Lymphatic invasion
Lymphatic invasion means that tumour cells have entered small lymphatic vessels, which are part of the body’s immune and fluid drainage system. From there, the tumour cells can travel to lymph nodes, where they may start new areas of tumour growth. Lymphatic invasion increases the risk of lymph node metastasis and is often seen in aggressive cancers like anaplastic thyroid carcinoma.
Margins
In pathology, a margin is the edge of tissue removed during tumour surgery. The margin status in a pathology report is important as it indicates whether the entire tumour was removed or if some was left behind. This information helps determine the need for further treatment.
Pathologists examine margins to check if tumour cells are at the tissue’s cut edge. A positive margin, where tumour cells are found, suggests that some may remain in the body. In contrast, a negative margin, with no tumour cells at the edge, suggests that the tumour was entirely removed. Some reports also measure the distance between the nearest tumour cells and the margin, even if all margins are negative.

Lymph nodes
Lymph nodes are small immune organs found throughout the body. Cancer cells can spread through lymphatic vessels from a tumour to lymph nodes. For this reason, lymph nodes are commonly removed and examined under a microscope to look for cancer cells. The movement of cancer cells from the tumour to another part of the body, such as a lymph node, is called metastasis.
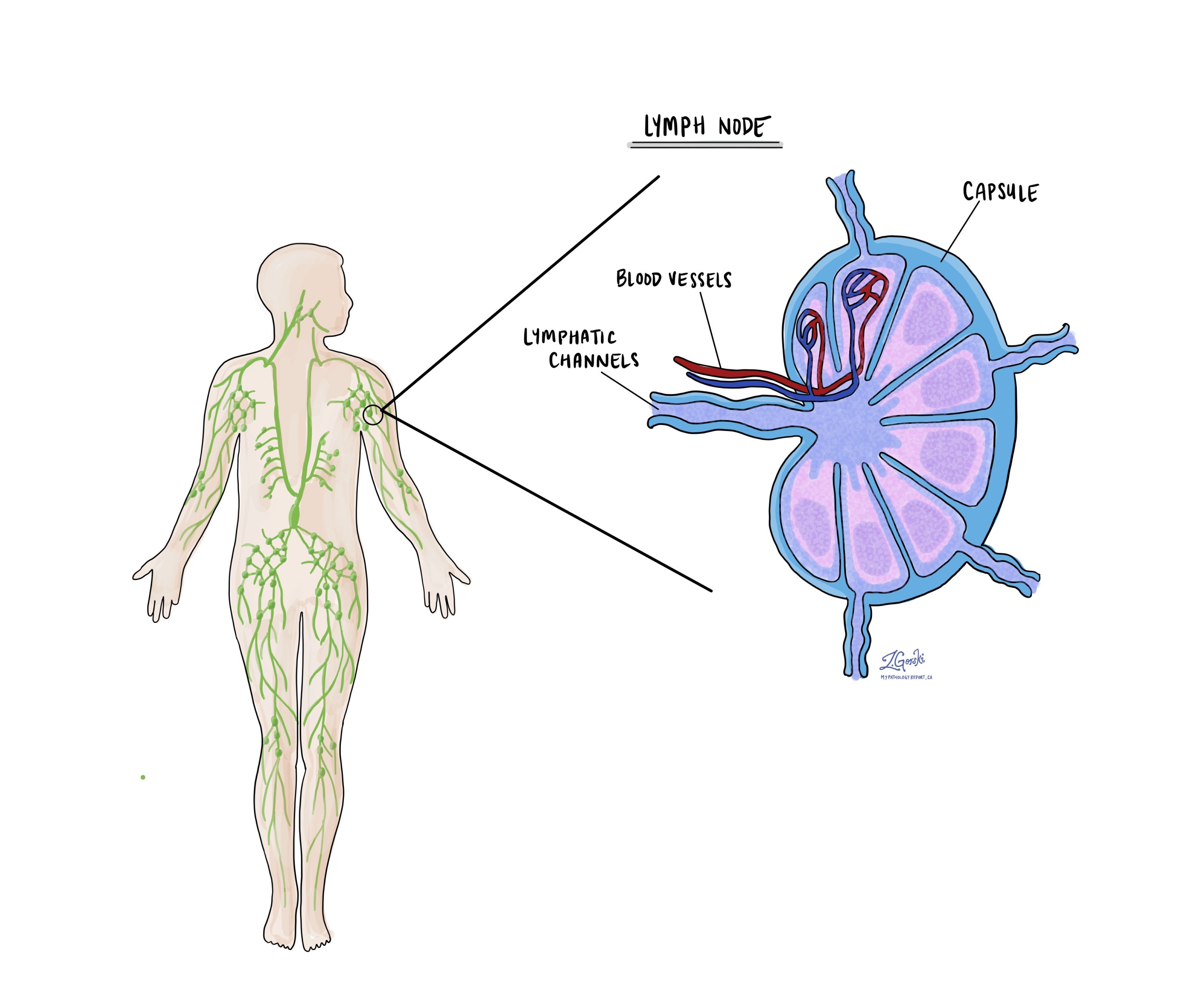
Cancer cells typically spread first to lymph nodes close to the tumour, although lymph nodes far away can also be involved. For this reason, the first lymph nodes removed are usually close to the tumour. Lymph nodes further away from the tumour are typically removed only if they are enlarged, and there is a high clinical suspicion that there may be cancer cells in them.
Neck dissections
A neck dissection is a surgical procedure that involves removing lymph nodes from the neck. The lymph nodes removed usually come from different areas of the neck, and each region is referred to as a level. The levels in the neck include 1, 2, 3, 4, and 5. Your pathology report will often describe the number of lymph nodes seen in each level sent for examination. Lymph nodes on the same side as the tumour are called ipsilateral, while those on the opposite side of the tumour are called contralateral.

How the lymph nodes will be described in your pathology report
If any lymph nodes are removed from your body, they will be examined under the microscope by a pathologist, and the examination results will be described in your report. “Positive” means that cancer cells were found in the lymph node. “Negative” indicates that no cancer cells were found. If cancer cells are found in a lymph node, the size of the largest group of cancer cells (often described as “focus” or “deposit”) may also be included in your report. Extranodal extension means that the tumour cells have broken through the capsule outside of the lymph node and spread into the surrounding tissue.
Why is the examination of lymph nodes important?
The examination of lymph nodes is important for two reasons. First, this information determines the pathologic nodal stage (pN). Second, the discovery of cancer cells in a lymph node increases the likelihood that cancer cells will be detected in other parts of the body in the future. As a result, your doctor will use this information when deciding if additional treatment, such as radioactive iodine, chemotherapy, radiation therapy, or immunotherapy, is required.
Pathologic stage (pTNM)
The pathologic stage for anaplastic thyroid carcinoma is determined using the TNM staging system, an internationally accepted classification system developed by the American Joint Committee on Cancer (AJCC). This system helps doctors understand how far the cancer has spread by looking at three main factors:
-
T (Tumour): The size of the tumour and whether it has grown into nearby tissues outside the thyroid gland.
-
N (Nodes): Whether the cancer has spread to nearby lymph nodes.
-
M (Metastasis): Whether the cancer has spread to distant parts of the body, such as the lungs or bones.
After examining the tumour and any lymph nodes removed during surgery, the pathologist assigns a number or letter to each of these categories. In general, higher numbers mean more advanced cancer, which may require more aggressive treatment and is associated with a less favorable prognosis. For anaplastic thyroid carcinoma, all cases are considered stage IV because of the tumour’s aggressive behaviour, but the exact substage (IVA, IVB, or IVC) depends on how far the cancer has spread.
Tumour stage (pT)
Anaplastic thyroid carcinoma is given a tumour stage between 1 and 4 based on its size and the presence of tumour cells outside of the thyroid.
- T1 – The tumour is less than or equal to 2 cm, and the cancer cells do not extend beyond the thyroid gland.
- T2 – The tumour is greater than 2 cm but less than or equal to 4 cm, and the cancer cells do not extend beyond the thyroid gland.
- T3 – The tumour is greater than 4 cm OR the cancer cells extend into the muscles outside of the thyroid gland.
- T4 – The cancer cells extend to structures or organs outside the thyroid gland, including the trachea, larynx, or esophagus.
Nodal stage (pN)
Anaplastic thyroid carcinoma is given a nodal stage of 0 or 1 based on the presence or absence of tumour cells in a lymph node and the location of the involved lymph nodes.
- N0 – No cancer cells were found in any of the lymph nodes examined.
- N1a – Cancer cells were found in one or more lymph nodes from levels 6 or 7.
- N1b – Cancer cells were found in one or more lymph nodes from levels 1 through 5.
- NX – No lymph nodes were sent to pathology for examination.
What is the prognosis for a person with anaplastic thyroid carcinoma?
Anaplastic thyroid carcinoma has a very poor prognosis. It is one of the most aggressive human cancers. Without treatment, the average survival is only a few months. Even with treatment, most people live less than one year after diagnosis. However, survival may be longer in people with:
-
Smaller tumours confined to the thyroid.
-
No distant metastasis.
-
Successful surgical removal of all visible tumour.
-
Tumours with certain genetic mutations (such as BRAF p.V600E) that respond to targeted therapy.
Newer treatments, including targeted therapies, immunotherapy, and multimodal treatment (surgery, radiation, and chemotherapy), are improving outcomes for some patients. Clinical trials are ongoing.
Questions to ask your doctor
-
What did my biopsy or pathology report show?
-
Has the cancer spread outside the thyroid gland?
-
Are there any lymph nodes or distant organs involved?
-
What stage is my cancer?
-
What treatments are available?
-
Can I have surgery to remove the tumour?
-
Are there targeted therapies available based on my tumour’s genetic changes?
-
Should I consider participating in a clinical trial?
-
What is the expected prognosis?
-
What symptoms should I watch for going forward?




